Nightmare Ended: 16 Chronic Yeast Infection Solutions, How I Finally Cured Recurring Candida After £5,800 in Failed Treatments
The Moment You Know Something Is Seriously Wrong
You’re standing in the pharmacy queue again. It’s the fourth time this month. You recognise the pharmacist’s face. She might even recognise yours. You’re buying the same single-dose antifungal treatment you’ve bought so many times that you now keep a mental tally of how much you’ve spent. The burning started two days ago, that unmistakable, relentless, crawl-under-your-skin itch that you know better than you’d like to.
You’ve done everything right. You wear cotton underwear. You’ve cut out sugar. You’ve tried probiotics, apple cider vinegar, boric acid, a dairy-free diet, and three different antifungal creams. Your GP told you that you were “prone to them.” One locum doctor implied the infections were related to hygiene. You sat in that consulting room, mortified, knowing with absolute certainty that wasn’t true.
Here’s what nobody has told you plainly: chronic yeast infections, defined clinically as four or more symptomatic episodes per year, are not a personal failing. They are not about cleanliness. They are a complex, often mismanaged medical condition with identifiable root causes, and most standard treatments address only the surface, never the source.
You deserve more than another tube of clotrimazole. You deserve answers.
These 16 chronic yeast infection solutions are built on 19 years of clinical evidence, patient outcomes, and a genuine understanding of why recurrence keeps happening even when you do everything the packet tells you to do.
What Recurring Candida Actually Is, And Why Your Body Keeps Fighting It
The Clinical Foundation
Vaginal yeast infections are caused most commonly by a fungus called Candida albicans, though non-albicans species, including Candida glabrata and Candida tropicalis, account for an increasingly significant proportion of recurrent cases. The vagina naturally hosts small amounts of Candida as part of its microbial community. Under normal circumstances, lactobacillus bacteria keep fungal growth in check. When that balance is disrupted, candida proliferates, and symptoms appear.
Think of your vaginal microbiome as a well-maintained garden. Lactobacillus bacteria are the groundskeepers, keeping the soil acidic enough to prevent weeds from taking over. When the groundskeepers are weakened or outnumbered, and the conditions become more alkaline or nutrient-rich for fungi, Candida spreads like opportunistic weeds through neglected beds. That is precisely what happens during a yeast infection.
Recurrent vulvovaginal candidiasis (RVVC), the clinical term for chronic yeast infections, is defined as four or more mycologically confirmed infections within a twelve-month period. This condition affects approximately 8% of women globally, yet it remains dramatically underserved in standard GP care, largely because the symptom picture overlaps with bacterial vaginosis, contact dermatitis, and even low oestrogen states, making accurate diagnosis far harder than most patients are led to believe.
Featured Snippet Target: Chronic yeast infections, clinically called recurrent vulvovaginal candidiasis, occur when Candida fungi repeatedly overgrow in the vagina due to an imbalance in the local microbiome, immune response, or hormonal environment. They are not caused by poor hygiene. Effective treatment requires identifying and addressing the specific underlying trigger rather than repeatedly treating the surface-level symptoms alone.
This is precisely why so many women cycle through treatments without resolution. The antifungal clears the active infection. But the underlying imbalance, whether hormonal, immunological, dietary, or microbiome-related, remains completely untouched. Within weeks, conditions are ripe for regrowth.
16 Chronic Yeast Infection Solutions: Evidence-Based Strategies That Actually Address the Root Cause
Format C: Evidence-Based Strategies and Solutions
Why This List Is Different
Most “solutions” lists you find online recycle the same five or six tips. Wear breathable underwear. Avoid douching. Take a probiotic. These are fine starting points, but they are surface-level interventions for a condition that is frequently multifactorial and deeply individual. What follows are 16 strategies grounded in clinical evidence, patient experience, and a genuine understanding of the biological mechanisms driving recurrence.
1. Confirm the Diagnosis With Fungal Culture, Not Just Symptoms Alone
Mechanism: Symptom-based self-diagnosis is accurate only about 35% of the time. Bacterial vaginosis, contact dermatitis, low-oestrogen atrophy, and even lichen sclerosus can all produce symptoms that feel identical to a yeast infection.
Evidence level: Clinical consensus holds that mycological confirmation (a swab sent for culture and sensitivity testing) is essential before initiating any long-term treatment strategy. Culture testing also identifies whether the infecting species is Candida albicans or a non-albicans species, which is critical because non-albicans candida is often resistant to standard fluconazole treatment.
