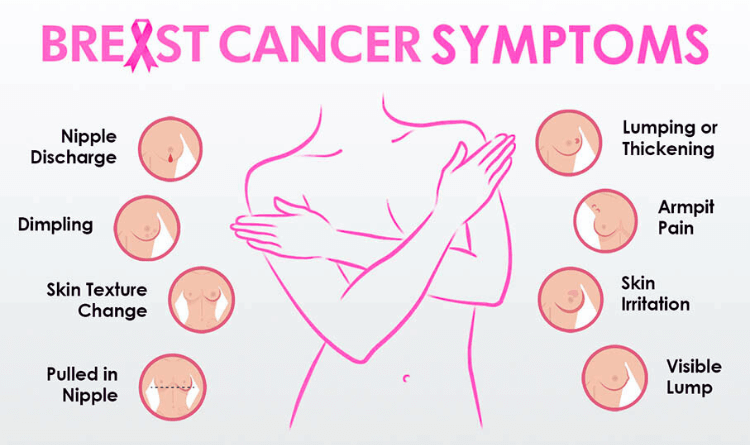
Breast Cancer Symptoms Women Should Never Ignore: 14 Warning Signs That Go Far Beyond a Simple Lump
You checked, you felt nothing unusual, and you moved on. Most women do. But here is the truth that nobody puts on a pink ribbon: a lump is just one way breast cancer announces itself, and it is not even the most common way women first notice something is wrong.
Why Breast Cancer Symptoms Go So Much Deeper Than a Lump
Most of us grew up hearing one piece of advice about breast health: check for a lump. And while that is not wrong, it is dangerously incomplete. Breast cancer is most often associated with having a breast lump. However, your symptoms may vary depending on your specific type of breast cancer. While it’s true that many patients have a lump, it is possible to have breast cancer with no lump at all.
That single blind spot has cost lives. Women dismiss a rash, explain away an ache, or attribute skin changes to getting older, gaining weight, or breastfeeding. Months pass. Then a year. Then a diagnosis arrives at a stage no one wanted.
In 2025, an estimated 316,950 women will be diagnosed with invasive breast cancer in the United States, with an additional 59,080 cases of non-invasive breast cancer expected. Those are not abstract numbers. Those are sisters, mothers, colleagues, and friends. And many of them had symptoms they did not recognize as symptoms.
This article is your complete, no-fluff guide to 14 breast cancer warning signs that go far beyond a lump. Reading this could be one of the most important health decisions you make this year. Not because cancer is inevitable, but because knowledge is what turns a late diagnosis into an early one.
Warning Sign #1: Skin Dimpling or Puckering, a Critical Breast Cancer Symptom
Imagine pressing your finger into an orange peel. That subtle, textured indentation is exactly what breast skin dimpling can look like, and it is one of the most telling breast cancer warning signs there is.
Breast dimpling, a localized change in the texture of the skin of the breast such as small indentations or puckering, isn’t always a sign of breast cancer. However, breast dimpling can be a significant sign of breast cancer that should be reported to your doctor right away.
Dimpling happens when a tumor pulls on the connective tissue beneath the skin, creating that telltale puckered appearance. It can appear anywhere on the breast surface, not just near the nipple. Many women first notice it when they raise their arms or bend forward while looking in a mirror.
What to look for:
- Localized skin that looks pulled inward
- An area of breast skin that no longer sits smoothly
- A texture resembling orange peel, especially over a larger portion of the breast
- Puckering that appears when you change position but may not be visible when standing still
If you see this, do not wait it out. Book an appointment within a week.
Warning Sign #2: Breast Swelling Without Any Detectable Breast Cancer Lump
Swelling that arrives without a noticeable lump underneath often gets written off as hormonal changes, water retention, or an underwire bra that fits badly. It is one of the most overlooked breast cancer symptoms, especially in younger women.
