Revolutionary: 12 Vaginal Rejuvenation Procedures Compared, Your $18,000 Investment Complete Breakdown
You deserve to know exactly what you’re paying for before a single dollar leaves your bank account. If you’ve been quietly researching vaginal rejuvenation at 2 a.m. with your phone screen dimmed, you’re not alone, and you’re not being vain.
Introduction: Why Women Are Investing Thousands in Vaginal Rejuvenation (And Why Nobody Talks About It)
Let’s cut through the silence right now. Vaginal rejuvenation is one of the fastest growing segments in women’s health, yet most women still whisper about it like it’s a secret they should be ashamed of. In 2023, the American Society of Plastic Surgeons reported a 30% increase in vaginal rejuvenation consultations compared to just five years earlier. That’s not a trend. That’s a movement.
Here’s the truth that nobody puts on a billboard. After childbirth, during perimenopause, after menopause, or simply as a result of aging and gravity doing what gravity does, your vaginal and vulvar tissues change. They lose collagen. They lose elasticity. The pelvic floor muscles that once held everything in place start letting things slip, literally.
And the consequences? They’re not cosmetic footnotes. We’re talking about urinary incontinence that makes you cross your legs every time you sneeze. Reduced sexual sensation that makes intimacy feel like a chore instead of a connection. Vaginal dryness so persistent that even your most expensive lubricant feels like a temporary band-aid. Pelvic organ prolapse that creates a constant heaviness you can’t shake.
These are quality of life issues. These are relationship issues. These are confidence issues. And for millions of women, they’re everyday realities that go unaddressed because the medical establishment has historically been slow to take women’s intimate health complaints seriously.
The good news? The landscape has changed dramatically. Today, there are more vaginal rejuvenation procedures available than ever before, ranging from completely nonsurgical options you can do on a lunch break to full surgical reconstructions that deliver permanent structural change. The investment ranges from a few hundred dollars to well over $18,000 when you factor in multiple sessions, follow-up treatments, and complementary procedures.
But here’s where it gets complicated. Not all procedures are created equal. Some work brilliantly for one concern and do absolutely nothing for another. Some require zero downtime while others need weeks of recovery. Some are backed by robust clinical evidence, and frankly, some are riding more on marketing hype than peer-reviewed research.
That’s exactly why I’ve put together this comprehensive comparison. By the time you finish reading, you’ll understand all 12 major vaginal rejuvenation procedures available today, know exactly what each one costs, understand what each one can and cannot do, and most importantly, you’ll be equipped to have an informed, confident conversation with your healthcare provider.
No more going into consultations blind. No more nodding along while a doctor throws acronyms at you. No more feeling pressured into a procedure because a med-spa had a compelling Instagram ad.
This is your body. This is your money. This is your decision. Let’s make sure it’s a well-informed one.
1. Vaginoplasty: The Gold Standard Surgical Vaginal Rejuvenation Procedure Compared to All Others
When most people hear “vaginal rejuvenation,” vaginoplasty is what comes to mind first. It’s the most established, most invasive, and arguably most transformative surgical option available. Among all vaginal rejuvenation procedures compared in this guide, vaginoplasty delivers the most dramatic structural change.
Vaginoplasty is a surgical procedure that tightens the vaginal canal by removing excess vaginal lining and tightening the surrounding soft tissues and muscles. Think of it like this: if your vaginal canal were a hallway, vaginoplasty essentially narrows that hallway by bringing the walls closer together and reinforcing the structural supports. The procedure is performed under general anesthesia or regional anesthesia, typically takes one to two hours, and is done by a board-certified gynecologic surgeon or plastic surgeon with specialized training.
What Vaginoplasty Actually Involves
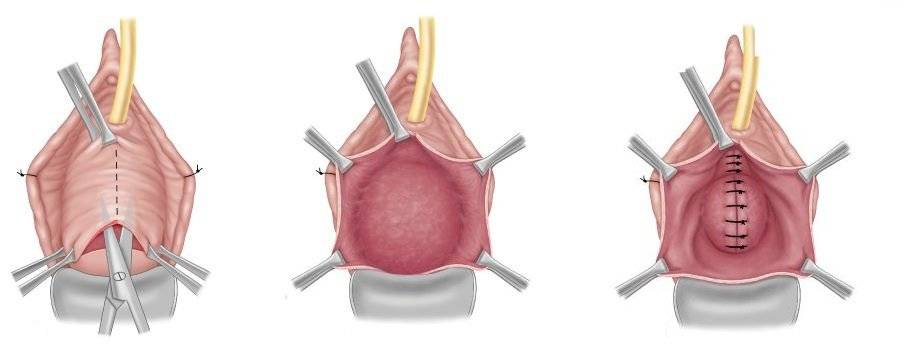
The surgeon makes incisions inside the vaginal canal, removes a pie-shaped wedge of excess tissue, then sutures the remaining tissue together tightly. In many cases, the surgeon also repairs or tightens the levator ani muscles, which are the deep pelvic floor muscles that form the primary support structure for the vaginal canal.
The sutures used are typically absorbable, meaning they dissolve on their own over several weeks. Some surgeons also address the perineum (the area between the vaginal opening and the anus), which is often the site of tearing during childbirth. This component is sometimes called perineoplasty and may be performed alongside vaginoplasty as a combined procedure.
Cost Breakdown for Vaginoplasty
This is where your wallet feels it. Vaginoplasty typically ranges from $5,000 to $12,000 depending on geographic location, surgeon experience, facility fees, and anesthesia costs. In major metropolitan areas like New York, Los Angeles, or Miami, you can expect to be on the higher end of that range.
Here’s what that number typically includes:
- Surgeon’s fee: $3,000 to $8,000
- Anesthesia: $500 to $1,500
- Facility/operating room fee: $1,000 to $2,500
- Pre-op lab work and consultations: $200 to $500
- Post-op follow-up visits: Usually included in the surgeon’s fee
- Prescription medications (pain management, antibiotics): $50 to $150
Insurance almost never covers vaginoplasty when performed for rejuvenation purposes. However, if the procedure is medically necessary due to pelvic organ prolapse or significant structural damage from childbirth, some insurers will cover a portion. You’ll need pre-authorization documents and a letter of medical necessity from your physician.
Recovery Timeline and What to Expect
Recovery from vaginoplasty is no walk in the park, and anyone who tells you otherwise is selling something. Here’s the honest timeline:
- Week 1: Significant swelling, bruising, and discomfort. Most women need prescription pain medication for the first 3 to 5 days. Walking is encouraged but should be gentle. No sitting for prolonged periods.
- Weeks 2 to 3: Swelling begins to subside. You can usually return to desk work. Avoid lifting anything heavier than 10 pounds.
- Weeks 4 to 6: Most swelling resolved. Sutures fully dissolved. Light exercise can resume.
- Week 6 to 8: Sexual intercourse can typically resume, but many women wait until the 8-week mark for comfort. Your surgeon will clear you at a follow-up appointment.
- Months 3 to 6: Final results become apparent as tissues fully heal and settle.
Who Is the Ideal Candidate?
Vaginoplasty works best for women who experience:
- Significant vaginal laxity after one or more vaginal deliveries
- Reduced sexual sensation related to structural looseness
- A feeling of “openness” or reduced friction during intercourse
- Mild to moderate pelvic organ prolapse (when combined with prolapse repair)
- Persistent dissatisfaction with nonsurgical treatments that haven’t delivered adequate results
It’s important to note that vaginoplasty is not designed to enhance the external appearance of the vulva. That’s a separate procedure (labiaplasty, which we’ll cover shortly). It also doesn’t address vaginal dryness, hormonal changes, or urinary incontinence on its own, though the muscle tightening component can have secondary benefits for mild stress incontinence.