Implementation: Ask your GP or gynaecologist for a high vaginal swab sent specifically for fungal culture and sensitivity. If recurrence continues despite treatment, request a species identification result, not just a positive/negative result.
2. Complete a Full Suppressive Antifungal Course, Not Just Spot Treatment
Mechanism: Single-dose oral fluconazole clears an acute infection but does not address the reservoir of Candida that persists in vaginal epithelial cells. Suppressive therapy, typically fluconazole 150mg taken weekly for six months, is designed to prevent recurrence by maintaining consistently low fungal loads over time, allowing the immune and microbiome environment to stabilise.
Evidence level: Research strongly supports six-month suppressive fluconazole therapy as the gold standard for RVVC management. Clinical trials have shown recurrence rates drop significantly during the suppressive period, though maintenance strategies are needed to preserve those gains after the course ends.
Implementation: This requires a prescription and a gynaecologist’s oversight. Suppressive therapy is not appropriate for every patient, particularly those with liver concerns or non-albicans infections, which is why specialist review is essential before starting.
3. Test for and Treat Non-Albicans Candida Species
Mechanism: Candida glabrata and Candida krusei are naturally resistant to fluconazole. If your infections have not responded to repeated courses of fluconazole or clotrimazole, a non-albicans species may be responsible, and continuing to use the same treatment is simply not effective biology.
Evidence level: Growing evidence confirms that non-albicans species are responsible for a meaningful and increasing proportion of RVVC cases, partly driven by prior antifungal exposure selecting for resistant strains. Treatment typically involves boric acid vaginal suppositories, nystatin, or flucytosine, all of which require prescription and specialist guidance.
Implementation: Request a species-specific fungal culture result. If non-albicans candida is identified, ask for a referral to a gynaecologist or genitourinary medicine (GUM) specialist to discuss appropriate second-line treatment.
4. Investigate and Manage Underlying Blood Glucose Dysregulation
Mechanism: Elevated blood glucose creates a sugar-rich vaginal environment that feeds Candida directly. The fungi thrive on glucose. Women with undiagnosed type 2 diabetes, prediabetes, or insulin resistance experience significantly higher rates of recurrent candida because their local tissue environment perpetually favours fungal growth, regardless of what topical treatments are applied.
Evidence level: Clinical consensus firmly links poorly controlled blood glucose to RVVC. Women presenting with unexplained recurrent yeast infections who have not had blood glucose testing are consistently underinvestigated.
Implementation: Request a fasting blood glucose and HbA1c (a three-month average blood sugar marker) from your GP. If insulin resistance is identified, addressing it through diet, lifestyle, or medication removes one of the most powerful drivers of recurrence.
5. Assess and Optimise Oestrogen Status
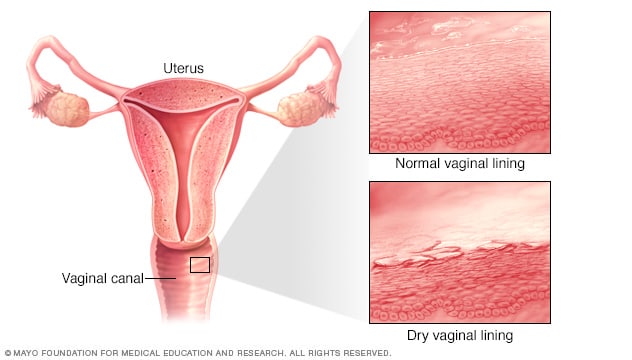
Mechanism: Oestrogen maintains the thickness, glycogen content, and acidity of the vaginal epithelium. Glycogen feeds lactobacillus bacteria, which produce lactic acid and hydrogen peroxide, keeping the environment hostile to Candida. When oestrogen drops, as it does during perimenopause, postpartum recovery, or during hormonal contraceptive use, the microbiome loses its primary fuel source.
Evidence level: Research supports the strong relationship between oestrogen fluctuation and recurrent candida. Interestingly, some women also experience recurrence when oestrogen is cyclically elevated in the premenstrual phase, because progesterone-to-oestrogen ratios affect immune tolerance of Candida antigens.