Sometimes, people notice swelling before they feel or see a lump. So it’s also important to see your doctor if it happens to you. The swelling may affect the whole breast or just one section of it. When only one breast is involved, or when swelling is persistent rather than cyclical, that is when the alarm bells should start ringing.
Swelling can also be the first visible sign of inflammatory breast cancer (IBC), an aggressive form of the disease that often presents with no distinct lump at all. IBC moves fast. When swelling accompanies warmth or skin changes, getting evaluated quickly is not optional.
Key distinctions:
- Swelling that does not fluctuate with your menstrual cycle
- One breast noticeably larger than the other, especially if this is new
- Swelling that feels warm or heavy to the touch
- Swelling in the upper chest area or near the collarbone
Warning Sign #3: Nipple Inversion, an Often-Missed Breast Cancer Warning Sign
A nipple that has recently turned inward, also called nipple retraction or inversion, is something that many women attribute to natural changes or aging. Sometimes it is. But when the change is new, it deserves prompt medical attention.
Not all flat or inverted nipples are signs of breast cancer. In fact, up to 20% of men and women naturally have flat or inverted nipples. However, flat or inverted nipples can be a symptom of breast cancer. If you are experiencing a flat or inverted nipple, especially if it is new for you, you should speak with your healthcare provider about it right away.
The critical word there is “new.” If your nipple has always been inverted, that is likely just anatomy. But if it has recently changed direction, become pulled in, or begun pointing differently than it used to, that shift in position may indicate a tumor beneath the surface pulling on the surrounding tissue.
Do not dismiss this. Take a photo if it helps you track the change over time, and then get it checked.
Warning Sign #4: Unusual Nipple Discharge Is One of the Earliest Breast Cancer Symptoms
Nipple discharge gets complicated fast. Not all discharge is dangerous. During pregnancy or breastfeeding, discharge is completely expected. But outside of those contexts, any discharge from the nipple should be reported to a doctor.
Nipple discharge other than breast milk, including blood, is a potential symptom of breast cancer. Clear, watery, or bloody discharge from one nipple, particularly when it occurs without squeezing, is the kind of discharge that warrants urgent attention. Discharge that comes from only one duct opening in the nipple is also more concerning than discharge that comes from multiple openings.
Unusual nipple discharge could be clear, bloody, or another color. Some women dismiss it as benign because it is not painful. But painlessness is not reassurance. Many breast cancer symptoms, including this one, are entirely pain-free.
Discharge that needs evaluation:
- Bloody or rust-colored discharge
- Clear or watery discharge in one breast
- Discharge that happens spontaneously, without any pressure
- Any discharge in a woman who is not pregnant or breastfeeding
Warning Sign #5: Breast Skin That Looks Like Orange Peel
This one has a name in medicine: peau d’orange, which is French for “skin of an orange.” When the skin on your breast takes on a dimpled, pitted texture that resembles citrus peel across a larger area, it is a red flag that should not wait.
Texture changes to the skin on your breast, such as a rash, redness, or dimpling, could see the skin resemble the peel of an orange. This pattern develops when cancer cells block lymphatic vessels in the skin, causing fluid to build up and create that distinctive pitted look. It is one of the hallmark signs of inflammatory breast cancer.
The tricky part is that this can develop quickly, sometimes within days or weeks. Women sometimes think it is a skin infection or an allergic reaction. Inflammatory breast cancer can mimic mastitis so convincingly that it gets misdiagnosed and treated with antibiotics before the underlying cancer is identified.
If you have orange-peel texture on any part of your breast, combined with redness or warmth, go to the emergency room or an urgent care center rather than waiting for a routine appointment.
Warning Sign #6: Redness, Warmth, or a Rash, the Breast Cancer Symptoms Most Likely to Be Dismissed
A rash on the breast is easy to brush off. Fabrics irritate skin. Sweat accumulates in summer. Eczema happens. But a rash that does not resolve, that keeps coming back, or that covers more than a small isolated area of the breast deserves a closer look.