Risks and Considerations
Every surgical procedure carries risks. For vaginoplasty, these include:
- Infection (risk approximately 1% to 3%)
- Bleeding or hematoma
- Scarring that may cause pain or tightness
- Over-tightening (which can make intercourse painful)
- Changes in sensation (usually temporary, rarely permanent)
- Reaction to anesthesia
- Deep vein thrombosis (rare but serious)
Choosing a board-certified surgeon with specific experience in vaginal rejuvenation surgery is critical. This is not the procedure to bargain-hunt for. Ask how many vaginoplasties the surgeon performs annually, request before-and-after photos, and speak with previous patients if possible.
2. Labiaplasty: The Most Popular Cosmetic Vaginal Rejuvenation Procedure Compared by Volume
Labiaplasty has been the single most requested female genital cosmetic surgery worldwide for over a decade. When we look at vaginal rejuvenation procedures compared by raw volume, labiaplasty dominates, with over 12,000 procedures performed annually in the United States alone, according to ASPS data.
Unlike vaginoplasty, which addresses the internal vaginal canal, labiaplasty focuses on the external anatomy, specifically the labia minora (inner lips) and sometimes the labia majora (outer lips). The goal is to reduce, reshape, or correct asymmetry in labial tissue that causes physical discomfort, self-consciousness, or both.
Understanding What Drives Women to Labiaplasty
Let’s dispel a myth right now. The majority of women seeking labiaplasty are not doing it because of unrealistic beauty standards or pornography influence, though critics love to make that claim. Research published in the Journal of Sexual Medicine found that the primary motivations for labiaplasty are functional and physical, not purely aesthetic.
Common reasons include:
- Chronic discomfort during exercise, cycling, or horseback riding
- Irritation or chafing from clothing, especially tight jeans, leggings, or swimwear
- Pain or pulling sensation during sexual intercourse
- Hygiene concerns related to excess tissue trapping moisture and causing recurrent infections
- Visible asymmetry that causes psychological distress
- Post-childbirth changes that resulted in stretched or torn labial tissue
Surgical Techniques
Two primary techniques dominate labiaplasty:
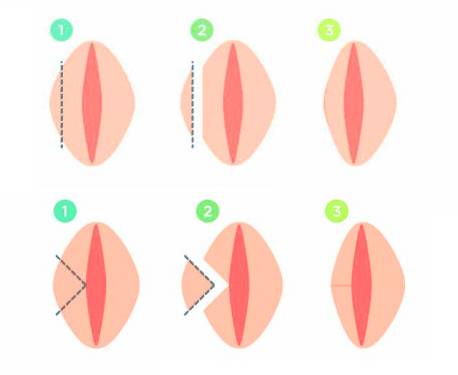
Trim technique: The surgeon removes the excess tissue along the edge of the labia minora, creating a neater, more defined labial border. This is the most straightforward approach and the one most commonly performed. It works well for women who want to remove the darker, irregular outer edge of the labia.
Wedge technique: Instead of trimming the edge, the surgeon removes a V-shaped or pie-shaped wedge from the thickest part of the labia and sutures the remaining edges together. This preserves the natural labial border and edge color, which some women prefer for a more natural appearance.
Both techniques are typically performed under local anesthesia with sedation, though general anesthesia is sometimes used. The procedure takes 45 minutes to an hour.
Cost Breakdown for Labiaplasty
Labiaplasty costs range from $3,000 to $8,000, with the national average sitting around $4,500 to $5,500.
- Surgeon’s fee: $2,500 to $6,000
- Anesthesia (local with sedation): $300 to $800
- Facility fee: $500 to $1,500
- Follow-up appointments: Typically included
Like vaginoplasty, labiaplasty is almost always classified as elective cosmetic surgery and is not covered by insurance. The exception is when excess labial tissue is causing documented, recurrent medical problems such as chronic infections, significant pain, or interference with urinary function.
Recovery and Results
Recovery from labiaplasty is generally faster and less intense than vaginoplasty:
- Days 1 to 3: Swelling and tenderness. Ice packs and loose clothing are your best friends. Most women manage pain with over-the-counter medications plus a short course of prescription pain relief.
- Week 1: Swelling peaks, then begins to subside. Light walking is encouraged.
- Weeks 2 to 3: Most women return to work. Swelling continues to decrease.
- Week 4 to 6: Exercise can gradually resume. Sexual activity is typically cleared at the 6-week mark.
- Months 3 to 6: Final cosmetic result is visible as all swelling resolves and scars mature.
Patient satisfaction rates for labiaplasty are exceptionally high, consistently above 90% in published studies. Most women report improved comfort, increased confidence, and resolution of the physical symptoms that drove them to seek the procedure.
Risks Specific to Labiaplasty
- Asymmetry (the most common reason for revision)
- Over-resection (removing too much tissue, which cannot be reversed)
- Scarring
- Temporary or permanent changes in sensation
- Wound dehiscence (sutures opening prematurely)
- Chronic dryness at the incision edges
3. MonaLisa Touch: Fractional CO2 Laser Vaginal Rejuvenation Procedures Compared for Menopausal Symptoms
Now we shift gears from surgical to nonsurgical, and MonaLisa Touch is perhaps the most well-known laser-based vaginal rejuvenation procedure on the market. When evaluating vaginal rejuvenation procedures compared for addressing menopausal and postmenopausal symptoms specifically, MonaLisa Touch consistently emerges as a frontrunner.
MonaLisa Touch uses fractional CO2 (carbon dioxide) laser energy to create controlled micro-injuries in the vaginal wall tissue. These tiny, precise wounds trigger the body’s natural healing response, which involves producing new collagen, elastin, and hyaluronic acid, the three building blocks of healthy, resilient vaginal tissue.
How the Procedure Works
The treatment is performed in a gynecologist’s office and takes approximately 5 minutes of actual laser application time. Here’s the step-by-step:
- No anesthesia is typically required, though some providers apply a topical numbing cream for comfort.
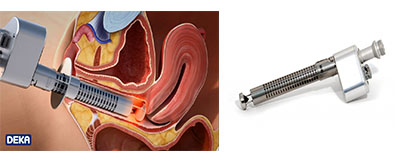
- A slim laser probe (about the size of a standard speculum) is inserted into the vaginal canal.
- The probe delivers 360-degree fractional CO2 laser energy to the vaginal walls.
- The probe is slowly rotated and withdrawn, treating the entire vaginal canal.
- The external vulvar area can also be treated in the same session if needed.
Most women describe the sensation as a mild vibration or warmth, not pain. The entire office visit, including prep and treatment, usually takes 15 to 30 minutes.
The Science Behind MonaLisa Touch
According to the Mayo Clinic’s overview of vaginal dryness treatments, the decline in estrogen that occurs during menopause leads to vaginal atrophy, a condition characterized by thinning, drying, and inflammation of the vaginal walls. This affects approximately 50% of postmenopausal women, though the actual number is likely higher because many women don’t report symptoms.
MonaLisa Touch addresses vaginal atrophy at the tissue level by:
- Stimulating fibroblast activity (fibroblasts are the cells that produce collagen)
- Increasing vascularity (more blood flow means healthier tissue)
- Restoring the vaginal epithelium (the mucosal lining) to a pre-menopausal thickness
- Boosting natural lubrication by rehydrating the tissue from within
- Normalizing vaginal pH, which helps prevent recurrent infections
Cost and Treatment Protocol
MonaLisa Touch is not a one-and-done treatment. The standard protocol involves:
- 3 initial treatments spaced 6 weeks apart
- Annual maintenance treatments (1 to 2 per year) to sustain results
Each treatment costs $700 to $1,500, depending on your provider and geographic location. That puts the initial series at $2,100 to $4,500, with annual maintenance adding $700 to $1,500 per year.