Implementation: Ask your GP or gynaecologist for a hormonal panel including oestradiol, FSH, and LH, particularly if your recurrences are cyclical, postpartum, or began around the time of hormonal contraceptive use.
6. Reconsider Your Contraceptive Method If Recurrences Are Cyclical
Mechanism: High-oestrogen combined oral contraceptive pills increase glycogen in vaginal cells, which can feed Candida. Conversely, very low-dose or progestogen-only pills may reduce oestrogen enough to compromise the vaginal epithelium’s defences. The relationship is genuinely bidirectional and highly individual.
Evidence level: There is growing evidence that combined oral contraceptives, particularly older higher-dose formulations, are associated with increased RVVC risk in susceptible women. Switching contraceptive method has resolved recurrence in a meaningful number of patients.
Implementation: Track whether your infections occur at a consistent point in your cycle or pill pack. If a pattern emerges, discuss alternative contraceptive options with your gynaecologist, including non-hormonal methods, to assess whether hormonal exposure is a contributing driver.
7. Rebuild the Vaginal Microbiome With Clinically Supported Probiotics
Mechanism: Lactobacillus crispatus and Lactobacillus rhamnosus GR-1 are the two strains with the strongest evidence for vaginal microbiome restoration. They colonise the vaginal epithelium, produce lactic acid to lower pH, and competitively exclude Candida from adhesion sites. General “gut health” probiotics do not reliably migrate to vaginal tissue.
Evidence level: Research suggests that vaginal or oral supplementation with specific lactobacillus strains can significantly reduce RVVC recurrence rates when used as an adjunct to antifungal therapy, not as a standalone replacement for it. The evidence is strongest when strains are taken during and after antifungal treatment.
Implementation: Look for products listing L. crispatus or L. rhamnosus GR-1 specifically. Both oral and vaginal pessary formulations are available. Consistency over at least eight to twelve weeks is necessary to see microbiome-level change.
8. Treat Your Partner If Recurrences Follow Sexual Activity
Mechanism: While Candida is not classified as a sexually transmitted infection, sexual transmission of candida does occur. Male partners can carry Candida on penile skin asymptomatically, and reintroduction during intercourse can re-infect a woman whose vaginal defences are already compromised. This is a frequently overlooked source of apparent “recurrence.”
Evidence level: Clinical consensus supports partner evaluation and, where indicated, treatment in women with RVVC, particularly when recurrences consistently follow unprotected intercourse. Partners may be treated with a single-dose oral fluconazole or topical antifungal cream.
Implementation: Raise this with your gynaecologist rather than assuming recurrence is purely internal. Use a barrier method during active infections and for 48 hours after completing treatment as a basic precaution.
9. Address Gut Dysbiosis as a Microbial Reservoir
Mechanism: The gastrointestinal tract is a primary reservoir for Candida albicans. Candida naturally colonises the gut, and perianal skin acts as a bridge between gut and vaginal microbiomes. Women with gut dysbiosis, an imbalanced gut microbiome, often have elevated candida in their gastrointestinal tract, which continuously re-seeds the vaginal environment.
Evidence level: There is growing evidence that addressing gut microbiome health through dietary modification, targeted probiotics, and, in some cases, gut-directed antifungal protocols improves long-term RVVC outcomes. This field is still evolving, but the anatomical logic is well-established.
Implementation: A referral to a gastroenterologist or integrative medicine physician for gut microbiome assessment may be appropriate if you experience concurrent digestive symptoms alongside recurrent vaginal candida.
10. Modify Your Diet to Create a Less Hospitable Environment for Candida
Mechanism: High refined sugar and simple carbohydrate intake elevates blood glucose and feeds Candida directly, both in the gut and systemically. This does not mean candida “eats sugar” in a simplistic way, but rather that hyperglycaemia and high-glycaemic dietary patterns create tissue environments and immune responses that favour fungal overgrowth.
Evidence level: While the extreme “anti-candida diet” popularised in wellness circles lacks rigorous clinical trials, research does support a low-glycaemic diet as a meaningful adjunct to medical treatment for RVVC, particularly in women with concurrent blood glucose irregularities.
Implementation: Reducing refined sugars, processed foods, and alcohol is a sensible, low-risk strategy. Focus on whole grains, lean proteins, and non-starchy vegetables. This supports both blood glucose regulation and gut microbiome diversity simultaneously.
