You already know that drinking too much is “not great” for your health. But nobody told you it could be quietly raising your breast cancer risk with every single glass.
That glass of Pinot Grigio with dinner. The prosecco at the birthday party. The “I deserve this” cocktail after a brutal work week. Millions of women pour these moments without a second thought, completely unaware that alcohol is one of the most well-documented, modifiable risk factors for breast cancer in the world.
This is not a scare piece. This is information that your doctor may not have spelled out for you at your last checkup, that wine advertising will never mention, and that most women simply do not have access to in plain language. The science is staggering, the statistics are sobering, and you deserve to know all of it.
Breast cancer remains the most commonly diagnosed cancer among women worldwide. In the United States alone, roughly 1 in 8 women will receive a breast cancer diagnosis at some point in their lifetime. While some risk factors, like your age or your genetics, are completely out of your control, alcohol consumption is different. It is a lever you can actually pull. And the research is increasingly clear that pulling it in the right direction can make a meaningful difference to your long-term health.
Let us walk through the seven statistics that every woman should have memorized, the biology behind why alcohol does what it does to breast tissue, and what practical steps you can take right now.
Statistic #1: Even Light Drinking Raises Your Breast Cancer Risk — The Alcohol and Breast Cancer Dose-Response Is Linear
Let us start with the one that tends to knock the wind out of people.
A landmark 2024 meta-analysis of prospective cohort studies published in Alcohol, Clinical and Experimental Research confirmed what researchers have suspected for decades: there is no safe lower threshold for alcohol when it comes to breast cancer. The relationship is linear. The more you drink, the higher the risk. And it begins before you even hit one full drink per day.
The numbers are specific and stark. Compared to women who drink no alcohol, the relative risk of breast cancer is 1.05 for just half a drink per day, 1.10 for one drink per day, 1.18 for two drinks per day, and 1.22 for three drinks per day. Even consuming less than one standard drink daily was found to significantly increase breast cancer risk.
What this means in plain language: there is no amount of alcohol that research has identified as completely safe for breast health. The World Health Organization has stated it directly, that “no level of alcohol consumption is safe when it comes to human health,” and the breast cancer data backs this up with consistent, reproducible evidence across dozens of studies in multiple countries.
Key takeaways:
- Risk increases with every additional drink consumed regularly.
- The dose-response relationship is linear, meaning no flat “safe zone” exists below a certain threshold.
- Even occasional or light drinkers carry a measurably elevated risk compared to non-drinkers.
Statistic #2: One Drink a Day Is Linked to a 10% Higher Breast Cancer Risk — What the 2025 Dietary Guidelines Reveal About Alcohol
You may have heard that one drink a day is the official guideline for women. Technically, it has been the accepted “moderate” level for years. But the 2025-2030 U.S. Dietary Guidelines, released in January 2026, fundamentally changed the tone of that conversation.
The National Academies of Sciences, Engineering, and Medicine (NASEM) report that supported the new guidelines found that drinking one drink per day or fewer in women was still associated with a 10% increased breast cancer risk. The guidelines moved decisively away from the old “moderation” framing and toward a clear, unambiguous directive: drink less.
This is not a small revision. The previous guidelines had used the word “moderation” in a way that many people interpreted as permission. The updated version makes the health tradeoff explicit, and breast cancer is front and center in that conversation.
Additionally, the 2025 U.S. Surgeon General’s Advisory, issued in January 2025 by Dr. Vivek Murthy, called for updated cancer-warning labels on all alcoholic beverage containers. This was the first proposed update to alcohol warning labels in nearly four decades. The Surgeon General specifically named breast cancer as one of at least seven cancer types linked to alcohol consumption.
Key takeaways:
- Even “moderate” drinking within official guidelines carries a 10% higher breast cancer risk.
- The 2025-2030 Dietary Guidelines moved away from “moderation” toward “drink less.”
- A Surgeon General’s advisory called for cancer warnings on alcohol labels specifically citing breast cancer.