Over a 5-year period, your total investment could range from $5,600 to $10,500. That’s significant, especially since MonaLisa Touch is rarely covered by insurance.
Who Benefits Most from MonaLisa Touch?
This procedure is particularly well-suited for:
- Postmenopausal women experiencing vaginal dryness, burning, or itching
- Women who cannot or choose not to use estrogen-based hormone therapy
- Breast cancer survivors on aromatase inhibitors (which accelerate vaginal atrophy)
- Women experiencing painful intercourse (dyspareunia) due to tissue thinning
- Women with recurrent urinary tract infections related to vaginal pH changes
- Women seeking mild improvement in vaginal tightness (though the tightening effect is modest compared to surgery)
What MonaLisa Touch Cannot Do
Let’s be clear about limitations. MonaLisa Touch is not a replacement for vaginoplasty if you have significant structural laxity. It will not correct pelvic organ prolapse. It will not dramatically change the appearance of your labia. And its effects on urinary incontinence, while sometimes positive, are secondary and inconsistent.
Think of MonaLisa Touch as a tissue quality treatment, not a structural treatment. It makes the tissue healthier, plumper, more hydrated, and more elastic. But it doesn’t physically tighten muscles or remove excess tissue.
4. ThermiVa: Radiofrequency Vaginal Rejuvenation Procedures Compared for Comfort and Convenience
If MonaLisa Touch is the laser queen, ThermiVa is the radiofrequency rival. Among nonsurgical vaginal rejuvenation procedures compared for patient comfort, ThermiVa often wins because it involves no laser, no incisions, no anesthesia, and essentially zero pain.
ThermiVa uses temperature-controlled radiofrequency (RF) energy delivered via a small S-shaped wand. The wand is applied to both external vulvar tissue and internal vaginal tissue, delivering gentle heat that stimulates collagen remodeling and tissue tightening.
The ThermiVa Experience
Here’s what a typical ThermiVa session looks like:
- You’ll lie in a comfortable position, similar to a regular gynecological exam.
- The provider applies the small ThermiVa wand to the external labial tissue first, gently heating the area.
- The wand is then inserted into the vaginal canal, treating the internal tissue.
- The entire process takes approximately 30 minutes.
- Most women describe the sensation as a warm, pleasant massage. Seriously. No joke.
- You walk out the door and resume normal activities immediately.
There is no downtime. None. You can exercise, work, and even have sexual intercourse the same day. That’s a massive selling point for busy women who can’t afford weeks of recovery.
What ThermiVa Treats
ThermiVa’s primary effects include:
- Mild to moderate vaginal tightening through collagen contraction and remodeling
- Improved labial appearance by plumping and tightening external vulvar skin
- Enhanced natural lubrication through tissue rejuvenation
- Reduced symptoms of mild stress urinary incontinence (leaking during coughing, sneezing, or exercise)
- Improved sexual sensation and satisfaction reported by many patients
Cost and Treatment Protocol
The standard ThermiVa protocol includes:
- 3 treatments spaced approximately 1 month apart
- Maintenance treatments every 9 to 12 months
Each session costs $1,500 to $3,000, placing the initial series at $4,500 to $9,000. Annual maintenance adds $1,500 to $3,000 per year.
Over 5 years, your total investment could reach $10,500 to $21,000, making ThermiVa potentially more expensive than surgical vaginoplasty over the long run. That’s a critical consideration that many med-spas conveniently leave out of their marketing.
ThermiVa vs. MonaLisa Touch: Head to Head
Since these two procedures compete directly for the same patient population, let’s compare them clearly:
| Feature | ThermiVa | MonaLisa Touch |
|---|---|---|
| Technology | Radiofrequency (RF) | Fractional CO2 Laser |
| Treatment Time | 30 minutes | 15 to 30 minutes |
| Pain Level | None to minimal | Minimal to mild |
| Anesthesia | None required | None (topical numbing optional) |
| Downtime | Zero | 2 to 3 days (avoid intercourse 48 hours) |
| Initial Sessions | 3 | 3 |
| Cost Per Session | $1,500 to $3,000 | $700 to $1,500 |
| Total Initial Cost | $4,500 to $9,000 | $2,100 to $4,500 |
| Maintenance Frequency | Every 9 to 12 months | Annually |
| Best For | Mild laxity, labial rejuvenation, comfort | Vaginal atrophy, dryness, menopausal symptoms |
| FDA Cleared for Vaginal Use? | Off-label (cleared for general soft tissue) | Off-label (similar) |
| Evidence Base | Moderate (growing) | Stronger (more published studies) |
Both procedures are used off-label for vaginal rejuvenation, meaning the devices are FDA-cleared for general tissue heating and remodeling, but the specific application to vaginal tissue has not received a separate FDA indication. This is an important distinction that ethical providers should disclose during your consultation.
5. FemiLift: Another Laser Among Vaginal Rejuvenation Procedures Compared for Postpartum Recovery
FemiLift uses a pixel CO2 laser platform (the Alma Pixel CO2) to deliver controlled micro-ablative treatment to the vaginal walls. It’s often positioned as a competitor to MonaLisa Touch, and indeed, the mechanism of action is quite similar: create controlled micro-injuries, stimulate collagen production, restore tissue health.
How FemiLift Differs
While the underlying technology overlaps with MonaLisa Touch, FemiLift distinguishes itself in a few ways:
- The probe design allows for 360-degree treatment with a single insertion and rotation, potentially providing more uniform coverage.
- The treatment protocol is typically 3 sessions spaced 4 weeks apart, slightly faster than MonaLisa Touch’s 6-week intervals.
- FemiLift markets heavily toward postpartum women, positioning itself as a recovery tool for vaginal laxity, mild incontinence, and reduced sensation after childbirth, whereas MonaLisa Touch leans more into the menopausal demographic.
Cost Breakdown
FemiLift pricing is comparable to MonaLisa Touch:
- $800 to $1,500 per session
- 3 sessions required for initial treatment: $2,400 to $4,500
- Annual maintenance: 1 session per year, $800 to $1,500
What the Research Says
The evidence base for FemiLift is growing but still limited compared to MonaLisa Touch. Several small studies have shown improvements in:
- Vaginal tightness scores (patient-reported)
- Stress urinary incontinence symptoms
- Vaginal moisture and lubrication
- Sexual satisfaction scores
However, the studies are often manufacturer-funded, involve small sample sizes, and lack long-term follow-up beyond 12 months. This doesn’t mean FemiLift doesn’t work. It means we need more independent research to confirm the magnitude and durability of its effects.
Who Should Consider FemiLift?
FemiLift is worth exploring if you:
- Are in your postpartum recovery period (at least 3 months post-delivery)
- Experience mild vaginal laxity but don’t want or need surgery
- Have mild stress urinary incontinence
- Want a faster treatment protocol than MonaLisa Touch
- Live in an area where FemiLift is available but MonaLisa Touch is not (availability varies by region)
6. Votiva by InMode: Combination RF Vaginal Rejuvenation Procedures Compared for Versatility
Votiva is InMode’s entry into the vaginal rejuvenation market, and it brings something unique to the table: a combination approach. Votiva uses two complementary technologies, FormaV (bipolar radiofrequency for internal tightening) and FractoraV (fractional radiofrequency for external skin resurfacing), in a single treatment platform.
The Dual-Technology Advantage
FormaV delivers uniform, temperature-controlled radiofrequency energy to the internal vaginal canal. It heats the tissue to a therapeutic temperature that stimulates collagen production and tissue remodeling. The effect is gradual tightening and improved tissue tone over time.
