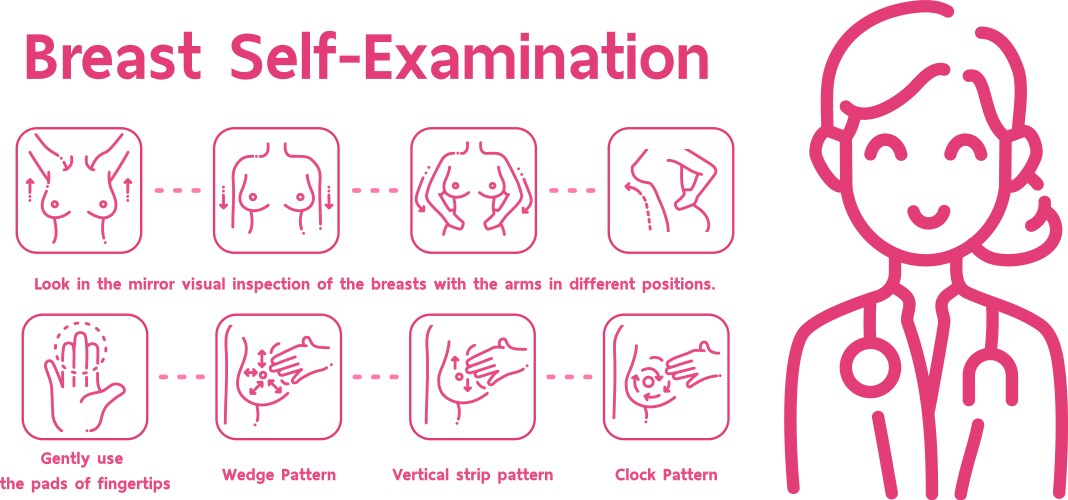
Early Detection Saves Lives: 9 Breast Cancer Screening Methods Beyond Mammograms, $7,800 Testing Comparison
One in eight women will hear the words “you have breast cancer” in her lifetime. But here’s the truth that changes everything: the women who survive, thrive, and beat this disease almost always have one thing in common. They found it early.
If you think a mammogram is your only line of defense, you’re operating with outdated information, and that gap in knowledge could genuinely cost you your life.
Why Understanding All Breast Cancer Screening Methods Matters More Than Ever
Let’s get real for a second. Most women walk into their annual check-up, get their mammogram, and assume they’ve done everything they can. And look, mammograms are excellent. They’ve saved countless lives since becoming a standard screening tool in the 1980s. But they are not perfect. They miss roughly 20% of breast cancers, and that number climbs significantly higher in women with dense breast tissue.
Here’s where things get personal. Dense breast tissue affects nearly half of all women over 40. If that’s you, a mammogram alone is like trying to spot a snowball in a snowstorm. The cancer tissue and the dense tissue both appear white on the image, making tumors incredibly difficult to detect. This isn’t a minor oversight. It’s a critical blind spot in the screening process that millions of women don’t even know exists.
The five-year survival rate for breast cancer caught at Stage 1 is 99%. At Stage 4, it drops to 30%. That difference, that enormous, life-altering gap, comes down to one thing: early detection. And early detection depends entirely on using the right breast cancer screening methods for your specific body, your risk level, and your medical history.
This article walks you through nine screening technologies that go beyond the standard mammogram. We’ll break down how each one works, who benefits most, what it costs, and how it compares to everything else on the market. Some of these tests cost as little as $50. Others run past $7,800 for comprehensive panels. By the end, you’ll know exactly which combination of breast cancer screening methods gives you the best possible chance of catching cancer before it has a chance to spread.
This isn’t about fear. It’s about power. Knowledge is the most potent weapon you have against this disease, and you deserve access to all of it.
Let’s dive in.
1. Digital Breast Tomosynthesis (3D Mammography): The Evolved Breast Cancer Screening Method
If the standard mammogram is a photograph, 3D mammography is a video. Digital breast tomosynthesis, commonly called 3D mammography, takes multiple X-ray images of the breast from different angles and reconstructs them into a three-dimensional picture. This layered approach allows radiologists to examine breast tissue one thin slice at a time, rather than viewing everything compressed into a single flat image.
The practical difference is enormous. Studies have consistently shown that 3D mammography reduces callback rates (those terrifying “we need you to come back for more imaging” phone calls) by up to 40%. It also increases invasive cancer detection rates by approximately 27% to 50% compared to traditional 2D mammography. For women with dense breast tissue, this technology is genuinely transformative.

How 3D Mammography Works
You’ll stand in front of the machine just like a standard mammogram. Your breast is still compressed between two plates (yes, still uncomfortable, but the compression is typically briefer). The X-ray arm sweeps in a small arc over the breast, capturing images at multiple angles in just a few seconds.