Statistic #3: Moderate Drinking Can Increase Breast Cancer Risk by 30 to 50% — The Numbers Behind “Social Drinking” and Cancer
Here is where the numbers get genuinely jarring.
Multiple case-control and cohort studies, including a widely cited review from Columbia University’s Mailman School of Public Health, have documented that moderate alcohol consumption, defined roughly as 1 to 2 drinks per day or 15 to 30 grams of alcohol daily, is associated with an approximate 30 to 50% increased risk of breast cancer compared to non-drinkers.
Thirty to fifty percent. Not a rounding error. Not a tiny statistical blip. A substantial elevation in risk from a level of drinking that most people would describe as perfectly normal social behavior.
A separate analysis of 20 studies found that regular alcohol consumption raised the risk of estrogen receptor-positive (ER+) breast cancer by 35% and estrogen receptor-negative (ER-) breast cancer by 28%. Hormone receptor-positive breast cancers are the most common type, making the 35% figure especially relevant for the vast majority of women.
The Women’s Health Study, a prospective cohort study tracking nearly 40,000 women over a median of 25 years, found that compared to women who rarely or never drank, consuming alcohol at least monthly was associated with 63.79 more breast cancer cases per 100,000 women over 10 years. Consuming more than one drink per day was associated with 278.66 additional cases per 100,000 women. These are real women, real cases, and real statistics that underline the population-level burden alcohol places on breast health.
Key takeaways:
- Moderate drinking is linked to a 30 to 50% increased breast cancer risk in multiple large studies.
- The elevated risk applies to both pre- and postmenopausal women.
- Hormone receptor-positive breast cancers, the most common subtype, show the strongest alcohol-related risk increase.
Statistic #4: Alcohol Is a Group 1 Carcinogen — And Most Women Have No Idea
Here is a fact that should be on the label of every bottle of wine, beer, and spirits on the shelf: the World Health Organization’s International Agency for Research on Cancer (IARC) classifies alcohol as a Group 1 carcinogen. That is the same category as tobacco smoke, asbestos, and processed meats.
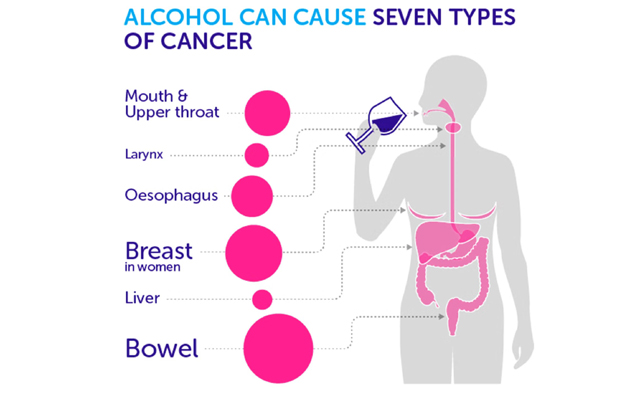
Group 1 means the evidence for causing cancer in humans is conclusive. It is the highest-risk classification available. Alcohol earned this designation not for one cancer type but for at least seven, including breast, colorectal, liver, esophageal, stomach, and certain head and neck cancers.
Despite this, public awareness remains shockingly low. According to the AACR Cancer Progress Report 2024, fewer than half of Americans are even aware that alcohol can increase cancer risk at all. A January 2025 Annenberg Public Policy Center survey found that only 56% of U.S. adults knew that regular alcohol consumption raises cancer risk, up from just 40% four months earlier, largely because of the Surgeon General’s advisory receiving major media coverage.
The information gap is staggering. A substance classified in the same carcinogen tier as cigarettes has been culturally normalized, socially celebrated, and aggressively marketed, particularly to women, while the public remains largely unaware of its cancer connection.
According to the AACR, approximately 5.4% of all cancers diagnosed in the United States are attributable to alcohol consumption. Reducing or stopping alcohol consumption altogether can lower the risk of developing alcohol-related cancers by 8%.