FractoraV uses fractional radiofrequency to treat the external vulvar area, improving skin texture, reducing hyperpigmentation, tightening labial tissue, and addressing the aesthetic concerns that many women have about their external appearance.
By combining both modalities, Votiva allows providers to address internal laxity and external appearance in the same session. That’s a significant advantage when you compare vaginal rejuvenation procedures side by side, because most other nonsurgical options focus on either internal or external, not both.
Treatment Experience
A typical Votiva session:
- Takes 30 to 45 minutes
- Requires no anesthesia (topical numbing may be offered for FractoraV, which can cause mild discomfort)
- Involves minimal downtime (1 to 2 days of mild sensitivity)
- Is performed in an office setting
Cost Breakdown
- $1,500 to $3,500 per session (when combining FormaV and FractoraV)
- 3 sessions recommended initially: $4,500 to $10,500 total
- Annual maintenance: 1 to 2 sessions, $1,500 to $3,500 each
Ideal Candidates
Votiva is particularly well-suited for women who want:
- Both internal and external rejuvenation in one treatment
- Improved labial appearance without surgical labiaplasty
- Mild vaginal tightening
- Improvement in vulvar skin texture and discoloration
- A nonsurgical approach with minimal downtime
7. Platelet-Rich Plasma (PRP) Therapy: The O-Shot Among Vaginal Rejuvenation Procedures Compared
The O-Shot (short for “Orgasm Shot”) burst onto the scene with bold marketing claims about enhanced sexual pleasure, and it remains one of the more controversial entries when vaginal rejuvenation procedures are compared objectively. But controversy aside, the underlying science of PRP therapy is well-established in other areas of medicine, including orthopedics, dermatology, and wound healing.
What PRP Therapy Actually Is
PRP therapy involves:
- Drawing a small amount of your own blood (similar to a standard blood draw)
- Spinning the blood in a centrifuge to separate the platelet-rich plasma from other blood components
- Injecting the concentrated PRP into specific target areas
For the O-Shot specifically, the PRP is injected into:
- The clitoral area (to enhance sensitivity)
- The anterior vaginal wall (the area near the G-spot)
- Sometimes the labia and periurethral tissue
The growth factors in PRP stimulate tissue regeneration, increase blood flow, and promote new cell growth. The theory is that this rejuvenation leads to enhanced sensation, improved lubrication, easier arousal, and stronger orgasms.
What Does the Evidence Say?
Here’s where we need to be transparent. The evidence for the O-Shot specifically for sexual enhancement is still in its early stages. There are positive anecdotal reports and a handful of small studies, but no large, randomized, double-blind, placebo-controlled trials, which are the gold standard in medical research.
That said, PRP therapy’s regenerative properties are well-documented in other medical contexts. The question isn’t whether PRP regenerates tissue (it does). The question is whether injecting it into vaginal and clitoral tissue produces the specific sexual enhancement benefits that providers claim. The honest answer is: probably for some women, but we need better research to know for sure.
Cost
- $1,200 to $2,500 per injection
- 1 to 3 treatments recommended
- Total investment: $1,200 to $7,500
- Maintenance: Every 12 to 18 months
Who Might Benefit?
The O-Shot may be worth considering if you experience:
- Decreased sexual sensation or difficulty reaching orgasm
- Vaginal dryness that hasn’t responded well to other treatments
- Mild stress urinary incontinence
- Lichen sclerosus (early research suggests PRP may help with this condition)
Who Should Be Cautious?
Be wary of any provider who guarantees specific results from the O-Shot. The response is highly individual, and while many women report positive outcomes, others notice little difference. Also, ensure your provider is certified in the O-Shot procedure (there is a specific training protocol) and is using proper centrifuge equipment to prepare the PRP.
8. Pelvic Floor Physical Therapy: The Non-Procedure Vaginal Rejuvenation Approach Compared for Foundational Strength
Here’s where we take a sharp left turn from the world of lasers, radiofrequency, and surgery. Pelvic floor physical therapy (PFPT) isn’t technically a “procedure” in the medical sense, but when we compare vaginal rejuvenation procedures and approaches holistically, it absolutely deserves a seat at the table. In fact, many experts argue it should be the first line of treatment before any invasive or device-based option is considered.
Pelvic floor physical therapy involves working with a specialized physical therapist who assesses and treats the muscles, connective tissue, and nerves of the pelvic floor. These therapists have advanced training in women’s health and use a combination of techniques to restore function, strength, and coordination to the pelvic floor complex.
What Happens During Pelvic Floor PT
Your first appointment will typically include:
- A comprehensive history covering your symptoms, pregnancy and birth history, surgical history, exercise habits, bladder and bowel function, and sexual health.
- An external assessment of posture, breathing patterns, hip mobility, and core engagement.
- An internal assessment (with your consent) where the therapist evaluates pelvic floor muscle tone, strength, coordination, and any trigger points or areas of tension via vaginal palpation.
Based on this assessment, your therapist will develop a personalized treatment plan that may include:
- Kegel exercises (done correctly, not the way most women self-teach them)
- Biofeedback training using internal sensors that show you in real-time whether you’re engaging the right muscles
- Manual therapy to release tight or overactive pelvic floor muscles
- Electrical stimulation to help activate weak muscles
- Core and hip strengthening exercises
- Breathing and relaxation techniques
- Education on bladder and bowel habits
Why Pelvic Floor PT Should Come First
Here’s the thing most med-spas won’t tell you. According to the American College of Obstetricians and Gynecologists’ guidelines on pelvic floor disorders, pelvic floor muscle training is recommended as a first-line treatment for stress urinary incontinence and pelvic organ prolapse before considering surgical intervention.
The evidence supporting pelvic floor PT for these conditions is strong. Multiple systematic reviews have shown that supervised pelvic floor muscle training significantly reduces urinary incontinence, improves prolapse symptoms, and enhances sexual function.
And here’s a practical bonus: even if you ultimately decide to pursue a procedure like vaginoplasty or laser treatment, having a strong, well-functioning pelvic floor will improve your outcomes and recovery from those procedures. Pelvic floor PT and other vaginal rejuvenation procedures aren’t mutually exclusive. They’re complementary.
Cost
Pelvic floor PT is remarkably affordable compared to device-based treatments and surgery:
- $100 to $300 per session (varies by region and whether insurance is accepted)
- 8 to 12 sessions typical for a full treatment course
- Total investment: $800 to $3,600
Many insurance plans cover pelvic floor PT with a referral from your physician, potentially reducing your out-of-pocket cost to just a copay per visit. This makes it the most accessible option on this entire list.
The Catch
Pelvic floor PT requires active participation and consistency. You’ll need to do home exercises regularly, attend sessions weekly or biweekly, and commit to the process for several months. There’s no “lie back and let the machine do it” shortcut here. If you’re looking for a passive treatment, this isn’t it. But if you’re willing to put in the work, the results can be profound and lasting.
9. Emsella: The “Kegel Throne” Among Vaginal Rejuvenation Procedures Compared for Ease of Use
Imagine sitting on a chair, fully clothed, reading a magazine for 28 minutes, and walking out having completed 11,200 Kegel contractions. That’s Emsella, and yes, it sounds almost too good to be true.
Emsella uses High-Intensity Focused Electromagnetic (HIFEM) technology to stimulate deep pelvic floor muscle contractions without any voluntary effort on your part. The device looks like a futuristic chair, and you simply sit on it while electromagnetic waves cause your pelvic floor muscles to contract rapidly and intensely, far beyond what you could achieve through voluntary Kegel exercises.
How Emsella Works
The electromagnetic pulses penetrate the pelvic floor and trigger supramaximal contractions. A “supramaximal” contraction is one that is stronger than what you can voluntarily produce. These intense contractions effectively retrain and strengthen the pelvic floor muscles, improving their tone, endurance, and neuromuscular control.