The entire process takes about 10 to 15 minutes. The radiation dose is slightly higher than a standard 2D mammogram, but newer systems have brought combination 2D/3D exams to roughly the same dose as a traditional mammogram alone. The FDA has approved 3D mammography as both a screening and diagnostic tool, and most major medical centers now offer it.
Who Should Consider This Screening Method
- Women with dense breast tissue (categories C and D on the BI-RADS density scale)
- Women of any age undergoing routine mammographic screening
- Women who have experienced previous false-positive results with 2D mammography
- Women with a family history of breast cancer who want enhanced standard screening
What It Costs
The cost of 3D mammography ranges from $50 to $100 above the cost of a standard mammogram, bringing the total to approximately $250 to $450 out of pocket without insurance. However, most insurance plans now cover 3D mammography at the same rate as standard mammograms, thanks to legislation passed in the majority of U.S. states. Under the Affordable Care Act, screening mammograms are covered with zero out-of-pocket cost for women over 40, and many insurers extend this coverage to include the 3D component.
What Results to Expect
You’ll typically receive results within one to two weeks. If something looks abnormal, you’ll be called back for additional imaging or a biopsy. The key advantage here is fewer unnecessary callbacks. Fewer false alarms mean less anxiety, fewer invasive follow-up procedures, and lower overall healthcare costs over time.
The important caveat: 3D mammography is an evolution, not a revolution. It’s still X-ray based, which means it still struggles somewhat with extremely dense tissue. Think of it as the best version of the mammogram family, but not a replacement for supplemental screening in high-risk women.
2. Breast MRI: The Gold Standard Among Advanced Breast Cancer Screening Methods
If you’re high-risk, this is the screening method that could save your life. Breast MRI (magnetic resonance imaging) uses powerful magnets and radio waves instead of radiation to create incredibly detailed images of breast tissue. It is the most sensitive breast cancer screening method currently available, detecting cancers that mammograms, ultrasounds, and physical exams all miss.
According to the American Cancer Society, breast MRI has a sensitivity rate of approximately 94% to 100% in detecting invasive breast cancer, compared to roughly 30% to 48% sensitivity for mammography in high-risk populations. That’s not a marginal improvement. That’s a fundamentally different level of detection capability.
How Breast MRI Works
You’ll lie face down on a padded table with your breasts positioned in a cushioned coil that helps capture the images. A contrast dye (gadolinium) is injected into your arm through an IV line. This dye highlights areas of increased blood flow, which is a hallmark of cancerous tissue because tumors grow their own blood supply through a process called angiogenesis.
The scan takes about 30 to 60 minutes. You’ll need to lie still during this time, and the machine is noisy (you’ll be given earplugs or headphones). For women who are claustrophobic, some centers now offer open MRI machines, though the image quality may be slightly reduced.
Who Should Consider This Screening Method
The American Cancer Society recommends annual breast MRI screening alongside mammography for women with:
- A lifetime risk of breast cancer of 20% to 25% or greater (based on risk assessment tools)
- A known BRCA1 or BRCA2 gene mutation
- A first-degree relative with a BRCA mutation, even if they haven’t been tested themselves
- A history of radiation therapy to the chest between ages 10 and 30
- Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome, or a first-degree relative with one of these conditions
Breast MRI is not currently recommended as a routine screening tool for average-risk women. This is partly because of cost and partly because MRI’s extreme sensitivity comes with a trade-off: a higher rate of false positives. The specificity of breast MRI is lower than mammography, meaning it picks up many findings that turn out not to be cancer. This can lead to unnecessary biopsies and significant anxiety.
What It Costs
A breast MRI is one of the most expensive breast cancer screening methods available. Without insurance, you can expect to pay between $1,000 and $3,000 per scan. With insurance and a documented high-risk status, many plans cover annual breast MRI with a copay ranging from $100 to $500. However, if you don’t meet the specific high-risk criteria, insurance may deny coverage entirely, leaving you with the full bill.
What Results to Expect
Results typically come within a few days to a week. Because MRI is so sensitive, there is a meaningful chance (approximately 8% to 15% per exam) of being called back for additional imaging or biopsy, even when cancer is not present. While this can be stressful, most women who are recommended for breast MRI screening have risk profiles where the benefits of early detection far outweigh the downsides of false positives.
For high-risk women, breast MRI isn’t optional. It’s essential. Combined with mammography, it provides the most comprehensive screening available today.
3. Breast Ultrasound: An Accessible Supplemental Breast Cancer Screening Method
Breast ultrasound uses high-frequency sound waves, the same technology that creates those first grainy images of your baby during pregnancy, to generate pictures of the internal structures of the breast. No radiation involved. No compression. Just a transducer gliding over gel-coated skin while a computer translates the sound echoes into real-time images.