Key takeaways:
- Alcohol is officially classified as a Group 1 carcinogen by the WHO’s IARC.
- Fewer than half of Americans knew alcohol raises cancer risk before the 2025 Surgeon General’s advisory.
- 5.4% of all U.S. cancer diagnoses are attributable to alcohol, according to the AACR.
Statistic #5: Binge Drinking Carries a Unique and Compounding Risk — Not Just a “One-Night Thing”
You might be thinking, “I don’t drink every day. I just have a lot on the weekend.” That pattern, often called heavy episodic drinking or binge drinking, carries its own specific and compounding risk that deserves its own spotlight.
Research included in the 2024 systematic review in Alcohol, Clinical and Experimental Research found that heavy episodic drinking (HED) is positively associated with breast cancer risk, and the pattern of drinking may matter beyond just the total volume consumed. When large amounts of alcohol are consumed in a short window, the enzymatic pathways responsible for breaking down ethanol and its toxic byproduct acetaldehyde can become saturated. The result is a prolonged surge of acetaldehyde in the bloodstream, a carcinogen that directly damages DNA and prevents the body from repairing it properly.
Binge drinking also triggers additional biological cascade effects that are each known cancer-promotion pathways: increased oxidative stress, systemic inflammation, and insulin resistance. These mechanisms do not “reset” after a single night out. Over time and with repeated episodes, they accumulate in their effect on cellular health.
A 2024 Harvard Women’s Health Study analysis found that even drinking exceeding one drink per month was associated with measurable breast cancer risk elevation. Approximately 4.1% of breast cancer cases in their cohort were attributable to consumption exceeding just one drink per month, which places even infrequent drinkers in a statistically meaningful risk category.
Key takeaways:
- Binge drinking saturates the body’s alcohol-processing pathways, leading to elevated acetaldehyde exposure.
- Heavy episodic drinking compounds cancer risk through inflammation, oxidative stress, and insulin resistance.
- The pattern of drinking matters alongside the total volume consumed.
Statistic #6: Alcohol Raises Estrogen Levels — And That Hormonal Shift Fuels Breast Cancer Growth
This is the biological mechanism that ties so much of the alcohol-breast cancer research together, and it is worth understanding clearly, because it explains why the risk is not random or mysterious. It is mechanistic, predictable, and rooted in how your body processes alcohol at a hormonal level.
When you drink alcohol, your body converts it to a toxic chemical called acetaldehyde. But that is only part of the story. Alcohol also drives up the levels of circulating estrogen in your body. It does this by enhancing the activity of an enzyme called aromatase, which converts androgens into estrogens, particularly in fat tissue. Higher estrogen levels in the bloodstream directly stimulate the growth of estrogen receptor-positive (ER+) breast cells, which are the cells most likely to become cancerous.
In a controlled feeding study of 51 postmenopausal women, consuming 15 to 30 grams of alcohol per day for 8 weeks increased concentrations of estrone sulfate by up to 10.7% and dehydroepiandrosterone (DHEAS) by up to 7.5% compared to a placebo. Among premenopausal women, moderate alcohol intake also increases exposure to endogenous estrogens by altering menstrual cycle patterns.
Alcohol also appears to downregulate BRCA1, the tumor suppressor gene most people associate with hereditary breast cancer risk. In laboratory studies, ethanol has been shown to suppress BRCA1 expression, which in turn increases the transcriptional activity of estrogen receptors and creates greater opportunity for genetic damage to accumulate in breast cells.
This is the chain of events that happens inside your body when you drink. It is not theoretical. It has been replicated in controlled studies, in cell cultures, and in large epidemiological cohorts. According to the Breast Cancer Research Foundation, alcohol is broken down into acetaldehyde, which damages DNA and prevents the body from repairing it, and once DNA is damaged, a cell can start to grow out of control and form a malignant tumor.