The treatment protocol is straightforward:
- 6 sessions over approximately 3 weeks (2 sessions per week)
- Each session lasts 28 minutes
- You remain fully clothed throughout
- No downtime whatsoever
What Emsella Addresses
Emsella has received FDA clearance for the treatment of urinary incontinence. Studies have shown:
- 95% of patients reported improvement in quality of life
- 75% reduction in pad usage for urinary leakage
- Significant improvement in stress, urge, and mixed urinary incontinence
Beyond incontinence, many patients also report:
- Improved vaginal tightness and sensation
- Enhanced sexual satisfaction
- Greater confidence and freedom from worry about leakage
Cost Breakdown
- $250 to $500 per session
- 6 sessions in initial course: $1,500 to $3,000
- Maintenance: 1 to 2 sessions every 6 to 12 months, $250 to $500 each
- 5-year total: approximately $2,500 to $5,000
The Emsella Advantage
For women whose primary concern is urinary incontinence or pelvic floor weakness, Emsella offers an incredibly convenient option. No undressing. No probes. No pain. No downtime. You literally sit and let the machine work. It’s particularly appealing for women who:
- Haven’t been consistent with Kegel exercises (no judgment, most women haven’t)
- Are uncomfortable with internal examinations or treatments
- Want a non-invasive first step before considering more intensive procedures
- Are postpartum and looking for pelvic floor rehabilitation without internal devices
Limitations
Emsella does not address vaginal dryness, vaginal atrophy, or external cosmetic concerns. Its effects on vaginal tightness are secondary to muscle strengthening, not tissue remodeling. And while it’s fantastic for incontinence, it’s not a substitute for pelvic floor PT for women with complex pelvic floor dysfunction (such as pelvic pain syndromes or hypertonic, i.e., too-tight, pelvic floor muscles).
10. Perineoplasty: The Targeted Surgical Vaginal Rejuvenation Procedure Compared for Specific Repair
Perineoplasty is the quiet achiever of vaginal rejuvenation surgery. It doesn’t get the headlines that vaginoplasty or labiaplasty do, but for women whose primary concern is damage to the perineum (the area between the vaginal opening and the anus), it’s the most targeted and effective solution.
Why the Perineum Matters
The perineum is ground zero for childbirth trauma. It’s the tissue that stretches, tears, or is cut (episiotomy) during vaginal delivery. When the perineum heals poorly, or when it’s been damaged across multiple deliveries, the results can include:
- A widened or gaping vaginal opening that doesn’t close properly
- Reduced sensation during intercourse due to the loss of the normal “shelf” of perineal tissue
- A cosmetically unsatisfying appearance with irregular scarring
- Weakness in the posterior vaginal wall, contributing to rectocele (the rectum bulging into the vaginal canal)
- Wind trapping in the vagina during intercourse or exercise (yes, it’s a real and bothersome symptom, and no, you’re not the only one)
What Perineoplasty Involves
Perineoplasty is a relatively minor surgical procedure that:
- Removes scar tissue from previous tears or episiotomies
- Reconstructs and tightens the perineal body (the muscular wedge between vagina and anus)
- Tightens the vaginal opening specifically (without tightening the entire vaginal canal, which is what vaginoplasty does)
- Can be performed under local anesthesia with sedation in an outpatient setting
The procedure takes 30 to 60 minutes and is often combined with vaginoplasty or labiaplasty for a comprehensive result.
Cost
- $2,000 to $5,000 as a standalone procedure
- $1,000 to $2,000 additional when added to a vaginoplasty
- Often not covered by insurance unless performed as part of a medically necessary pelvic floor repair
Recovery
- 1 week off work recommended (desk jobs may allow earlier return)
- 4 to 6 weeks before resuming exercise and sexual activity
- Sutures dissolve on their own within 2 to 3 weeks
- Pain is generally mild to moderate, manageable with oral medication
Who Should Consider Perineoplasty?
This procedure is ideal if your primary issue is localized to the perineum and vaginal opening, rather than the deeper vaginal canal. If you had significant perineal tearing during delivery, a poorly healed episiotomy, or if the cosmetic and functional result of your perineum after childbirth is causing you distress, perineoplasty can be transformative.
11. Hyaluronic Acid Vaginal Injections: The Filler-Based Vaginal Rejuvenation Procedure Compared for Volume Restoration
If you’re familiar with dermal fillers for the face, this concept will feel intuitive. Hyaluronic acid (HA) vaginal injections apply the same principle to intimate anatomy: restoring lost volume, improving tissue hydration, and enhancing fullness in areas that have thinned or deflated with age.
How It Works
Hyaluronic acid is a naturally occurring substance in your body that holds moisture and provides structural volume. When injected into vaginal or vulvar tissue, it:
- Plumps thinning vaginal walls, restoring a more youthful tissue quality
- Hydrates the tissue at a deeper level than topical products can reach
- Enhances the G-spot area (when injected into the anterior vaginal wall, sometimes marketed as the “G-Shot”)
- Restores labial fullness in women who’ve experienced volume loss in the labia majora
The injections are performed in-office, take 15 to 30 minutes, and involve a fine needle or cannula to deliver the HA filler to specific target areas. Topical or local anesthetic is applied first to minimize discomfort.
What Conditions Does It Address?
- Vaginal dryness and atrophy that hasn’t responded to topical estrogen
- Loss of labial volume (deflated or flat-appearing labia majora)
- Desire for enhanced G-spot sensitivity
- Thinning of the vaginal vestibule causing pain with intercourse
Cost
- $1,000 to $2,500 per treatment
- Results last approximately 6 to 12 months before the HA naturally dissolves
- Repeat treatments necessary to maintain results
- 5-year total: $5,000 to $12,500
The Honest Take
Hyaluronic acid vaginal injections occupy an interesting middle ground. The science behind HA’s hydrating and volumizing properties is solid. The problem is that long-term data on its use specifically in vaginal tissue is still limited. We know it works as a temporary volumizer, but questions remain about:
- Long-term safety of repeated injections in this area
- Whether the hydrating effects are truly superior to consistent topical HA or estrogen therapy
- The evidence for G-spot enhancement (which is particularly thin and controversial)
If you pursue this option, work with a provider who has specific experience with intimate HA injections and uses products appropriate for this application.
12. Clitoral Hood Reduction: The Specialized Cosmetic Vaginal Rejuvenation Procedure Compared for Targeted Enhancement
Rounding out our comprehensive comparison is clitoral hood reduction (also called clitoral hoodectomy or clitoral unhooding), a specialized procedure that addresses the prepuce, the fold of skin covering the clitoris.
What It Is and Why Women Seek It
The clitoral hood serves a protective function, shielding the sensitive clitoral glans from constant friction. However, excess clitoral hood tissue can:
- Reduce sexual stimulation by creating too much tissue barrier between the clitoris and direct contact
- Cause aesthetic concerns, particularly when the excess tissue creates a visible bulge or irregularity
- Collect moisture and debris, potentially contributing to irritation or odor
- Create asymmetry with the surrounding labial tissue
Clitoral hood reduction removes the excess tissue while preserving enough of the hood to maintain its protective function. The procedure is delicate and requires a surgeon with specific expertise in female genital anatomy.
Surgical Technique
The procedure involves:
- Marking the excess tissue to be removed
- Administering local anesthesia
- Carefully excising the redundant hood tissue, typically from the sides (lateral approach) or the top (central approach)
- Closing the incisions with fine absorbable sutures
- Total procedure time: 30 to 45 minutes
Clitoral hood reduction is very commonly performed alongside labiaplasty, as excess hood tissue often accompanies excess labial tissue, and addressing both in a single procedure creates a more harmonious result.