This screening method truly shines as a supplemental tool for women with dense breast tissue. A landmark study called ACRIN 6666 found that adding ultrasound to mammography detected an additional 3.7 cancers per 1,000 women screened in those with dense tissue and at least one other risk factor. That’s 3.7 women per thousand who would have walked out with an undetected cancer if they had relied on mammography alone.
How Breast Ultrasound Works
There are two main types of breast ultrasound. The first is handheld ultrasound (HHUS), where a trained technologist manually moves a transducer across your breast. This exam takes about 15 to 30 minutes and is highly operator-dependent, meaning the quality of results varies significantly based on the skill and experience of the person performing it.
The second type is automated breast ultrasound (ABUS), which uses a large transducer that scans the entire breast in a standardized, reproducible pattern. ABUS produces a 3D volume of images that a radiologist can review later, reducing the variability that comes with handheld scanning. The FDA approved ABUS specifically as a supplemental screening tool for women with dense breast tissue and negative mammograms.
Who Should Consider This Screening Method
- Women with dense breast tissue who have had a normal mammogram
- Women who cannot undergo MRI (due to metallic implants, claustrophobia, kidney issues that prevent contrast dye use, etc.)
- Women who are pregnant and need breast imaging (since ultrasound uses no radiation)
- Younger women under 30 who find a lump, as their breast tissue is typically too dense for effective mammography
- As a diagnostic tool when a mammogram finds something that needs further evaluation
What It Costs
Breast ultrasound is significantly more affordable than MRI, typically ranging from $100 to $500 without insurance. Automated breast ultrasound can cost slightly more, generally $200 to $450. Insurance coverage varies. Some states have passed dense breast notification laws that also mandate insurance coverage for supplemental ultrasound screening, but this is not universal.
The Trade-offs
Ultrasound’s main limitation is a relatively high false-positive rate. For every cancer detected through supplemental ultrasound screening, approximately 5 to 10 women will undergo biopsies that turn out to be benign. Additionally, ultrasound is not great at detecting ductal carcinoma in situ (DCIS), which is an early-stage, non-invasive form of breast cancer that mammography catches well.
That said, ultrasound excels at distinguishing between solid masses (which may need biopsy) and fluid-filled cysts (which are almost always benign). This capability alone saves thousands of women from unnecessary biopsies every year.
4. Contrast-Enhanced Mammography (CEM): The Emerging Breast Cancer Screening Method
This is one of the most exciting developments in breast imaging, and most women have never heard of it. Contrast-enhanced mammography combines the accessibility of mammography with the cancer-highlighting power of contrast dye, similar to what’s used in MRI. The result is an imaging method that approaches MRI-level sensitivity at a fraction of the cost and time.
Here’s how it works in practice: you receive an injection of iodine-based contrast dye through an IV, wait about two minutes for the dye to circulate, and then undergo what is essentially a modified mammogram. The machine captures two images at each position: a standard low-energy image (which looks like a regular mammogram) and a high-energy image. A computer then subtracts the low-energy image from the high-energy one, creating a “recombined” image that highlights areas of abnormal blood flow, exactly the signature of many cancers.
Why CEM Is Generating So Much Excitement
Early research is remarkably promising. Multiple studies have shown CEM sensitivity ranging from 88% to 96%, closely rivaling breast MRI’s detection rates. A 2019 study published in Radiology found that CEM detected significantly more cancers than mammography combined with ultrasound, with comparable accuracy to MRI. And the exam takes about 10 minutes, compared to 30 to 60 minutes for MRI.
For women who need something beyond standard mammography but can’t access, afford, or tolerate breast MRI, CEM may be the breakthrough they’ve been waiting for.
Who Should Consider This Screening Method
- Women at intermediate to high risk for breast cancer
- Women with dense breast tissue seeking a supplemental screening option
- Women who are claustrophobic or can’t undergo MRI for other medical reasons
- Women for whom MRI is cost-prohibitive
- As a problem-solving tool when other imaging results are inconclusive
What It Costs
CEM typically costs between $350 and $800 without insurance, making it substantially less expensive than breast MRI. However, because it’s relatively new as a screening tool, insurance coverage is inconsistent. Some facilities bill it as a diagnostic mammogram with contrast, which may improve insurance reimbursement. As more research accumulates, coverage is expected to expand.
Considerations and Limitations
CEM involves both radiation (comparable to a standard mammogram) and contrast dye. Iodine-based contrast carries a small risk of allergic reaction, and it’s not suitable for women with significant kidney disease or iodine allergies. Breast compression is still required. And because CEM is newer, not all imaging centers offer it yet, so access may be limited depending on where you live.
Despite these considerations, the trajectory of CEM research suggests it may become a standard recommended screening tool for intermediate and high-risk women within the next five to ten years. It’s worth asking your doctor about, especially if you fall into a risk category where standard mammography alone isn’t enough.