Inflammatory breast cancer grows and spreads quickly, often spreading to nearby lymph nodes. IBC can also spread to organs such as the brain, bones, liver, and lungs if not diagnosed promptly. The rash associated with IBC is often described as sudden in onset, sometimes appearing overnight, and it tends to involve at least a third of the breast surface.
Then there is Paget’s disease of the breast, a rare but serious condition where cancer of the nipple can mimic eczema so convincingly that scaling and erythema of the nipple and/or areola can be misdiagnosed as eczema or other benign inflammatory conditions, such as dermatitis or psoriasis.
Symptoms of Paget’s disease of the breast may include flaky or scaly skin on the nipple, crusty or oozing or hardened skin that looks like eczema on the nipple or areola or both, and a burning sensation.
The rule of thumb here is simple. A breast rash that does not clear up within two weeks with standard treatment should be biopsied, not just treated with more cream.
Warning Sign #7: Changes in Breast Size or Shape, a Subtle But Real Warning Sign
Breasts change throughout life. Puberty, pregnancy, weight fluctuations, and menopause all shift how breasts look and feel. This is exactly why subtle changes in size or shape can slide past a woman’s awareness for months.
An unexplained change in the size or shape of the breast, including swelling or shrinkage of all or part of the breast, especially if on one side only, even if no lump is felt, can be a warning sign of breast cancer.
The key phrase is “one side only.” Both breasts naturally differ slightly in size, and that is normal. But a rapid or unexplained change that affects only one breast, whether it becomes visibly larger, smaller, or differently shaped, is worth investigating. A tumor does not have to be large to pull at surrounding tissue and distort the breast’s contour.
Check your profile in the mirror, not just the front view. Lean forward. Raise your arms above your head. Some changes only become visible in certain positions.
Warning Sign #8: Swollen Lymph Nodes in the Armpit or Collarbone Area
Many people are surprised to learn that breast cancer can announce itself first in the armpit, not in the breast itself. The lymph nodes under the arm and near the collarbone are often the first stop cancer cells make when they begin to spread.
Swollen lymph nodes under the arm or near the collar bone can sometimes be a sign of breast cancer spread even before the original tumor in the breast is large enough to be felt.
Cancerous lymph nodes typically feel hard, fixed or non-movable, and painless, unlike swollen nodes from infection which feel tender, soft, and mobile.
This is a crucial distinction to understand. Lymph nodes swell all the time when you are fighting a cold or an infection. Those nodes are tender and movable, and they go back to normal within a few weeks. But a hard, fixed node that doesn’t move, doesn’t hurt, and doesn’t go away is a different story entirely.
Palpate your armpits monthly, ideally lying down with your arm raised. If you find something that feels out of the ordinary and does not resolve within two to three weeks, see your doctor.
Warning Sign #9: Breast Pain or Tenderness Is Not Always Hormonal
Here is something that surprises most women: breast pain can be a breast cancer symptom, even though it is far more commonly caused by hormonal fluctuations, fibrocystic tissue, or poorly fitting bras. The distinction lies in the pattern.
Pain, tenderness, or burning in the breast or nipple could be the first sign of inflammatory breast cancer or Paget’s disease, which are among the rarer types of breast cancer.
Cyclical breast pain that reliably comes and goes with your menstrual period is almost always hormonal. It is the non-cyclical pain, pain that sits in one specific spot, that does not respond to typical cycle changes, that persists for more than two consecutive menstrual cycles, which should raise concern.
Symptoms of Paget’s disease may include a burning sensation and straw-colored or bloody nipple discharge. Any burning or aching localized to the nipple area specifically, outside of breastfeeding, deserves evaluation.
Track your pain in a note on your phone. Log where it is, how intense it feels on a scale of one to ten, whether it relates to your cycle, and how long it lasts. That information will help your doctor immensely.
