9 Proven Ways to Permanently Get Rid of Bacterial Vaginosis Without Antibiotics — Methods That Actually Deliver Real Results
You’ve taken the antibiotics. You felt better for two weeks. Then it came back, as if it never left.
If that story sounds painfully familiar, you are not alone, and more importantly, you are not out of options.
Why Antibiotics Keep Failing You (And What That Means for Your BV)
Bacterial vaginosis is the most common vaginal infection in women aged 15 to 44. According to the Centers for Disease Control and Prevention, roughly 21 million American women experience BV each year. Yet despite how widespread it is, it remains stubbornly misunderstood, even by the medical community.
The standard prescription is metronidazole or clindamycin. Both are antibiotics that work by killing the overgrown harmful bacteria. And they do work, at first. Studies show that about 80% of women are symptom-free after initial treatment. The catch? Within three months, nearly 50% experience a recurrence. Within a year, that number climbs to 70%.
So why does BV keep returning? Because antibiotics treat the symptom, not the root cause.
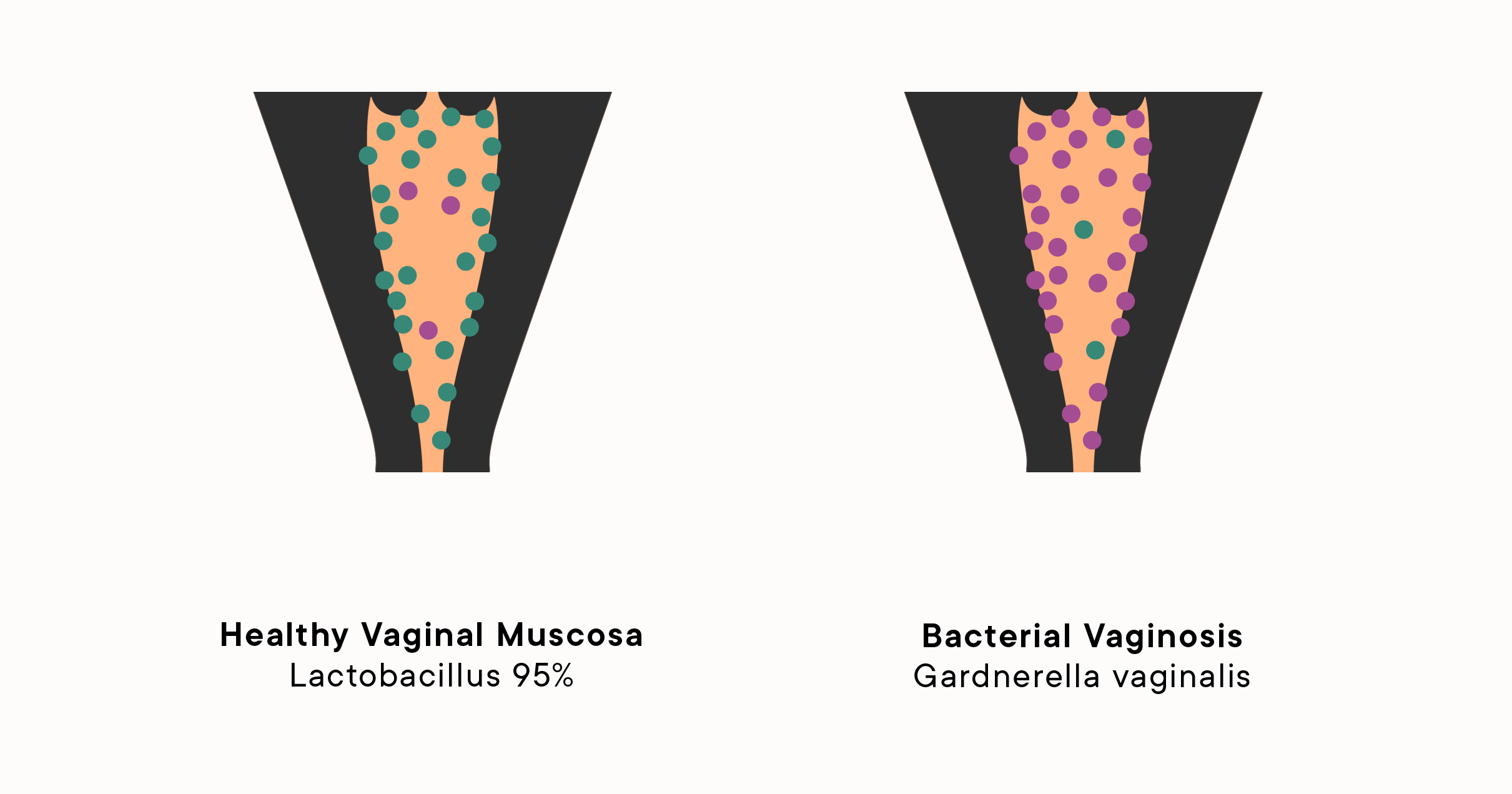
BV is not caused by a single “bad” bacterium the way strep throat is. It is a complex imbalance of the vaginal microbiome, a shift where protective Lactobacillus bacteria are outnumbered by anaerobic bacteria like Gardnerella vaginalis, Prevotella, and others. Antibiotics wipe out both the harmful and the helpful bacteria indiscriminately, leaving the vaginal environment vulnerable to recolonization.
The goal of lasting recovery is not just to kill bacteria. It is to rebuild and sustain a healthy vaginal ecosystem that naturally resists imbalance.
That is exactly what the nine methods in this article help you do.
These are not folk remedies from a wellness blog written by someone without a biology degree. These are approaches grounded in peer-reviewed research, microbiome science, and the lived experiences of women who have finally broken the BV cycle. Some of them work best in combination. All of them are worth understanding.
Let us get into it.
1. Repopulate Your Vaginal Microbiome With Targeted Probiotics to Get Rid of Bacterial Vaginosis Without Antibiotics