5. Molecular Breast Imaging (MBI): The Nuclear Medicine Breast Cancer Screening Method
Molecular breast imaging, also known as breast-specific gamma imaging (BSGI) or scintimammography, takes a fundamentally different approach to finding cancer. Instead of looking at anatomy (the structure of your breast), it looks at physiology (what your breast cells are doing). Cancer cells are metabolically hyperactive, meaning they consume energy at a much higher rate than normal cells. MBI exploits this difference.
Before the exam, a small amount of radioactive tracer (technetium-99m sestamibi) is injected into a vein in your arm. This tracer travels through your bloodstream and is preferentially absorbed by cells that are metabolically active, including cancer cells. Special gamma cameras then detect the radiation emitted by the tracer and create images showing areas of increased uptake.
How MBI Performs Compared to Other Breast Cancer Screening Methods
The results from clinical trials are impressive. A study published by the Mayo Clinic found that MBI detected an additional 7.5 cancers per 1,000 women with dense breast tissue, compared to digital mammography, which detected only 3.2 per 1,000. The sensitivity of MBI for invasive cancer in women with dense breasts ranges from approximately 82% to 91%, which is dramatically better than mammography’s estimated 25% to 50% sensitivity in this population.
MBI also has a notable advantage in terms of specificity. Compared to MRI, MBI produces fewer false positives, meaning fewer unnecessary biopsies. This makes it particularly appealing for women who want enhanced screening without the anxiety and procedural burden of frequent false alarms.
Who Should Consider This Screening Method
- Women with dense breast tissue and a normal mammogram who want supplemental screening
- Women at intermediate risk (15% to 20% lifetime risk) who don’t qualify for MRI screening
- Women who cannot undergo MRI due to implanted devices, claustrophobia, or kidney issues
- Women with breast implants, which can interfere with mammographic and MRI imaging
What It Costs
MBI typically costs between $400 and $800 without insurance. Coverage is still evolving. Some insurers cover it for women with documented dense breast tissue or elevated risk factors, but many do not yet. Medicare coverage for MBI has been expanding, particularly in states with comprehensive dense breast legislation.
The Radiation Question
The elephant in the room with MBI is radiation dose. The original MBI protocols used radiation doses significantly higher than mammography (approximately 6 to 8 times the effective dose). However, newer low-dose MBI protocols have reduced the dose to approximately 2 to 3 times that of a standard mammogram, and research continues to push this lower.
For perspective, the radiation dose from a low-dose MBI exam is roughly equivalent to the background radiation you’d absorb from natural environmental sources over about six to eight months. Most experts consider this an acceptable trade-off for women who would otherwise have cancers missed by mammography alone, but it’s a factor worth discussing with your doctor.
6. Thermography: The Controversial Breast Cancer Screening Method
Thermography, formally known as digital infrared thermal imaging (DITI), is perhaps the most divisive topic in breast cancer screening. It uses a special camera to detect and map heat patterns on the surface of the skin. The theory is that areas of increased blood flow and metabolic activity (hallmarks of cancer growth) generate more heat, and this heat signature can be detected from the skin surface.
Let’s be clear upfront: the FDA has not approved thermography as a standalone screening tool for breast cancer, and every major medical organization, including the American Cancer Society, the American College of Radiology, and the Society of Breast Imaging, states explicitly that thermography should not replace mammography.
What the Evidence Actually Shows
Thermography’s sensitivity for breast cancer detection varies wildly in studies, ranging from approximately 25% to 97%, depending on the study design, equipment used, and interpretation criteria. The most rigorous studies tend to show sensitivity in the 40% to 60% range, which is significantly lower than mammography, breast MRI, and even ultrasound.
The specificity is similarly inconsistent. False-positive rates are high, and the technology has not demonstrated the ability to reliably detect early-stage or small cancers. A 2012 review by the Cochrane Collaboration found insufficient evidence to recommend thermography for breast cancer screening.
Why Some Women Still Choose Thermography
Despite the lack of supporting evidence, thermography has a devoted following. Several factors drive this:
- It involves zero radiation
- It requires no breast compression
- It’s completely non-invasive and painless
- Some practitioners market it as “preventive” because it may theoretically detect physiological changes before a tumor is large enough to appear on other imaging
These are understandable appeals, especially for women who are anxious about radiation exposure or who find mammograms painful. However, choosing thermography instead of mammography is genuinely dangerous because it provides a false sense of security. A normal thermogram does not mean you don’t have cancer.
What It Costs
Thermography scans typically cost $150 to $300 out of pocket. Insurance almost never covers it for screening purposes. Some wellness centers and naturopathic practices offer thermography as part of broader “whole body health” screening packages, which can cost $300 to $500.
The Bottom Line on Thermography
If you’re interested in thermography, approach it as one additional piece of information, never as a replacement for proven breast cancer screening methods. The National Cancer Institute’s page on breast cancer screening provides a comprehensive overview of evidence-based approaches, and thermography is notably absent from their recommended methods. Use it alongside your mammogram and any other appropriate screening, never instead of them. A missed cancer is an unacceptable risk, regardless of how appealing the marketing language around any particular technology might be.