Key takeaways:
- Alcohol raises circulating estrogen by enhancing aromatase enzyme activity.
- Higher estrogen levels stimulate the growth of ER+ breast cancer cells.
- Alcohol also suppresses BRCA1, the key tumor suppressor gene in breast tissue.
- Acetaldehyde damages DNA and blocks the body’s natural repair mechanisms.
Statistic #7: Women on Hormone Replacement Therapy Face a Tripled Risk When They Combine HRT With Alcohol
This statistic is particularly critical for women over 40 who are navigating menopause.
Research has found that postmenopausal women who were taking hormone replacement therapy (HRT) and consuming one to two alcoholic drinks per day had a breast cancer risk that was three times higher than women who neither drank nor used HRT. That is a 3-fold increase in risk from combining two factors, each of which independently raises breast cancer risk.
The mechanism is not difficult to understand once you grasp the estrogen story from Statistic #6. HRT introduces or mimics hormones in the body, while alcohol independently boosts circulating estrogen levels. When combined, these two estrogen-elevating inputs create a compounding hormonal environment that is significantly more favorable to breast cancer cell proliferation than either factor alone.
This does not mean every woman on HRT should panic. The decision about HRT involves many factors, including quality of life during menopause, bone density, cardiovascular considerations, and personal and family health history. But if you are currently on HRT, or considering it, the alcohol piece of this picture deserves an honest conversation with your doctor. Many women simply do not know to raise it.
Key takeaways:
- Combining HRT with 1 to 2 drinks per day can triple breast cancer risk compared to abstaining from both.
- The compounding effect is driven by both HRT and alcohol independently raising estrogen levels.
- Women currently on HRT should discuss their alcohol intake with their healthcare provider.
The Science Behind the Statistics: Why Alcohol Is Not “Just Calories”
Understanding the seven statistics above is one thing. Understanding why they are true makes it far easier to take them seriously and act on them. Let us break down the core biological mechanisms, because this is where the story becomes less about numbers and more about what is actually happening inside your body every time you drink.
The Acetaldehyde Problem
When your liver processes ethanol, the first major metabolite it produces is acetaldehyde. This compound is classified as a probable carcinogen in its own right. It forms what are called DNA adducts, essentially attaching itself to your DNA in ways that cause mutations and block the repair enzymes that would normally fix them. Over time, these accumulated mutations can tip a normal breast cell into a cancerous one.
The body is reasonably efficient at clearing acetaldehyde under normal conditions. But during heavy or binge drinking episodes, the processing pathways become overwhelmed, and acetaldehyde concentrations remain elevated in the bloodstream for longer. Genetically, some women also carry variations in alcohol-metabolizing genes that result in higher baseline acetaldehyde levels even from small amounts of alcohol, making them biologically more vulnerable to alcohol’s carcinogenic effects.
The Estrogen Amplification Loop
Alcohol does not just damage DNA directly. It also creates a hormonal environment that is favorable to cancer growth. By increasing aromatase activity and raising circulating estrogen levels, alcohol essentially turns up the volume on a signal that ER+ breast cells are already tuned to receive. This is why the alcohol-breast cancer association is particularly strong for estrogen receptor-positive tumors, the most common type of breast cancer in women. Research from the American Cancer Society confirms that alcohol’s effect on estrogen and other hormones is among the primary reasons it raises breast cancer risk.
The Folate Depletion Factor
There is a third, less-discussed pathway that compounds the damage. Alcohol interferes with your body’s ability to absorb and utilize folate, a B vitamin that plays a critical role in DNA synthesis and methylation. Low folate levels impair the body’s ability to copy DNA accurately during cell division, which creates additional opportunities for mutations to arise and persist. Women who drink and also have low dietary folate intake appear to carry even greater breast cancer risk, though supplementation with folic acid may partially offset this effect.