If BV is a story of microbial imbalance, then probiotics are the plot twist where the good guys come back.
The vaginal microbiome of a healthy, premenopausal woman is dominated by Lactobacillus species, most commonly Lactobacillus crispatus, Lactobacillus iners, Lactobacillus jensenii, and Lactobacillus gasseri. These bacteria produce lactic acid, which keeps vaginal pH low (typically between 3.8 and 4.5). That acidic environment is inhospitable to the anaerobic bacteria responsible for BV.
When Lactobacillus populations crash, pH rises, and opportunistic bacteria rush in. Probiotics aim to reverse that process by directly reintroducing beneficial strains.
What the research says
Multiple clinical trials have tested oral and vaginal probiotic supplementation for BV treatment and prevention. A 2019 meta-analysis published in the journal Infectious Diseases and Therapy found that women who received Lactobacillus-containing probiotics alongside or after antibiotic treatment had significantly lower recurrence rates compared to those who received antibiotics alone.
Another study out of Italy found that vaginal suppositories containing L. crispatus reduced BV recurrence by over 60% in women with a history of repeat infections.
How to use probiotics effectively for BV
The key is specificity. Not all probiotics are created equal, and most grocery store yogurt cultures will not deliver the strains or concentrations needed to shift your vaginal microbiome.
Look for supplements that contain:
- Lactobacillus rhamnosus GR-1 and Lactobacillus reuteri RC-14 (the most clinically studied combination for vaginal health)
- Colony-forming units (CFUs) of at least 5 billion per dose
- Enteric-coated capsules or refrigerated products to preserve viability
Some women also use vaginal probiotic suppositories (brands like Jarrow Femdophilus or Lactin-V) for more direct delivery. For oral probiotics, consistency matters more than dosage. Taking them daily for at least eight to twelve weeks gives the microbiome time to genuinely shift.
Probiotic-rich foods like plain Greek yogurt (unsweetened), kefir, kimchi, and sauerkraut can supplement capsule use, though they should not replace a high-quality targeted supplement.