7. Liquid Biopsy (Multi-Cancer Early Detection Blood Tests): The Futuristic Breast Cancer Screening Method
This is where screening technology starts to feel like science fiction, except it’s already available. Liquid biopsies are blood tests that detect fragments of cancer DNA (called circulating tumor DNA, or ctDNA) or other cancer-associated biomarkers circulating in your bloodstream. The most prominent example is Galleri, developed by GRAIL, which is a multi-cancer early detection test that can screen for over 50 types of cancer, including breast cancer, from a single blood draw.
The concept is breathtaking in its simplicity. Cancer cells shed DNA into the bloodstream, even in very early stages. By analyzing the methylation patterns on this DNA, sophisticated algorithms can not only detect the presence of cancer but also predict where in the body it originated. No imaging. No radiation. No compression. Just a tube of blood.
How Liquid Biopsies Perform as Breast Cancer Screening Methods
Let’s temper the excitement with reality. The Galleri test, while groundbreaking, is not yet sensitive enough to replace mammography for breast cancer specifically. In clinical trials (the PATHFINDER study), Galleri’s overall cancer detection rate was strongest for cancers that currently lack screening methods, like pancreatic, liver, and ovarian cancers.
For breast cancer specifically, liquid biopsy sensitivity for early-stage disease (Stage 1) is estimated at roughly 16% to 40%, depending on the study. This improves significantly for later-stage disease (Stage 3 and 4 sensitivity reaches 75% to 90%), but the whole point of screening is to find cancer early, when it’s most treatable. So while liquid biopsy adds a valuable layer of protection, it is not a replacement for imaging-based screening.
The positive predictive value is also worth noting. When Galleri says cancer is detected, it is correct approximately 43% to 44% of the time. This means that roughly half of positive results turn out to be false positives after diagnostic workup. This is being addressed through ongoing research and algorithm refinement.
Who Should Consider This Screening Method
- Adults over 50 who want a supplemental layer of cancer screening beyond organ-specific tests
- Individuals with a strong family history of multiple cancer types
- Those with elevated anxiety about cancer who want maximum screening coverage
- Anyone interested in screening for cancers that have no current standard screening tests (like ovarian or pancreatic cancer)
It’s important to note that as of 2024, no medical society recommends liquid biopsy as a replacement for any existing cancer screening test. It is intended as a supplemental, or “additive,” screening tool.
What It Costs
The Galleri test costs approximately $949 and is not covered by insurance. It’s available by prescription only, meaning you’ll need a healthcare provider to order it. Some concierge medicine practices and direct-to-consumer health platforms include it in premium screening packages. Newer competitors entering the liquid biopsy market may drive prices down over time.
The Bigger Picture
Liquid biopsy represents the future of cancer screening, and that future is arriving faster than most people realize. As sensitivity improves through larger training datasets and refined algorithms, these tests will likely become standard components of annual physicals within the next decade. For now, consider them a promising addition to your screening strategy, not a cornerstone.
8. Breast-Specific PET Scanning (Positron Emission Mammography): The High-Resolution Breast Cancer Screening Method
Most people have heard of PET scans in the context of cancer staging, those full-body scans that light up areas of high metabolic activity. Positron emission mammography (PEM) takes the same nuclear medicine principle and applies it specifically to the breast, with much higher resolution than a standard whole-body PET scan.
Like MBI, PEM involves injecting a radioactive tracer, in this case fluorodeoxyglucose (FDG), which is a form of sugar. Cancer cells are sugar-hungry. They consume glucose at dramatically higher rates than normal cells (a phenomenon known as the Warburg effect). When the FDG accumulates in cancer cells, it emits positrons that the PEM scanner detects, creating a metabolic map of your breast.
How PEM Compares to Other Breast Cancer Screening Methods
PEM offers remarkable spatial resolution, detecting lesions as small as 1.5 to 2 millimeters in some studies. Its sensitivity for invasive breast cancer ranges from approximately 90% to 95%, putting it in the same tier as breast MRI. Importantly, PEM has demonstrated better specificity than MRI in several comparative studies, meaning fewer false positives and fewer unnecessary biopsies.
A study published in the American Journal of Roentgenology found that PEM detected additional cancers missed by both mammography and MRI, particularly in women with dense breast tissue or multifocal disease (cancer in multiple locations within the breast).
Who Should Consider This Screening Method
- Women with known breast cancer, for evaluating the extent of disease before surgery
- Women at high risk where MRI has produced inconclusive results
- Women with breast implants that limit mammographic or MRI assessment
- Women who need a problem-solving tool when other imaging is contradictory
PEM is primarily used as a diagnostic tool rather than a routine screening tool. Its use in average-risk screening is limited by radiation dose, cost, and availability.