The Oxidative Stress and Inflammation Connection
Alcohol metabolism generates reactive oxygen species (ROS), unstable molecules that damage cellular components including DNA, proteins, and lipid membranes. This oxidative stress activates inflammatory pathways like NF-kB, which promote cell survival, proliferation, and metastasis. Chronic low-grade inflammation is increasingly understood as a central driver of cancer initiation and progression, and regular alcohol consumption keeps this inflammatory switch in the “on” position.
Alcohol and Breast Cancer Risk: A Comparison at a Glance
The table below summarizes how different drinking levels correspond to breast cancer risk, based on the 2024 meta-analysis and related research. All risk figures are relative to non-drinkers (baseline = 1.00).
| Drinking Level | Approximate Daily Alcohol | Relative Risk of Breast Cancer | Risk Category |
|---|---|---|---|
| Non-drinker | 0 g/day | 1.00 (baseline) | Reference |
| Very light (less than 1 drink/day) | Under 10 g/day | 1.04 to 1.05 | Slightly elevated |
| Light to moderate (1 drink/day) | ~14 g/day | 1.10 | Moderately elevated |
| Moderate (2 drinks/day) | ~28 g/day | 1.18 to 1.30 | Elevated |
| Moderate-heavy (3 drinks/day) | ~42 g/day | 1.22 to 1.40 | Significantly elevated |
| Heavy (3+ drinks/day) | Over 45 g/day | 1.40 to 1.50+ | Substantially elevated |
| HRT users (1-2 drinks/day) | ~14 to 28 g/day | ~3.00 (combined HRT + alcohol) | Markedly elevated |
Note: Relative risk above 1.00 indicates increased breast cancer risk compared to non-drinkers. Individual risk depends on additional factors including family history, genetic mutations, age, body weight, and reproductive history.
Who Is Most at Risk? Factors That Compound the Alcohol-Breast Cancer Connection
Alcohol does not exist in a vacuum. Its impact on breast cancer risk is shaped by your broader health profile. Some women face a more pronounced increase in risk because of factors that interact with alcohol’s biological mechanisms.
Age and Menopausal Status
Research consistently shows that the alcohol-breast cancer association is particularly strong among postmenopausal women, likely because estrogen levels are already shifting and breast tissue is responding differently to hormonal signals during this period. That said, premenopausal breast cancer risk is also elevated by alcohol consumption, with studies confirming the association holds regardless of menopausal status.
Body Weight and Body Composition
Because aromatase activity is higher in adipose (fat) tissue, women with a higher body mass index already convert more androgens to estrogens at baseline. When alcohol further boosts aromatase activity on top of that, the estrogen amplification effect is more pronounced. Maintaining a healthy weight is itself a breast cancer protective factor, and it compounds the benefit of reducing alcohol intake.
Family History and Genetic Risk
If you carry a family history of breast cancer or have been tested positive for BRCA1 or BRCA2 mutations, the alcohol-breast cancer picture becomes more nuanced. Some studies suggest the mechanism through which alcohol primarily raises risk, via ER+ hormone signaling, may not amplify BRCA1-related hereditary cancers in the same way. However, alcohol’s DNA-damaging and inflammation-promoting effects are universal, and women at already elevated genetic risk are generally advised to limit or eliminate all modifiable risk factors wherever possible.
Oral Contraceptive Use
Women who use oral contraceptive pills (OCPs) alongside regular alcohol consumption may face additional risk. Blood levels of acetaldehyde are elevated during the high estradiol phase of the menstrual cycle among women who drink, and this effect is amplified among women using OCPs. The intersection of hormonal contraception and regular alcohol intake is an underexplored area that deserves more attention in public health messaging.
What Can You Actually Do? Practical Guidance for Reducing Your Risk
The research does not ask you to be perfect. It simply makes the tradeoffs transparent. Here is what the evidence supports, translated into real-world actions.
Reduce, Not Just “Moderate”
The new language from the 2025-2030 Dietary Guidelines is deliberate: the goal is to drink less, not simply to stay within a defined limit. Every drink you eliminate or reduce counts. There is no minimum reduction threshold below which the benefit disappears. Even cutting from three drinks a day to one is a meaningful move in the right direction.