Warning Sign #10: Skin Thickening or a Marble-Like Area Beneath the Skin
Not all breast cancer feels like a classic smooth or irregular lump. Some women describe finding an area that feels like a thickened patch, more like pressing on the heel of a hand than a distinct ball or mass. Others describe a marble-like area beneath the surface that feels unlike anything else in the breast.
A marble-like area under the skin that feels different from any other part of either breast is a possible symptom of breast cancer. Thickening without a distinct lump occurs when cancer infiltrates the tissue more diffusely, making boundaries harder to define.
Breast tissue thickening feels different from a distinct lump. It’s a firm, dense area that lacks clear borders. Dense breast tissue on mammography can mask tumors, making detection more challenging and highlighting the importance of clinical breast examination.
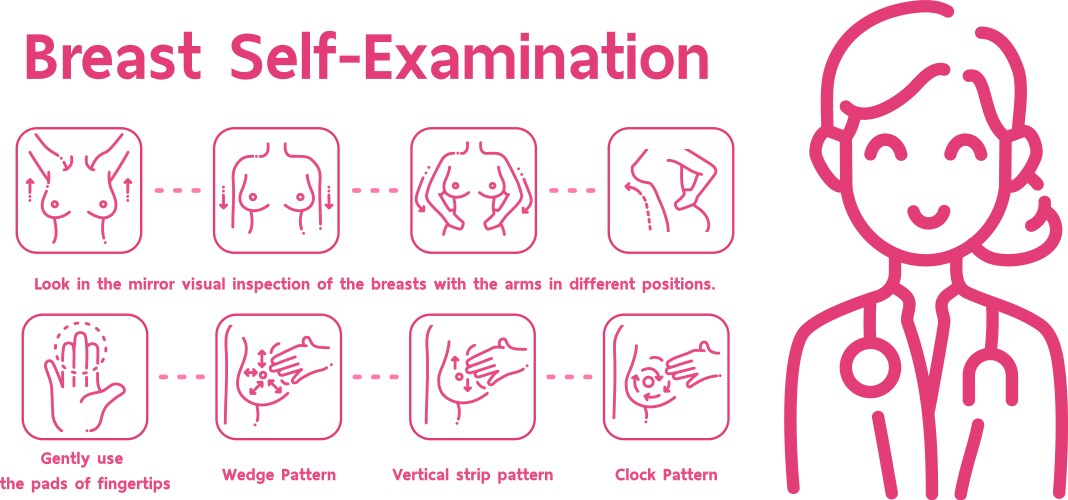
This is also why breast self-awareness matters more than any specific technique. You are not performing a clinical exam. You are learning what is normal for your body so that when something changes, you notice it.
Warning Sign #11: Flat or Indented Area on the Breast Surface
Picture a beach ball that has been slightly deflated on one side. A flat or sunken area on an otherwise rounded breast surface is exactly that kind of visual cue, and it is one of the less discussed breast cancer warning signs.
A flat or indented area on your breast could happen because of a tumor you can’t see or feel. A tumor that is located close to the surface but too small to feel may still exert enough traction on the overlying skin to create a slight flattening or indentation.
This sign is best identified by looking at your breasts carefully in a mirror with good lighting, in multiple positions, including with your arms raised. Many women never look at their breasts this deliberately. Taking two minutes each month to do so could make a life-saving difference.
Warning Sign #12: Changes to the Areola Area That Signal Breast Cancer
The areola, the darker skin surrounding the nipple, is not often discussed in the context of breast cancer symptoms. But changes to this area can be just as significant as changes to the nipple itself.
Scaly, red, or swollen skin on the breast, nipple, or areola is a potential sign of breast cancer. The areola can become discolored, take on a reddish or purple hue, develop a rash that does not heal, or begin to look crusted or flaky.
Initial findings in Paget’s disease of the breast often include itching, scaling, and crusting of and/or discharge from the nipple. The condition usually affects one breast. Early on, the skin symptoms may fluctuate, improving only to worsen again.