2. Use Boric Acid Suppositories to Restore Vaginal pH and Beat Bacterial Vaginosis Without Antibiotics
Boric acid sounds alarming. It is the same compound used in pest control, which makes it understandable that women are sometimes hesitant. But context matters enormously here.
Used vaginally in small, precisely measured doses, boric acid is a well-established and increasingly mainstream treatment for recurrent BV and yeast infections. It works by directly acidifying the vaginal environment, disrupting the biofilms that harmful bacteria use to anchor themselves, and creating conditions where Lactobacillus can thrive again.
What makes boric acid different from antibiotics
Antibiotics are systemic. Even a topical antibiotic cream affects the broader microbial balance. Boric acid is targeted and pH-specific. It does not kill bacteria the way antibiotics do. Instead, it changes the chemical environment so that anaerobic bacteria cannot survive, while simultaneously making the habitat more hospitable for the beneficial strains you want to reintroduce.
This is a meaningful distinction. Boric acid does not create the post-treatment vacuum that antibiotics leave behind.
How to use boric acid suppositories safely
- Use 600 mg boric acid suppositories (available over the counter or compounded by a pharmacist)
- Insert one suppository vaginally at bedtime for 7 to 14 consecutive nights
- For recurrence prevention, some gynecologists recommend twice-weekly use for several months
- Never take boric acid orally. It is toxic when ingested. Vaginal use in suppository form is safe for adults when used as directed.
- Do not use during pregnancy.
A 2011 study in the Journal of Women’s Health found that boric acid was effective in resolving BV in 92% of women who had not responded to standard antibiotic therapy. For women with recurrent BV, it is increasingly recommended as a first-line option by integrative gynecologists.
Pair boric acid treatment with a probiotic regimen to get the best of both approaches: acid to reset the environment, probiotics to repopulate it with protective strains.
3. Adjust Your Diet to Support Vaginal Microbiome Health and Get Rid of BV Naturally
What you eat feeds every microbiome in your body, including the one in your vagina. This is not a metaphor. The gut microbiome and vaginal microbiome are connected through a pathway researchers call the gut-vagina axis.
When the gut is rich in Lactobacillus species, colonization of the vaginal tract with beneficial bacteria is more likely. When the gut is inflamed or dysbiotic (overrun with harmful strains), that imbalance can travel south, quite literally.
Foods that promote vaginal health
A diet that supports your vaginal microbiome looks remarkably like a diet that supports your overall health. No surprises there.
Prioritize:
- Fermented foods (yogurt, kefir, kimchi, miso, tempeh)
- Prebiotic-rich foods that feed Lactobacillus: garlic, onions, leeks, asparagus, bananas, oats
- Leafy greens and vegetables high in folate
- Probiotic-rich foods as described above
- Water (adequate hydration supports mucous membrane health)
Reduce or eliminate:
- Refined sugars and high-glycemic carbohydrates, which feed the overgrowth of anaerobic bacteria
- Alcohol, which disrupts gut flora and vaginal pH
- Processed foods high in preservatives and artificial additives
- Sweetened drinks, including fruit juice
The sugar connection
This one deserves emphasis. Anaerobic bacteria like Gardnerella thrive in glucose-rich environments. A diet high in refined sugar does not just affect your weight or blood sugar. It can directly fuel the bacterial overgrowth that causes BV.
A 2020 observational study found that women with BV consumed significantly more refined carbohydrates than women without it. While correlation is not causation, the mechanism is biologically plausible and consistent with what microbiome researchers know about bacterial feeding behavior.
Cutting back on sugar is not a magic cure, but it removes a key source of fuel for the organisms you are trying to crowd out.
4. Practice Strict Vaginal Hygiene (Without Over-Cleaning) to Prevent Bacterial Vaginosis From Returning
Here is one of the great paradoxes of vaginal health: many women get BV partly because they are trying too hard to be clean.