Cost
- $1,500 to $3,500 as a standalone procedure
- $500 to $1,500 additional when combined with labiaplasty
- Not covered by insurance
Recovery
- Similar to labiaplasty: 1 to 2 weeks of swelling and sensitivity
- Sexual activity avoided for 4 to 6 weeks
- Final results visible at 3 to 6 months
Important Considerations
Clitoral hood reduction carries a unique risk profile because of the delicate structures involved. The clitoral nerve is the most densely innervated area in the human body, and damage to this nerve during surgery could result in permanent loss of sensation. This makes surgeon selection absolutely critical. Ask specifically about the surgeon’s experience with this particular procedure, not just labiaplasty or vaginoplasty in general.
The Complete $18,000 Investment Breakdown: All 12 Vaginal Rejuvenation Procedures Compared in One Table
Now let’s put it all together. Below is the comprehensive comparison table that brings all 12 procedures into a single, clear view. This is what your $18,000 (or less, or more) could look like depending on which procedures you choose.
| Procedure | Type | Primary Benefit | Cost Range (Initial) | Sessions Needed | Downtime | Pain Level | Maintenance | 5-Year Total Cost | Evidence Strength |
|---|---|---|---|---|---|---|---|---|---|
| Vaginoplasty | Surgical | Structural vaginal tightening | $5,000 – $12,000 | 1 | 6 – 8 weeks | Moderate to high | None (permanent) | $5,000 – $12,000 | Strong |
| Labiaplasty | Surgical | Labial reshaping/reduction | $3,000 – $8,000 | 1 | 4 – 6 weeks | Moderate | None (permanent) | $3,000 – $8,000 | Strong |
| MonaLisa Touch | Laser (CO2) | Vaginal atrophy/dryness | $2,100 – $4,500 | 3 | 2 – 3 days | Minimal | Annual | $5,600 – $10,500 | Moderate to strong |
| ThermiVa | Radiofrequency | Mild tightening, comfort | $4,500 – $9,000 | 3 | None | None | Every 9 – 12 months | $10,500 – $21,000 | Moderate |
| FemiLift | Laser (CO2) | Postpartum recovery, laxity | $2,400 – $4,500 | 3 | 1 – 2 days | Minimal | Annual | $5,600 – $10,500 | Moderate |
| Votiva (InMode) | RF (dual) | Internal + external rejuvenation | $4,500 – $10,500 | 3 | 1 – 2 days | Minimal | Annual | $7,500 – $17,500 | Moderate |
| O-Shot (PRP) | Injectable | Sexual enhancement, sensitivity | $1,200 – $7,500 | 1 – 3 | None | Mild | Every 12 – 18 months | $3,600 – $15,000 | Weak to moderate |
| Pelvic Floor PT | Therapy | Strength, incontinence, function | $800 – $3,600 | 8 – 12 | None | None | Ongoing home exercises | $800 – $5,000 | Strong |
| Emsella | Electromagnetic | Incontinence, pelvic floor strength | $1,500 – $3,000 | 6 | None | None to mild | Every 6 – 12 months | $2,500 – $5,000 | Moderate to strong |
| Perineoplasty | Surgical | Perineal repair/tightening | $2,000 – $5,000 | 1 | 4 – 6 weeks | Moderate | None (permanent) | $2,000 – $5,000 | Strong |
| HA Injections | Injectable | Volume restoration, hydration | $1,000 – $2,500 | 1 | None | Mild | Every 6 – 12 months | $5,000 – $12,500 | Weak to moderate |
| Clitoral Hood Reduction | Surgical | Enhanced sensation, aesthetics | $1,500 – $3,500 | 1 | 2 – 4 weeks | Mild to moderate | None (permanent) | $1,500 – $3,500 | Moderate |
How to Read This Table
A few key takeaways from looking at all vaginal rejuvenation procedures compared side by side:
Surgical procedures cost more upfront but don’t require maintenance. Vaginoplasty, labiaplasty, perineoplasty, and clitoral hood reduction are one-time investments. What you pay is what you pay, and the results are permanent (barring future pregnancies or significant weight changes).
Nonsurgical procedures cost less initially but add up over time. ThermiVa, for example, looks attractive at $4,500 to $9,000 for the initial series, but over 5 years with maintenance, you could easily spend $10,500 to $21,000. That potentially exceeds the cost of surgical vaginoplasty, which delivers more dramatic and permanent results.
Evidence strength varies significantly. Pelvic floor PT, vaginoplasty, and labiaplasty have the most robust evidence supporting their effectiveness. Newer technologies like ThermiVa, Votiva, and the O-Shot have promising results but need larger, longer-term, independently funded studies.
There is no single “best” procedure. The right choice depends entirely on your specific concerns, anatomy, budget, risk tolerance, and lifestyle. A postmenopausal woman struggling with vaginal dryness has completely different needs than a 35-year-old postpartum woman dealing with laxity and incontinence.
How to Choose the Right Vaginal Rejuvenation Procedure: A Decision Framework
With 12 vaginal rejuvenation procedures compared, making a decision can feel overwhelming. Here’s a practical framework to help you narrow down your options.
Step 1: Identify Your Primary Concern
Be honest with yourself about what’s really driving your interest. Is it:
- Urinary incontinence? Start with pelvic floor PT and/or Emsella. If those don’t deliver sufficient results, consider surgical options.
- Vaginal dryness and atrophy? MonaLisa Touch or FemiLift are strong contenders. Also discuss topical estrogen therapy with your doctor.
- Vaginal laxity (looseness)? Mild cases may respond to ThermiVa, Votiva, or Emsella. Moderate to severe laxity usually needs vaginoplasty.
- External appearance? Labiaplasty, clitoral hood reduction, or Votiva’s FractoraV component.
- Sexual sensation? The O-Shot, pelvic floor PT, or surgical options depending on the underlying cause.
- Perineal damage from childbirth? Perineoplasty, potentially combined with vaginoplasty.
Step 2: Assess Your Budget and Timeline
Be realistic about what you can afford, both now and for maintenance. A $2,000 procedure that requires $1,500 annual maintenance is more expensive over 5 years than a $5,000 one-time surgical procedure. Do the math for your specific situation.
Also consider how much downtime you can realistically take. If you’re a single parent with no childcare support, 6 weeks of restricted activity post-vaginoplasty may not be feasible right now. That doesn’t mean you should rule it out permanently. It means the timing may need to wait.
Step 3: Evaluate the Evidence
Not all that glitters is gold, especially in the aesthetics and wellness industry. Before committing to any procedure, ask your provider:
- What peer-reviewed studies support this treatment for my specific concern?
- What are the expected results based on clinical data, not testimonials?
- What percentage of your patients are satisfied with their results?
- What are the risks, and how do they compare to the expected benefits?
- Is this device FDA-cleared for vaginal use, or is it being used off-label?
Step 4: Choose Your Provider Carefully
This may be the most important step of all. The skill and experience of your provider matters more than the specific technology or technique they use. A masterful surgeon with a basic technique will outperform a mediocre surgeon with the latest technology every time.
For surgical procedures, look for:
- Board certification in gynecology, urogynecology, or plastic surgery
- Specific fellowship or training in female pelvic medicine or genital cosmetic surgery
- A high volume of the specific procedure you’re considering
- Before-and-after photos (many providers keep a portfolio for consultation)
- Patient testimonials and reviews
- Willingness to discuss risks honestly, not just benefits
For nonsurgical procedures, verify that:
- The provider has been properly trained on the specific device being used
- The device is authentic and well-maintained (ask about device age and calibration)
- The clinic follows proper infection control protocols
- The provider performs a thorough consultation before recommending treatment
- There’s no high-pressure sales environment (a major red flag)
Understanding the Risks: What Every Woman Should Know Before Any Vaginal Rejuvenation Procedure
No discussion of vaginal rejuvenation procedures compared would be complete without a frank conversation about risks. Every treatment on this list, from the most conservative to the most invasive, carries some degree of risk.