That fluctuating quality fools a lot of people. The symptom seems to improve, they assume it is resolved, and they stop paying attention. Weeks later it returns, worse than before. If a change to your areola keeps coming back, that is not reassurance. That is a pattern that needs investigation.
Warning Sign #13: Unexplained Changes in Breast Texture
Breast tissue is naturally varied in texture. Some women have naturally lumpy, dense tissue all the time. But a change in overall texture that is new, particularly in one specific area, is different from the baseline variation your breasts have always had.
Irritation or dimpling of breast skin and redness or flaky skin in the nipple area or the breast are potential symptoms of breast cancer. Texture changes can be subtle: a patch that feels rougher than the surrounding skin, an area that seems to have become stiffer, or skin that no longer moves smoothly over the tissue beneath it.
The American Cancer Society’s breast cancer signs and symptoms guide notes that changes in the skin texture, including discoloration, rash, swelling, or an enlargement of the pores in the breast skin, can all serve as warning signs worth reporting promptly to a healthcare provider.
New texture changes, especially in one breast and not the other, should not be attributed to aging without a professional evaluation ruling out something more serious.
Warning Sign #14: A Persistent Feeling That Something Is “Off”
This one does not show up in any clinical guidelines, but it belongs on this list. Many women diagnosed with breast cancer describe knowing, in a very physical, instinctive way, that something had changed, even before they could point to a specific symptom. A heaviness, a low-grade ache, a vague sense of pressure, a feeling that was simply different from how their body usually felt.
Trust that instinct. You are not being hypochondriacal. You are being body-aware, which is exactly what breast health education asks you to be.
It’s important for all women to be familiar with the way their breasts normally look and feel. This is called breast self-awareness. Having breast self-awareness makes it easier to notice any changes in your breasts that should be reported to your doctor.
If something feels different and you cannot quite name what it is, that is exactly the kind of observation worth mentioning at your next appointment. Doctors work with vague descriptions every day. “Something just feels off” is a valid medical statement.
Breast Cancer Warning Signs at a Glance: Comparison Table
The table below covers all 14 warning signs, the area of the breast most commonly affected, whether the symptom is more commonly associated with a specific cancer type, and what urgency level to apply when seeking care.
| Warning Sign | Location | Possible Cancer Type | Urgency Level |
|---|---|---|---|
| Skin dimpling or puckering | Breast surface | All types, esp. IBC | High, see doctor within 1 week |
| Swelling without a lump | Whole breast or one section | Inflammatory breast cancer | High, especially if sudden |
| Nipple inversion (new) | Nipple | Invasive ductal carcinoma | High, if new or worsening |
| Unusual nipple discharge | Nipple | Ductal carcinoma, Paget’s | High, especially if bloody |
| Orange-peel skin texture | Breast surface | Inflammatory breast cancer | Urgent, same day if widespread |
| Redness, warmth, or rash | Breast, nipple, or areola | IBC, Paget’s disease | High, if not resolved in 2 weeks |
| Changes in size or shape | Whole breast | All types | Moderate, within 2 weeks |
| Swollen lymph nodes | Armpit, collarbone | Spread from breast primary | High, especially if hard/fixed |
| Unexplained breast pain | Localized spot | IBC, Paget’s disease | Moderate if non-cyclical |
| Thickening or marble-like area | Within breast tissue | Invasive ductal carcinoma | High, within 1 week |
| Flat or indented area | Breast surface | All types | High, within 1 week |
| Areola changes | Areola and surrounding skin | Paget’s disease | High if crusting or bleeding |
| Unexplained texture changes | Skin surface, breast tissue | All types | Moderate, within 2 weeks |
| Persistent feeling something is “off” | Generalized | All types | Moderate, mention at next visit |
What to Do If You Notice Any of These Breast Cancer Symptoms
First, breathe. Most breast changes are not cancer. Most lumps are benign. Most rashes are dermatitis. Most discharge is hormonal. The goal of knowing these symptoms is not to send you into a spiral of anxiety every time your breast feels different. It is to ensure you do not minimize something that deserves professional evaluation.