The vagina is a self-cleaning organ. It maintains its own pH, produces its own protective discharge, and manages its own bacterial populations without any external intervention. When well-meaning hygiene practices disrupt that internal system, the results can be counterproductive.
What disrupts vaginal balance
- Douching is the biggest offender. Multiple studies have confirmed that douching increases the risk of BV by washing away protective Lactobacillus bacteria and disrupting pH. If you douche regularly and experience recurring BV, stopping is one of the most impactful changes you can make.
- Scented soaps, washes, and sprays used inside or around the vaginal opening can alter pH and kill beneficial bacteria.
- Antibacterial soaps used externally in the vulvar area can strip natural protective microflora.
- Tight synthetic underwear traps heat and moisture, creating a breeding ground for anaerobic bacteria.
What good vaginal hygiene actually looks like
- Wash the external vulva only with warm water, or a very mild unscented soap
- Never insert soap, water, or any product into the vaginal canal itself
- Wear breathable cotton underwear and change it daily
- Change out of wet swimsuits or workout clothes promptly
- Wipe front to back after using the bathroom
- Sleep without underwear occasionally to allow airflow
These seem like small things. But for women with recurring BV, eliminating a daily disruption like scented washes can break the cycle of recurrence on its own.
5. Use Hydrogen Peroxide to Get Rid of Bacterial Vaginosis Without Antibiotics
Hydrogen peroxide (H2O2) as a BV treatment is one of the most clinically interesting developments in non-antibiotic management of vaginal infections.
Here is the reason it makes biological sense: healthy Lactobacillus bacteria naturally produce hydrogen peroxide as part of their metabolic activity. This H2O2 is part of what gives them their antimicrobial punch. Women with BV often have diminished or absent H2O2-producing Lactobacillus strains.
Introducing low-concentration hydrogen peroxide vaginally effectively replicates what a healthy microbiome would already be doing.
What the research shows
A landmark Italian study by Dr. Sena Riccardo followed 58 women with recurrent BV who were treated with vaginal douches of 3% hydrogen peroxide solution rather than antibiotics. After six months, 89% had no recurrence. That is a remarkable outcome compared to antibiotic recurrence rates.
More recently, a 2021 clinical trial published in BJOG: An International Journal of Obstetrics and Gynaecology tested a gel formulation of hydrogen peroxide against metronidazole. The hydrogen peroxide gel showed comparable cure rates at one month, with fewer side effects.
How to use it
- Use a 3% hydrogen peroxide solution (standard drugstore variety)
- Some protocols involve a vaginal douche with diluted solution (one part H2O2 to one part water) once daily for one week
- More recently, H2O2 gel products formulated specifically for vaginal use (such as Hydrogen Peroxide Gel by MedGyn or similar compounded products) are available for a more controlled application
- Always consult a healthcare provider before starting, particularly if pregnant or immunocompromised
This method works best when paired with probiotics to help repopulate the beneficial strains that will naturally continue producing H2O2 after treatment ends.
6. Try Tea Tree Oil (With Caution) to Support Natural BV Treatment
Tea tree oil has legitimate antimicrobial properties. Several laboratory studies have confirmed that it demonstrates activity against Gardnerella vaginalis, the primary bacterium associated with BV, as well as against Candida species, meaning it may simultaneously help prevent the yeast infections that sometimes follow BV treatment.
The active compounds, terpinen-4-ol in particular, disrupt the cell membranes of harmful bacteria without being broadly antibiotic in the way pharmaceutical agents are.
Using tea tree oil safely
The vaginal mucosa is extremely sensitive. Undiluted essential oils can cause chemical burns. This is not a risk worth taking.
If you choose to explore tea tree oil:
- Always dilute it. A common safe dilution for vaginal-adjacent use is 2 to 4 drops of tea tree essential oil per ounce of carrier oil (coconut oil, fractionated coconut oil, or almond oil work well).
- Use it externally on the vulvar area only, not inserted into the vaginal canal.