What It Costs
PEM is one of the more expensive breast cancer screening methods, typically ranging from $800 to $1,500 without insurance. Insurance coverage is more likely when PEM is used for diagnostic purposes (evaluating a known abnormality) rather than screening. Coverage as a screening tool is rare.
Radiation Considerations
PEM involves a higher radiation dose than mammography or low-dose MBI, roughly equivalent to a whole-body PET/CT scan. This limits its appropriateness for routine annual screening but makes it a powerful tool for specific clinical scenarios where the diagnostic benefit justifies the exposure.
9. Genetic Testing and Risk Assessment: The Predictive Breast Cancer Screening Method
The ninth “screening method” in our comparison isn’t an imaging test at all. It’s knowledge about your own DNA. Genetic testing for breast cancer susceptibility, particularly for BRCA1, BRCA2, and other high-risk gene mutations (PALB2, ATM, CHEK2, TP53, and others), fundamentally changes your screening strategy. It doesn’t detect cancer that already exists. It tells you how likely you are to develop it, which allows you to screen more aggressively, consider preventive interventions, and make informed decisions about your healthcare timeline.
Mutations in the BRCA1 gene carry a 55% to 72% lifetime risk of developing breast cancer. BRCA2 mutations carry a 45% to 69% lifetime risk. Compare this to the general population risk of approximately 13%, and you can see why knowing your genetic status is so powerful.
How Genetic Testing Works
Modern genetic testing for breast cancer is remarkably simple from the patient’s perspective. You provide either a blood sample or a saliva sample. The lab analyzes your DNA for mutations in the relevant genes. Results typically come back in two to four weeks. A genetic counselor (either before or after testing) helps you understand what the results mean and how they should influence your screening and prevention plan.
Panels now available test for mutations in 10 to 80+ genes simultaneously, providing a comprehensive risk picture that goes far beyond BRCA1 and BRCA2. These multi-gene panels can reveal intermediate-risk mutations that might still warrant enhanced screening but wouldn’t qualify you for the most aggressive interventions.
Who Should Consider Genetic Testing
The National Comprehensive Cancer Network (NCCN) recommends genetic testing for individuals who meet specific criteria, including:
- A personal history of breast cancer diagnosed at age 50 or younger
- Triple-negative breast cancer diagnosed at age 60 or younger
- Two or more primary breast cancers in the same individual
- A known family member with a pathogenic variant in a cancer susceptibility gene
- Ashkenazi Jewish heritage with any personal or family history of breast or ovarian cancer
- A family history pattern suggestive of hereditary cancer (multiple affected relatives, young ages of onset, associated cancers like ovarian, pancreatic, or prostate)
- Male breast cancer in the family
What It Costs
The cost of genetic testing has dropped dramatically over the past decade. A comprehensive multi-gene panel now costs approximately $250 to $4,000, with most falling in the $300 to $600 range for self-pay patients. Many insurance plans cover genetic testing when specific criteria are met, often with out-of-pocket costs below $100. Some testing companies offer financial assistance programs or cap patient costs regardless of insurance status.
If you factor in genetic counseling (pre-test and post-test), the total cost might range from $400 to $5,000, depending on your location and insurance coverage. Many cancer centers offer genetic counseling at no additional charge as part of their high-risk screening programs.
What the Results Mean for Your Screening Strategy
This is where genetic testing truly transforms your healthcare. A positive result for a high-risk mutation doesn’t just mean “you’re at higher risk.” It activates a completely different screening protocol:
- Annual mammography starting at age 25 to 30, instead of 40 to 50
- Annual breast MRI alternating with mammography every six months (so you’re being screened every six months by alternating modalities)
- Clinical breast exams every 6 to 12 months
- Discussion of risk-reducing medications (tamoxifen, raloxifene, aromatase inhibitors)
- Discussion of risk-reducing surgery (prophylactic mastectomy, which reduces breast cancer risk by 90% to 95%)
- Screening for associated cancers (ovarian, pancreatic, melanoma, depending on the gene involved)
A negative result in someone with a strong family history isn’t necessarily all-clear. It may simply mean the responsible mutation hasn’t been identified yet, or that the cancer risk in the family is driven by multiple lower-risk genetic variants or environmental factors.
Genetic testing doesn’t show you a tumor. It shows you your future risk profile. And that foresight is, for many women, the most valuable screening tool of all.