If you notice a symptom of breast cancer, don’t panic. Instead, report any symptoms or changes to your doctor immediately. While most lumps are not breast cancer, all breast changes including the symptoms listed above need to be investigated by a healthcare professional. Remember, you don’t need to have all of the symptoms of breast cancer. Having even one symptom is enough reason to contact your doctor.
Here is what to do next:
- Document the change. Take a photo if it is visible, note when it started, whether it has changed, and what other factors might be relevant like where you are in your menstrual cycle.
- Call your doctor. Do not wait for your annual appointment if you notice something new and persistent. Call and describe what you are seeing or feeling. Most practices will fit you in within one to two weeks for a breast concern.
- Ask for imaging. The U.S. Preventive Services Task Force recommends biennial mammography screening for women aged 40 to 74 at average risk, with the option for annual screening based on individual preference. Updated 2024 guidelines lowered the screening age from 50 to 40 years due to increasing breast cancer incidence in younger women.
- Ask about ultrasound if you have dense breast tissue. Research published in the NIH database shows that combining mammography with ultrasound increases breast cancer detection rates by 97.3% compared to mammography alone in women with dense breast tissue.
- Push back if you feel dismissed. You know your body. If a symptom persists and you feel your concern is not being taken seriously, ask for a second opinion. That is not being difficult. That is being your own best advocate.
The Importance of Regular Screening Alongside Knowing Breast Cancer Symptoms
Knowing your symptoms is not a substitute for routine screening, and routine screening is not a substitute for knowing your symptoms. Both are essential, and they work best together.
Regular mammograms are the most reliable way to catch breast cancer early, according to the American Cancer Society. But mammograms on their own can’t catch every case of breast cancer, which is why it’s important to pay attention to changes in your breasts, because you know your body best.
Mammograms catch tumors before they are large enough to cause any symptoms. But they are not perfect, particularly in women with dense breast tissue, where cancers can hide in the imaging. This is why the symptom awareness you have built by reading this article is genuinely complementary to your screening schedule, not redundant with it.
The Mayo Clinic’s comprehensive breast cancer resource emphasizes that early detection, combining regular screening with prompt reporting of any physical changes, remains the most powerful tool available for improving breast cancer outcomes. Women who find cancer early have significantly more treatment options and significantly better long-term survival rates.
Schedule your mammogram if you are due. Book your annual well-woman visit if you have been putting it off. And the next time something in your breast feels or looks different, say something about it.
Conclusion: Your Breast Health Awareness Is Worth More Than You Know
Breast cancer does not always knock loudly. It does not always arrive as a hard, unmistakable lump that you find the moment you check. Sometimes it whispers through a skin texture that changed, a nipple that shifted inward, a rash that keeps returning, or a swelling that arrived without explanation.
The fourteen warning signs covered in this article are not meant to frighten you. They are meant to equip you. An informed woman who recognizes a rash on her nipple as a potential sign of Paget’s disease, or who understands that orange-peel skin is a red flag for inflammatory breast cancer, is a woman who can act quickly when it matters most.
Early detection saves lives. Not in the abstract. In the practical, daily, mundane reality of noticing something, making a phone call, and getting an answer while there is still every option on the table.
You are worth that phone call.
Share This, Take Action, and Keep Reading
This article could save a life. Share it with the women in your life, your mother, your sister, your best friend, your colleague, your daughter who just turned 20 and thinks this does not apply to her yet. Early awareness does not have an age limit.
Drop a comment below: Have you ever experienced a breast cancer symptom that wasn’t a lump? Did you recognize it right away or did it take time to connect the dots? Your story might be the nudge someone else needs to make that appointment.
Read Next:
This article is intended for general informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for concerns about your breast health or any symptoms you experience.