- Some women use diluted tea tree oil on a tampon or suppository base for internal use; this requires very careful dilution and ideally guidance from an integrative practitioner.
- Perform a patch test on the inner forearm before any first use.
- Do not use if pregnant.
The evidence for tea tree oil is promising but not yet as robust as for probiotics or boric acid. Consider it a supportive tool rather than a standalone treatment, especially for internal BV.
7. Address Sexual Health Factors That Contribute to Recurring Bacterial Vaginosis
This is a section many guides leave out, possibly because it requires some uncomfortable honesty. But ignoring the sexual health dimension of BV leaves a significant gap in any treatment plan.
BV is not technically classified as a sexually transmitted infection. However, sexual activity is one of the most consistent risk factors for both initial BV and recurrence.
Why sex matters in BV recurrence
Semen is alkaline, with a pH between 7.2 and 8.0. The vaginal environment is acidic (pH 3.8 to 4.5). Each exposure to semen temporarily raises vaginal pH, creating a window of vulnerability. For women with already marginal Lactobacillus populations, this repeated disruption can tip the balance toward BV.
Additionally, there is evidence suggesting that the penile microbiome of a male partner can harbor BV-associated bacteria. In heterosexual couples where the woman has recurrent BV, some research suggests that reinfection from the partner may be part of the cycle.
In women who have sex with women, BV transmission between partners has been documented, and concurrent treatment of both partners has shown better outcomes in small studies.
What you can do
- Use condoms consistently, particularly with new or multiple partners. Condom use has been shown in several studies to reduce BV incidence significantly.
- Consider discussing partner treatment with a healthcare provider if BV recurs repeatedly despite other interventions.
- Urinate after sex and rinse the external vaginal area with water to help restore pH.
- Some women find a boric acid suppository inserted after sex helps buffer the pH disruption from semen.
None of this is about shame or blame. It is about understanding all the variables in your personal BV puzzle.
8. Manage Stress and Sleep to Support Your Immune System’s Role in Fighting BV Without Antibiotics
Chronic stress is a microbiome killer. That is not hyperbole. It is supported by a growing body of research in psychoneuroimmunology, the field that studies how the mind, nervous system, and immune function are interconnected.
When the body is under chronic stress, cortisol levels remain elevated. Elevated cortisol suppresses immune function, disrupts gut bacteria, alters mucosal immunity, and yes, affects the vaginal microbiome. Stress also tends to correlate with poorer sleep, poorer dietary choices, increased alcohol consumption, and higher inflammation, all of which are independent risk factors for BV.
The stress-BV connection
A 2007 study in the American Journal of Obstetrics and Gynecology found that women who reported high levels of perceived stress were significantly more likely to have BV, even after controlling for other risk factors. A follow-up analysis suggested that stress-related immune suppression may reduce the vaginal immune system’s ability to maintain Lactobacillus dominance.
Sleep matters just as directly. During deep sleep, the body produces cytokines, immune proteins that help regulate inflammation and microbial balance. Chronic sleep deprivation suppresses this repair process.
Practical interventions
- Aim for 7 to 9 hours of quality sleep per night
- Practice stress-reduction techniques that work for you: breathwork, meditation, yoga, regular exercise, time in nature, therapy
- Reduce caffeine and screen exposure in the two hours before bed
- Consider adaptogens like ashwagandha or rhodiola (with practitioner guidance) if chronic stress is a significant factor
Treating BV without addressing stress is like trying to fill a bucket that has a hole in it. The interventions may work temporarily, but the underlying vulnerability remains.
9. Consider Functional Medicine and Targeted Supplements to Permanently Get Rid of Bacterial Vaginosis
Sometimes recurring BV is a signal from the body that something upstream needs attention. Nutritional deficiencies, hormonal imbalances, and gut dysbiosis can all compromise vaginal health from the inside out.
A functional medicine approach to BV looks beyond the vagina and asks why the microbiome keeps failing to stabilize.