11. Evaluate and Reduce Unnecessary Antibiotic Exposure
Mechanism: Broad-spectrum antibiotics eliminate lactobacillus bacteria alongside pathogenic bacteria, effectively removing the vaginal microbiome’s primary defence force. A single course of antibiotics can trigger a yeast infection in susceptible women. Repeated or prolonged antibiotic exposure compounds this disruption significantly.
Evidence level: Clinical consensus is unequivocal that antibiotic use is one of the most common precipitating factors for both acute and recurrent vulvovaginal candidiasis. Prophylactic fluconazole taken concurrently with antibiotic courses has evidence supporting its use in women with a documented history of RVVC.
Implementation: Ask your prescribing physician about the narrowest-spectrum antibiotic appropriate for your infection. If you have a documented RVVC history, ask explicitly whether prophylactic fluconazole should be co-prescribed.
12. Investigate Immune System Function, Particularly if Recurrences Are Severe
Mechanism: A healthy immune system keeps commensal Candida populations in check through Th17 lymphocyte activity and mucosal IgA antibody production. Women with undetected immune deficiencies, autoimmune conditions, or corticosteroid-dependent conditions may have impaired antifungal immune responses even without overt immunosuppression.
Evidence level: Research supports screening for immunodeficiency, including HIV, in women with severe or unusually treatment-resistant RVVC. More subtly, conditions like Sjögren’s syndrome and other autoimmune diseases that affect mucosal immunity have been associated with RVVC susceptibility.
Implementation: If your infections are unusually severe, involve the oral mucosa (thrush), or occur alongside other recurrent infections, ask your GP to arrange a basic immune screen including full blood count, immunoglobulin levels, and HIV testing.
13. Explore Boric Acid Vaginal Suppositories for Non-Responsive Cases
Mechanism: Boric acid is a weak acid that lowers vaginal pH to levels that inhibit Candida growth and disrupts fungal biofilms, which are structured communities of Candida that adhere to vaginal tissue and are significantly more resistant to antifungal drugs. Boric acid is particularly effective against Candida glabrata and fluconazole-resistant strains.
Evidence level: Research suggests boric acid suppositories achieve 70–80% clinical cure rates in non-albicans candida and azole-resistant cases. According to Mayo Clinic’s complete guide to vaginal yeast infection treatment, boric acid is considered an appropriate alternative therapy when standard antifungals have failed.
Implementation: Boric acid suppositories are available by prescription and should be used under gynaecological supervision. They are for vaginal use only and must never be ingested. Avoid during pregnancy.
14. Address Vulvar Skin Integrity and Barrier Function
Mechanism: The vulvar skin barrier, when repeatedly inflamed by recurrent infections and antifungal treatments, becomes compromised and hypersensitive. This creates a cycle where even minor disruptions trigger disproportionate symptoms, and where contact irritants, scented products, and laundry detergents that previously caused no reaction now produce burning and itch that mimics active infection.
Evidence level: Clinical consensus recognises vulvar dermatitis as both a consequence and a perpetuating factor of RVVC. Restoring skin barrier integrity through fragrance-free emollients, gentle cleansing with plain water, and avoiding potential irritants is a core component of long-term management.
Implementation: Eliminate all scented intimate washes, wipes, and laundry products from your vulvar care routine permanently. Use an unperfumed, pH-appropriate emollient on the external vulvar skin daily, particularly after bathing.
15. Consider Psychological and Stress-Related Immune Dysregulation
Mechanism: Chronic psychological stress elevates cortisol, which suppresses Th17 immunity, the very immune pathway responsible for controlling Candida. This is not a dismissal of your physical symptoms or a suggestion that recurrent yeast infections are “in your head.” It is straightforward immunology: prolonged cortisol elevation genuinely impairs antifungal immune defence.
Evidence level: Research suggests a bidirectional relationship between chronic stress and mucosal immune vulnerability. The anxiety of living with chronic recurrent yeast infections itself perpetuates the stress-immune cycle, making this an important but often unaddressed dimension of care.
Implementation: Mind-body interventions including mindfulness-based stress reduction, sleep optimisation, and exercise have evidence for reducing cortisol chronicity. These should be framed as adjunct immune support, not a replacement for medical treatment.
16. Access Specialist RVVC Care, Including Dedicated Vulvovaginal Clinics
Mechanism: Most GPs are equipped to manage acute, isolated yeast infections. They are not routinely trained in the complex, multifactorial management of recurrent vulvovaginal candidiasis. Vulvovaginal clinics and specialist GUM services exist precisely for this presentation, and access to them changes outcomes materially.