Universal Risks Across All Procedures
- Infection: Any time the skin or mucosal barrier is broken, there’s an infection risk. Proper sterile technique minimizes but never eliminates this risk.
- Unsatisfactory results: No procedure guarantees a specific outcome. Individual healing, anatomy, and tissue quality all influence results.
- Financial risk: These procedures are expensive, and results aren’t guaranteed. There are no refunds in medicine.
- Psychological risk: If your expectations are unrealistic, even an objectively excellent result may leave you feeling disappointed.
Specific Risks by Category
Surgical procedures (vaginoplasty, labiaplasty, perineoplasty, clitoral hood reduction):
- Bleeding, hematoma, or seroma
- Scarring (sometimes thick or painful)
- Wound separation
- Over-correction or under-correction
- Permanent changes in sensation
- Need for revision surgery (approximately 5% to 10% of cases)
- Anesthesia-related complications
Laser and RF procedures (MonaLisa Touch, FemiLift, ThermiVa, Votiva):
- Burns (rare with proper technique)
- Vaginal discharge or spotting after treatment
- Temporary increase in sensitivity
- Lack of expected improvement
- Rare cases of scarring or fibrosis
Injectable procedures (O-Shot, HA injections):
- Bruising at injection sites
- Temporary swelling
- Uneven distribution of product
- Migration of filler material
- Allergic reaction (rare)
- No improvement (possible with any treatment)
The FDA’s Position
In July 2018, the FDA issued a safety communication warning about the use of energy-based devices for vaginal rejuvenation, including laser and radiofrequency treatments. The FDA stated that these devices had not been cleared or approved for vaginal cosmetic procedures and that their safety and effectiveness for these uses had not been established.
This doesn’t mean these treatments are dangerous or ineffective. It means the specific application of these devices to vaginal tissue hasn’t gone through the FDA’s formal approval process for that indication. The devices themselves are FDA-cleared for general tissue ablation and coagulation. It’s the marketing of them specifically for vaginal rejuvenation that the FDA took issue with.
Understanding this distinction helps you make an informed decision. Off-label use of medical devices and medications is extremely common in medicine and is not inherently problematic, but you should be aware of it.
Combining Procedures: How Women Are Stacking Vaginal Rejuvenation Treatments for Maximum Results
One of the most significant trends in vaginal rejuvenation is the combination approach, where women strategically stack multiple procedures to address different concerns simultaneously or sequentially.
Popular Combinations
The “Mommy Makeover” Package:
- Vaginoplasty + labiaplasty + perineoplasty
- Total cost: $8,000 to $20,000
- Performed in a single surgical session
- One recovery period instead of three
- Addresses internal laxity, external appearance, and perineal damage all at once
The Nonsurgical Triple:
- ThermiVa or Votiva (tissue tightening) + O-Shot (enhanced sensation) + Emsella (pelvic floor strengthening)
- Total cost: $7,200 to $19,500 for initial courses
- No surgical downtime
- Addresses multiple concerns through different mechanisms
- Can be staggered over several months
The Foundational Approach:
- Pelvic floor PT (8 to 12 sessions) followed by Emsella (6 sessions) followed by MonaLisa Touch (3 sessions)
- Total cost: $4,400 to $11,100
- Builds from foundational muscle strength upward to tissue quality
- Evidence-supported at each step
- Allows you to assess results incrementally before committing to additional treatments
The Surgical-Plus Approach:
- Vaginoplasty + post-operative pelvic floor PT + MonaLisa Touch maintenance
- Total cost: $7,800 to $18,100 over 5 years
- Surgical correction of structural laxity, therapeutic rehabilitation of the pelvic floor, and ongoing tissue quality maintenance
- Arguably the most comprehensive approach available
When Combining Makes Sense
Combining vaginal rejuvenation procedures makes sense when:
- You have multiple distinct concerns that a single procedure can’t address
- You want both structural correction (surgery) and tissue quality improvement (laser/RF)
- You’re starting with conservative options and planning to escalate if needed
- You have the budget to invest in a comprehensive treatment plan
When Combining Doesn’t Make Sense
- When you’re doing it because a clinic pressured you into a package deal
- When you haven’t fully recovered from one procedure before starting another
- When you haven’t given a single treatment adequate time to show results (many women add treatments too quickly out of impatience)
- When the combination offers redundant mechanisms (e.g., combining MonaLisa Touch and FemiLift, which use essentially the same technology)
What Insurance Covers (And What It Absolutely Doesn’t)
Let’s talk money with complete transparency, because the financial aspect of vaginal rejuvenation is where many women get blindsided.
Generally Not Covered by Insurance
All cosmetic vaginal rejuvenation procedures, including:
- Labiaplasty for aesthetic purposes
- Vaginoplasty for vaginal tightening (when no medical condition is present)
- ThermiVa, Votiva, and other RF/laser treatments
- O-Shot and PRP therapy
- HA injections
- Clitoral hood reduction
- Emsella (though this is changing as evidence grows)
Potentially Covered by Insurance
- Pelvic floor physical therapy with a physician referral for documented incontinence or pelvic floor dysfunction
- Vaginoplasty when performed for pelvic organ prolapse repair (classified as a colporrhaphy, not cosmetic vaginoplasty)
- Labiaplasty when excess tissue is causing documented medical problems (recurrent infections, significant pain, functional impairment)
- Perineoplasty when performed as part of a pelvic floor reconstruction for medical reasons
How to Maximize Insurance Coverage
If your concern is medically based (not purely cosmetic), take these steps:
- Document your symptoms meticulously. Keep a bladder diary if you have incontinence. Record the frequency and severity of pain. Note any activities you avoid because of your symptoms.
- Get a formal diagnosis from a physician. A diagnosis of stress urinary incontinence, pelvic organ prolapse, or vulvar pain disorder carries more weight with insurers than vague complaints.
- Pursue conservative treatment first. Most insurers require documentation that you’ve tried and failed conservative treatments (like pelvic floor PT) before they’ll consider covering surgical options.
- Obtain pre-authorization before scheduling any procedure. Don’t assume coverage. Get it in writing.
- Work with your surgeon’s billing department. Experienced billing staff know how to code procedures correctly to maximize the chance of coverage.
Real Talk: The Emotional Side of Vaginal Rejuvenation That Nobody Discusses
We’ve spent thousands of words on procedures, costs, technologies, and evidence. But let’s pause and talk about something just as important: the emotional journey.
Deciding to pursue vaginal rejuvenation is rarely purely clinical. It’s wrapped up in feelings about aging, motherhood, sexuality, body image, relationships, and identity. And those feelings deserve acknowledgment.
The Shame Factor
Many women feel embarrassed about even wanting vaginal rejuvenation. There’s a persistent cultural narrative that wanting to change your body, especially your intimate anatomy, means something is wrong with you psychologically. That you’re not “accepting yourself as you are.” That you’re doing it “for a man.”
Let’s put that narrative to rest. Women pursue vaginal rejuvenation for themselves. For their comfort. For their confidence. For their health. For their pleasure. The same way someone might get a knee replacement to walk without pain, or corrective eye surgery to see without glasses. Improving function and quality of life is not vanity. Full stop.
The Expectation Trap
On the other end of the emotional spectrum is the expectation trap. Some women approach vaginal rejuvenation expecting it to fix their relationship, transform their sex life, or restore them to their 20-year-old body. While these procedures can certainly improve things, they’re not magic wands.