Nutritional supplements with evidence for BV
Several supplements have shown promise in supporting vaginal microbiome health and reducing BV recurrence:
- Folate (Folic Acid or Methylfolate): A deficiency in folate has been associated with increased BV risk in multiple epidemiological studies. Women with BV have been found to have significantly lower serum folate levels. Supplementing with 400 to 800 mcg daily may provide protective benefit.
- Vitamin D: Low vitamin D is linked to disrupted vaginal immune function. A 2019 study in Nutrients found that vitamin D supplementation alongside standard BV treatment significantly reduced recurrence rates. Many women are deficient, particularly in northern latitudes and during winter months. Testing your levels is worthwhile.
- Zinc: Zinc plays a role in immune function and has shown some antimicrobial activity against BV-associated bacteria in laboratory settings. Dietary sources include pumpkin seeds, chickpeas, and beef.
- N-Acetyl Cysteine (NAC): NAC is a precursor to glutathione and has been studied for its ability to disrupt bacterial biofilms. Since Gardnerella vaginalis forms protective biofilms that make it resistant to both antibiotics and the immune system, NAC may help break down these biofilms and allow other treatments to work more effectively. A 2016 Italian study found that vaginal NAC gel significantly reduced BV recurrence.
Working with a functional or integrative practitioner
If BV has been recurring for more than a year despite multiple treatment attempts, it is worth seeking out a naturopathic doctor, integrative gynecologist, or functional medicine practitioner who can run comprehensive testing, including vaginal microbiome panels, nutrient levels, hormone panels, and gut microbiome analysis.
This level of investigation goes beyond what most conventional gynecologists have time for in a standard appointment. But for women with chronic, treatment-resistant BV, it can be genuinely life-changing.
A comprehensive overview of the vaginal microbiome and its connection to women’s health is available from the National Institutes of Health’s research portfolio, which provides in-depth insight into the science behind Lactobacillus dominance and what disrupts it.
Comparison Table: BV Treatment Methods at a Glance
| Treatment Method | Evidence Strength | Best For | Typical Duration | Side Effects | Use Alone or Combine? |
|---|---|---|---|---|---|
| Targeted Probiotics (L. rhamnosus GR-1 + L. reuteri RC-14) | Strong (multiple RCTs) | Prevention and long-term rebalancing | 8–12 weeks minimum | Minimal | Best combined |
| Boric Acid Suppositories | Strong (clinical trials) | Recurrent BV, antibiotic-resistant cases | 7–14 days acute, then maintenance | Mild discharge | Combine with probiotics |
| Dietary Changes (low sugar, fermented foods) | Moderate (observational) | Supporting microbiome long-term | Ongoing lifestyle | None | Combine with all |
| Improved Vaginal Hygiene | Strong (prevention data) | Preventing recurrence, breaking douching habit | Permanent change | None | Combine with all |
| Hydrogen Peroxide (vaginal) | Moderate-Strong (RCTs) | Acute BV resolution, antibiotic alternative | 7 days | Mild irritation possible | Combine with probiotics |
| Tea Tree Oil (diluted, external) | Limited (lab studies) | Mild external support | Short-term | Irritation if undiluted | Supportive use only |
| Sexual Health Practices (condoms, partner treatment) | Strong (epidemiological) | Recurrent BV linked to sexual activity | Ongoing | None | Combine with all |
| Stress and Sleep Management | Moderate (observational) | Chronic recurrence, immune support | Ongoing | None | Combine with all |
| Functional Medicine and Supplements (Vitamin D, Folate, NAC) | Moderate (clinical studies) | Treatment-resistant or root-cause BV | 3–6 months testing and supplementation | Varies by supplement | Combine with targeted approach |
How These Methods Work Together: Building Your Personal BV-Free Protocol
No single method in this list is likely to permanently resolve recurrent BV on its own. The women who achieve lasting results almost universally use a combination approach, addressing the problem from multiple angles simultaneously.