The Complete Breast Cancer Screening Methods Comparison: Cost, Sensitivity, and Suitability at a Glance
Here’s the table you’ve been waiting for. This comparison puts all nine breast cancer screening methods side by side so you can evaluate them based on the factors that matter most to your individual situation.
| Screening Method | Approx. Cost (No Insurance) | Sensitivity for Breast Cancer | Radiation Involved | Best For | Limitations |
|---|---|---|---|---|---|
| 3D Mammography (Tomosynthesis) | $250 – $450 | 65% – 85% (overall); better in dense tissue than 2D | Low (X-ray) | All women 40+; dense breast supplemental upgrade | Still limited in very dense tissue; compression required |
| Breast MRI | $1,000 – $3,000 | 94% – 100% (high-risk populations) | None (uses magnets/radio waves) | High-risk women (BRCA+, >20% lifetime risk) | High false-positive rate; expensive; contrast dye required; claustrophobia |
| Breast Ultrasound | $100 – $500 | 70% – 83% (supplemental in dense tissue) | None (sound waves) | Dense breast supplemental screening; pregnant women; MRI-ineligible patients | Operator-dependent (handheld); high false-positive rate; poor DCIS detection |
| Contrast-Enhanced Mammography (CEM) | $350 – $800 | 88% – 96% | Low (X-ray) | Intermediate/high-risk women; MRI alternative | Contrast dye allergy risk; newer technology; limited availability |
| Molecular Breast Imaging (MBI) | $400 – $800 | 82% – 91% (dense tissue) | Moderate (radiotracer) | Dense breast supplemental screening; MRI-ineligible patients | Higher radiation than mammography; not widely available |
| Thermography | $150 – $300 | 25% – 60% (variable) | None | Adjunct only (NOT a replacement for any proven method) | Not FDA-approved as standalone screening; unreliable; high variability; false reassurance risk |
| Liquid Biopsy (Galleri/MCED) | $949 | 16% – 40% (early-stage breast cancer) | None | Supplemental multi-cancer screening; cancers without standard tests | Low sensitivity for early breast cancer; not a replacement for imaging; not covered by insurance |
| Positron Emission Mammography (PEM) | $800 – $1,500 | 90% – 95% | Moderate-High (radiotracer) | Diagnostic use; extent-of-disease evaluation; complex cases | Not suitable for routine screening; radiation dose; expensive; limited availability |
| Genetic Testing + Risk Assessment | $250 – $4,000 (testing); up to $5,000 (with counseling) | N/A (predicts risk, not current cancer) | None | Family history of breast/ovarian cancer; Ashkenazi Jewish heritage; early-onset cancers | Doesn’t detect existing cancer; psychological impact of results; may not explain all familial risk |
Total estimated cost for all nine methods (without insurance): approximately $4,250 to $11,800+
Most common comprehensive high-risk panel (3D Mammo + MRI + Genetic Testing): approximately $1,550 to $7,450
The $7,800 figure referenced in our headline represents the approximate midpoint cost of pursuing comprehensive screening across multiple modalities in a single year for a high-risk woman. This includes 3D mammography, breast MRI, supplemental ultrasound, genetic testing with counseling, and a multi-cancer early detection blood test.
How to Choose the Right Breast Cancer Screening Methods for Your Risk Level
Navigating nine different screening technologies can feel overwhelming, but the decision framework is actually more straightforward than it appears. Your screening strategy should be built on three pillars: your age, your breast density, and your personal risk profile.
Average Risk Women (Lifetime Risk Below 15%)
If you have no significant family history of breast cancer, no known genetic mutations, no prior chest radiation, and no personal history of breast cancer or high-risk breast lesions, you are considered average risk.
Recommended screening:
- Annual or biennial 3D mammography starting at age 40 (some guidelines say 50, but the trend is moving toward 40 as the starting age)
- Clinical breast exam as part of your annual well-woman visit
- Breast self-awareness (knowing what’s normal for you so you can identify changes)
For average-risk women, mammography remains the cornerstone. Adding supplemental screening methods is generally not recommended unless you have dense breast tissue.
Intermediate Risk Women (Lifetime Risk 15% to 20%)
You might fall into this category if you have one or two risk factors, such as dense breast tissue, a first-degree relative with breast cancer, a history of certain benign breast conditions (atypical ductal hyperplasia, lobular carcinoma in situ), or older age at first pregnancy.
Recommended screening:
- Annual 3D mammography
- Supplemental breast ultrasound or contrast-enhanced mammography, especially if you have dense breast tissue
- Consider genetic testing if family history meets criteria
- Discuss molecular breast imaging with your doctor as an alternative supplemental option
High Risk Women (Lifetime Risk Above 20%)
This group includes women with known BRCA mutations, strong family histories, prior chest radiation, and certain genetic syndromes.
Recommended screening:
- Annual 3D mammography starting at age 25 to 30
- Annual breast MRI alternating with mammography (so you’re screened every 6 months)
- Clinical breast exam every 6 to 12 months
- Genetic counseling and testing if not already completed
- Consider liquid biopsy as supplemental screening
- Discuss risk-reducing strategies with your oncology team
Understanding Breast Density: The Factor That Changes Everything About Breast Cancer Screening Methods
We’ve mentioned breast density repeatedly throughout this article, and for good reason. It is the single most important variable that determines whether mammography alone is sufficient for you.