If your relationship has deeper issues, vaginal tightening won’t fix them. If your low libido is driven by stress, depression, or hormonal imbalance, a laser treatment alone won’t be the answer. And no procedure in the world will make you 25 again. Setting realistic expectations is not pessimism. It’s wisdom.
The Partner Conversation
Many women struggle with whether and how to discuss vaginal rejuvenation with their partner. There’s no single right answer here. Some women involve their partners early in the decision-making process. Others make the decision independently and inform their partner afterward. Some choose not to discuss it at all.
What matters is that the decision is yours. If you choose to involve your partner, approach the conversation from a place of empowerment, not apology. You’re not “fixing” yourself for them. You’re investing in your own wellbeing, and they happen to benefit too.
When to Seek Psychological Support
If your desire for vaginal rejuvenation is accompanied by:
- Persistent negative thoughts about your body that interfere with daily life
- Avoidance of intimacy due to shame or anxiety about your anatomy
- Body dysmorphic tendencies (obsessive focus on perceived flaws that others don’t notice)
- Pressure from a partner who is making you feel inadequate
Then it’s worth speaking with a therapist who specializes in body image or sexual health before pursuing any procedure. This isn’t about gatekeeping. It’s about ensuring that the procedure serves your genuine needs and that you’re in the best emotional place to make a clear-headed decision.
The Future of Vaginal Rejuvenation: What’s Coming in 2025 and Beyond
The field of vaginal rejuvenation is evolving rapidly. Here’s what’s on the horizon:
Regenerative Medicine Approaches
Stem cell therapy for vaginal rejuvenation is currently in early clinical trials. The concept involves injecting autologous stem cells (harvested from your own fat tissue) into the vaginal walls to promote tissue regeneration. Early results are promising, but we’re likely 3 to 5 years away from mainstream availability.
Improved Energy-Based Devices
The next generation of laser and RF devices is being designed specifically for vaginal application from the ground up, rather than repurposing devices originally designed for other body areas. These purpose-built devices should deliver more consistent results and may eventually obtain direct FDA clearance for vaginal rejuvenation.
Combination Devices
Devices that combine multiple energy modalities (laser + RF + ultrasound) in a single treatment session are in development. These could reduce the number of sessions needed and improve outcomes by targeting tissue through complementary mechanisms.
Better Evidence
Perhaps most importantly, larger and better-designed clinical trials are underway for many of the procedures discussed in this article. Within the next few years, we should have much clearer data on the long-term safety and effectiveness of laser and RF vaginal rejuvenation, which will help both patients and providers make more informed decisions.
Telemedicine Integration
Some aspects of pelvic floor rehabilitation are moving to telemedicine-supported models, where patients work with a pelvic floor PT in person initially and then transition to supervised home programs using biofeedback devices connected to smartphone apps. This could dramatically improve accessibility and reduce costs.
Frequently Asked Questions About Vaginal Rejuvenation Procedures Compared
How do I know if I actually need vaginal rejuvenation?
“Need” is a strong word. If you’re experiencing functional problems like urinary incontinence, pelvic organ prolapse, pain during intercourse, or significant quality-of-life impacts from vaginal laxity or dryness, then treatment can genuinely improve your life. If your concerns are primarily cosmetic, the decision is personal. There’s no universal standard for how vulvas or vaginas “should” look or feel. The question is whether the issue bothers you enough to justify the investment and risk.
Can I get vaginal rejuvenation if I plan to have more children?
Technically, yes. But practically, most surgeons recommend waiting until you’ve completed your family before pursuing surgical vaginal rejuvenation. A subsequent vaginal delivery would likely undo much of the surgical correction, meaning you’d need a repeat procedure. Nonsurgical treatments like ThermiVa, Emsella, or pelvic floor PT are better options if you plan to have more children, as they can be repeated and don’t involve surgical results that a future delivery might compromise.
Are results permanent?
It depends on the procedure. Surgical results are permanent in the sense that the tissue changes don’t reverse themselves. However, aging, weight fluctuations, hormonal changes, and gravity continue to affect tissues over time, so results may gradually shift. Nonsurgical treatments are inherently temporary, requiring ongoing maintenance to sustain results.
What’s the youngest/oldest age for vaginal rejuvenation?
Most providers require patients to be at least 18 for cosmetic procedures. There’s no upper age limit, and many women in their 60s and 70s pursue nonsurgical treatments for vaginal atrophy with excellent results. For surgical procedures, overall health and ability to tolerate anesthesia are more important than chronological age.
Can vaginal rejuvenation improve my sex life?
It can, but with important caveats. Procedures that tighten the vaginal canal can increase friction and sensation during intercourse for both partners. Treatments that improve lubrication and tissue quality can make intercourse more comfortable. Pelvic floor strengthening can enhance orgasm intensity. But sexual satisfaction is multifactorial, involving psychological, relational, hormonal, and physical components. A procedure can address the physical component, but if the other factors are contributing to dissatisfaction, they need attention too.
How do I find a qualified provider?
For surgical procedures, start with the American Board of Obstetrics and Gynecology (ABOG) or the American Board of Plastic Surgery (ABPS) to verify board certification. For nonsurgical treatments, look for providers who have completed manufacturer-specific training for the device they’re using and who have significant experience with vaginal rejuvenation patients specifically. Don’t hesitate to ask about their training, volume of procedures, and complication rates.
A Note on Terminology and Inclusivity
Throughout this article, I’ve used terms like “women” and “female anatomy” for clarity and readability. However, it’s important to acknowledge that not all people with vaginas identify as women, and not all women have vaginas. Vaginal rejuvenation may be relevant to transgender men, nonbinary individuals, and others who experience the conditions discussed here. If you’re a member of the LGBTQ+ community seeking these treatments, look for providers who create inclusive, affirming clinical environments.
Conclusion: Your Body, Your Decision, Your Timeline
If you’ve made it through all 12 vaginal rejuvenation procedures compared in this guide, you now know more about this topic than 95% of the general public, and honestly, more than some general practitioners. That knowledge is your greatest asset moving forward.
Here’s what I want you to take away from this. There is no single “best” vaginal rejuvenation procedure. There is only the best procedure for you, right now, given your specific anatomy, symptoms, goals, budget, and life circumstances. What’s right for your best friend, your sister, or the woman who posted her transformation on social media may not be right for you.
Start with the foundation. Pelvic floor physical therapy is underrated, evidence-based, affordable, and accessible. It should be your first step, regardless of what else you’re considering. From there, you can layer additional treatments as needed.
If your concerns are primarily about tissue quality, dryness, and atrophy, the laser and RF options offer real improvements with minimal downtime. If your concerns are structural, involving significant laxity or perineal damage, surgical options deliver the most definitive results.
And if you’re still unsure? That’s completely fine. Take this article to your next gynecologist appointment. Show them the comparison table. Have a conversation grounded in evidence, not marketing. Ask the hard questions. Get a second opinion if the first one doesn’t feel right.
This is your body. Your investment. Your quality of life. There’s no rush, and there’s no wrong choice, as long as it’s an informed one.
Share This With Someone Who Needs It
If this article helped you understand vaginal rejuvenation procedures more clearly, please share it with a friend, sister, mother, or anyone who might be quietly struggling with the same questions. Too many women suffer in silence because they don’t know their options exist. Let’s change that, one shared article at a time.
Have questions this article didn’t answer? Drop them in the comments below. I read every single one and will respond with evidence-based answers.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider before making decisions about medical procedures. Individual results vary, and no procedure guarantees specific outcomes. All cost figures are approximate and vary by geographic location, provider, and individual treatment plans.