A practical starting framework might look like this:
Phase 1 (Weeks 1 to 2): Reset
Start boric acid suppositories every night for 7 to 14 days. Begin a targeted probiotic supplement daily. Eliminate douching, scented products, and reduce sugar intake starting immediately.
Phase 2 (Weeks 3 to 8): Rebuild
Continue daily probiotics. Incorporate dietary changes and fermented foods consistently. Begin a sleep hygiene routine if sleep quality has been poor. Consider adding vitamin D and folate supplementation after testing your baseline levels.
Phase 3 (Months 3 and beyond): Maintain
Continue probiotics long-term. Use boric acid suppositories after sexual activity or menstruation if those are identified triggers. Maintain dietary and hygiene practices. Revisit with a functional practitioner if recurrence continues.
The Office on Women’s Health provides additional guidance on understanding and managing bacterial vaginosis, including when to seek medical care, which is always recommended if symptoms are severe or accompanied by fever or pelvic pain.
When to See a Doctor Even While Pursuing Natural Treatments
Natural approaches to BV are not a reason to avoid medical care entirely. There are situations where prompt medical attention is essential.
See a healthcare provider if:
- Symptoms are severe or rapidly worsening
- You experience pelvic pain, fever, or chills alongside vaginal symptoms (these may indicate pelvic inflammatory disease, a serious condition)
- You are pregnant (BV during pregnancy is associated with preterm birth and must be treated under medical supervision)
- Symptoms persist or worsen after two weeks of natural treatment
- You are immunocompromised due to HIV, chemotherapy, or other conditions
- Symptoms change significantly in character (new bleeding, sores, or extreme pain)
Natural and conventional approaches can be used together. Many integrative gynecologists support a combined protocol, antibiotics when necessary for acute resolution, followed by natural methods for microbiome restoration and long-term prevention.
The Bigger Picture: Understanding Your Vaginal Microbiome Is Empowering
Here is the thing nobody tells you when you sit in the exam room getting your third BV prescription in two years. Your body is not broken. You are not uniquely unlucky. And you are not powerless.
BV is not a moral failing. It is not caused by being “dirty.” It is a complex ecological imbalance influenced by genetics, sexual activity, hormones, diet, stress, hygiene practices, and the particular bacterial strains you have been exposed to over your lifetime.
Understanding that makes it something you can actually work with, rather than something that simply happens to you.
The vaginal microbiome is one of the most active and dynamic ecosystems in the human body. It responds, sometimes dramatically, to the inputs you give it. Feed it well. Reduce the disruptions. Support its protective bacteria. Give it time.
Most women who commit to this multi-faceted approach see meaningful improvement within two to three months. Many achieve lasting resolution. That outcome is worth pursuing.
Conclusion
Recurring BV is exhausting, physically and emotionally. The cycle of antibiotics, temporary relief, and relapse leaves women feeling like something is fundamentally wrong with their bodies. Nothing is fundamentally wrong. The system just needs different support than a ten-day antibiotic course provides.
The nine methods covered here, probiotics, boric acid, dietary changes, improved hygiene, hydrogen peroxide, tea tree oil, sexual health practices, stress management, and targeted supplementation, all work toward the same underlying goal: restoring and sustaining a vaginal microbiome that can defend itself naturally.
Start with the approaches that feel most accessible. Build from there. Give each intervention adequate time to work. And remember that the women who succeed long-term usually do so by treating this as a lifestyle recalibration, not a quick fix.
Your vaginal health is not a side note to your overall health. It is part of it. You deserve to feel comfortable, confident, and free of BV, not just for two weeks, but for good.
Ready to Take Control of Your Vaginal Health?
If this article gave you a new perspective on BV treatment, share it with a friend who might be stuck in the same cycle. You never know who needs to read this today.
Have a question or a personal experience to share? Drop it in the comments below. Real conversations help more women than perfectly formatted articles ever will.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before beginning any new treatment, particularly if you are pregnant, immunocompromised, or experiencing severe or unusual symptoms.