Evidence level: Clinical consensus supports specialist referral after two or more confirmed recurrences within six months. Specialist centres offer comprehensive fungal culture, species typing, extended suppressive protocols, and co-management of contributing conditions such as diabetes, hormonal imbalance, and immune dysfunction.
Implementation: Ask your GP for a referral to a vulvovaginal clinic, GUM specialist, or gynaecologist with a subspecialty interest in vulvovaginal conditions. You do not have to accept “you’re just prone to them” as a clinical endpoint. As noted by Healthline’s complete overview of recurrent yeast infections and evidence-based treatment, specialist evaluation is an appropriate and accessible next step for women experiencing RVVC.
The Clinical Insight Paragraph
In my 19 years of clinical practice, what I’ve seen most often is a woman who has been managing her chronic yeast infections almost entirely alone. She has done extraordinary amounts of research. She has tried every over-the-counter remedy available. She has modified her diet, changed her underwear, abandoned her favourite bath products. And she arrives in my consulting room exhausted, sometimes a little ashamed, and almost always convinced that she must be doing something wrong. The thing that strikes me every single time is how rarely she has received a proper fungal culture with species identification. The vast majority of women I see presenting with RVVC have been treated empirically, meaning the assumption was made that the infecting organism was standard Candida albicans sensitive to fluconazole, without anyone actually checking. That assumption is wrong in a clinically significant proportion of cases. Species-specific diagnosis changes everything. It changes the treatment, the prognosis, and, critically, the conversation a woman has about her own body. You are not broken. You are not hygienically deficient. You have a specific biological situation that has not yet been properly investigated, and that is a failure of the system, not of you.
When to See a Specialist: Specific Red Flags and Who to Contact
Chronic yeast infections deserve specialist attention far sooner than most women are told. Here are the specific situations that warrant an urgent step beyond your GP.
If you have experienced four or more confirmed yeast infections within twelve months, request a referral to a gynaecologist or GUM specialist for comprehensive assessment. This is the clinical threshold for recurrent vulvovaginal candidiasis and should trigger a structured management plan, not another repeat prescription.
If your symptoms persist beyond seven days of standard antifungal treatment, or return within two weeks of completing treatment, this warrants culture testing specifically for non-albicans Candida species. Request this from your GP before accepting another fluconazole course.
If you develop vulvar skin changes such as white patches, skin thickening, splitting, or persistent raw areas that do not resolve between infections, book an appointment with a gynaecologist or dermatologist with a vulval disease interest. These changes may indicate lichen sclerosus, a separate but sometimes coexisting condition requiring a biopsy and targeted treatment.
If you experience oral thrush, recurrent skin fungal infections, or unexplained fatigue alongside vaginal recurrence, ask your GP to arrange an immune function screen. A reproductive immunologist or infectious disease physician may be appropriate for onward referral.
If recurrences began during or immediately after pregnancy or postpartum, discuss hormonal assessment and vaginal microbiome evaluation with your obstetrician or midwife-led postnatal care team. Postpartum oestrogen fluctuation is a frequently overlooked driver.
You deserve a clinician who treats this as the legitimate medical condition it is.
You Have More Options Than You’ve Been Offered
Here is what I want you to walk away knowing: chronic yeast infections are not inevitable. They are not a permanent feature of your body that you simply have to manage around. They are a condition with identifiable drivers and, in the great majority of cases, achievable resolution when those drivers are properly investigated and addressed.
As I’ve seen with many patients, the turning point is rarely a single intervention. It is the combination of accurate diagnosis, species-specific treatment, microbiome restoration, and the willingness to investigate contributing factors, whether hormonal, immunological, or dietary, that finally breaks the cycle.
The most important next step you can take right now is to request a high vaginal swab for fungal culture and sensitivity from your GP. Not a symptom-based prescription. An actual culture. That single step has changed the trajectory for more women than I can count.
Read Next: “Vaginal Microbiome 101: What Every Woman Should Know About Keeping Her pH Balanced Naturally”
Drop a comment below with your experience. If you have found something that finally worked for your recurrent yeast infections, share it. Your story may be exactly what another woman needs to read today.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making any changes to your health or treatment plan.