Prioritize Alcohol-Free Days
If quitting entirely feels overwhelming or unrealistic, building in consistent alcohol-free days is a practical and effective starting point. Three or four alcohol-free days per week meaningfully lowers your average weekly alcohol exposure and gives your liver’s detoxification systems adequate recovery time.
Optimize Your Folate Intake
Because alcohol depletes folate, women who drink are well-advised to ensure adequate dietary folate intake through foods like dark leafy greens, legumes, fortified grains, and citrus fruits. A daily multivitamin containing folic acid can also help offset some of the folate-depleting effects of alcohol, though it is not a substitute for reducing consumption itself.
Talk to Your Doctor Honestly
Alcohol is one of those topics that tends to get minimized or sidestepped in routine medical appointments, both by patients who underreport their intake and by clinicians who feel uncomfortable raising it. If you have a family history of breast cancer, are on HRT, use oral contraceptives, or carry any elevated breast cancer risk factors, proactively ask your doctor about the alcohol piece of your risk picture. You deserve a complete picture, not a sanitized one.
Know Your Mammography Schedule
None of this replaces early detection. Regular mammography screening is still one of the most powerful tools available for catching breast cancer at its most treatable stage. The 5-year survival rate for breast cancer detected at an early, localized stage is dramatically better than for cancers caught at advanced stages. Reducing alcohol intake and committing to your screening schedule are not competing priorities. They work together.
The Cultural Disconnect: Why Women Are Drinking More and Hearing Less
It would be incomplete to talk about alcohol and breast cancer without acknowledging the social and cultural context in which women drink today.
Over the past two decades, alcohol marketing has increasingly targeted women with products, messaging, and cultural narratives designed to make drinking feel empowering, glamorous, or self-care adjacent. “Wine mom” culture, rosé aesthetics, and cocktail brunch imagery have become ubiquitous. Meanwhile, the cancer risk data has been largely confined to academic journals, clinical guidelines, and occasional health news stories that rarely get the same traction as a sponsored Instagram post.
Drinking rates among women have also climbed. Research shows that while men still drink more overall, the gender gap in alcohol consumption has been narrowing for years, and alcohol use disorder diagnoses have risen faster among women than men over recent decades. The physiological sensitivity also matters here. Women have lower total body water content than men, which means the same amount of alcohol produces higher blood alcohol concentrations in a woman than in a man of equivalent weight. Women process alcohol less efficiently, and at the cellular level, their breast tissue is particularly responsive to the estrogenic effects that alcohol amplifies.
The Surgeon General’s 2025 advisory was historic partly because it placed this information where it has never publicly appeared before: on the product itself. Whether Congress moves to mandate updated warning labels remains to be seen. But the science is settled, and every woman deserves to make her relationship with alcohol with full knowledge of what that relationship entails for her health.
Conclusion: Information Is the Real Power Move
None of this is about guilt or judgment. Millions of women drink alcohol, most of them casually, socially, and without any thought that their nightly glass of wine carries a calculable and real effect on their breast cancer risk. The goal of this article is not to make you feel bad about choices you have already made. It is to give you the information you need to make better-informed choices going forward.
The statistics are real. The biology is understood. The risk is modifiable. That last point is the most important one. Unlike your age, your family history, or your genetic makeup, what you choose to drink is a variable you control. And the research is consistent that less alcohol means lower breast cancer risk, from the very first drink you choose not to pour.
You do not need to be perfect. You need to be informed. And now you are.
Read Next and Take Action
Share this article with a woman you care about. Most women do not know these statistics. The ones in your life deserve to. Send this to a friend, a sister, a colleague, a mother. It might be the most useful thing you forward this year.
Drop a comment below: Did any of these statistics surprise you? Are you reconsidering your relationship with alcohol after reading this? We would love to hear from you.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for guidance specific to your personal health circumstances.