Breast density is categorized on a four-point scale:
- A: Almost entirely fatty (about 10% of women). Mammography works extremely well.
- B: Scattered areas of fibroglandular density (about 40% of women). Mammography works well.
- C: Heterogeneously dense (about 40% of women). Mammography starts to struggle.
- D: Extremely dense (about 10% of women). Mammography misses a significant proportion of cancers.
If you’re in category C or D, you have dense breast tissue, and you need to know about it. Here’s why dense tissue is a double problem:
- It masks cancer on mammograms. Both dense tissue and tumors appear white on the image, making tumors harder to spot.
- It independently increases your risk of developing breast cancer. Women with extremely dense tissue (category D) have a 4 to 6 times higher risk of breast cancer compared to women with almost entirely fatty breasts.
In September 2024, a new FDA rule went into effect requiring all mammography facilities in the United States to notify patients of their breast density. This is a major step forward. Previously, many women had no idea whether their breasts were dense, even though this information was sitting in their radiology reports.
If you learn that you have dense breast tissue, the single most important thing you can do is talk to your doctor about supplemental screening. This might mean breast ultrasound, contrast-enhanced mammography, molecular breast imaging, or breast MRI, depending on your overall risk profile.
The Economics of Early Detection: Why Spending Now Saves Everything Later
Let’s talk money, because the cost of breast cancer screening methods pales in comparison to the cost of treating advanced breast cancer.
The average cost of treating Stage 1 breast cancer in the United States is approximately $60,000 to $80,000. Treatment for Stage 4 metastatic breast cancer averages $250,000 to $500,000 or more, and these costs can extend over years of ongoing treatment. Beyond the financial devastation, late-stage treatment involves chemotherapy, radiation, multiple surgeries, hormone therapy, targeted therapy, immunotherapy, and their cumulative physical and emotional toll.
Even the most comprehensive annual screening protocol we’ve discussed in this article, totaling roughly $7,800 per year for a high-risk woman, represents a fraction of the cost of treating a cancer that was found late.
For average-risk women, annual 3D mammography (often covered by insurance with no out-of-pocket cost) is an investment of essentially zero dollars for a test that could save your life. There is no rational argument against it.
And for women who face barriers to accessing screening, whether financial, geographic, or systemic, organizations like Susan G. Komen, the National Breast and Cervical Cancer Early Detection Program (NBCCEDP), and local community health centers offer free or low-cost mammograms. If cost is preventing you from getting screened, these resources exist for you.
What’s Coming Next: The Future of Breast Cancer Screening Methods
The landscape of breast cancer screening is evolving rapidly. Several emerging technologies deserve attention because they may fundamentally change how we detect breast cancer within the next decade.
Artificial Intelligence in Mammography
AI algorithms are being trained to read mammograms with accuracy that matches or exceeds human radiologists. In a 2023 study published in Lancet Oncology, an AI system detected 20% more cancers than human radiologists while simultaneously reducing false positives. AI doesn’t replace human radiologists. Rather, it serves as a “second reader,” flagging potential abnormalities for human review. Several AI-assisted mammography platforms have received FDA clearance, and their integration into clinical practice is accelerating.
Abbreviated MRI Protocols
One of the biggest barriers to widespread breast MRI screening is time. A standard breast MRI takes 30 to 60 minutes. Abbreviated protocols (sometimes called “fast MRI” or “AB-MRI”) compress this to 10 minutes or less by focusing on the most diagnostically relevant sequences. Studies show that abbreviated MRI detects cancers at rates comparable to full MRI protocols while being faster and cheaper. If abbreviated MRI can be delivered at $300 to $500 instead of $1,000 to $3,000, it could become accessible to far more women.
Blood-Based Biomarker Panels
Beyond ctDNA (the basis for Galleri), researchers are exploring protein biomarkers, exosomes, microRNA, and circulating tumor cells as additional blood-based detection methods. The combination of multiple biomarker types in a single test may dramatically improve the sensitivity of liquid biopsy for early-stage breast cancer specifically.
Photoacoustic Imaging
This emerging technology combines laser light with ultrasound to create images based on how tissues absorb light. Hemoglobin in blood absorbs light differently than other tissues, and tumors with their abundant blood supply produce distinctive photoacoustic signatures. This technology is still primarily in the research phase, but early results are promising for non-invasive, radiation-free breast cancer detection.
The future of screening is a multi-layered, personalized approach where your risk profile, your breast density, your genetics, and your preferences determine a customized screening protocol. We’re not there yet, but we’re closer than most people realize.
Common Myths and Misconceptions About Breast Cancer Screening Methods
Let’s clear up some persistent myths that prevent women from making fully informed decisions about their screening.
Myth 1: “I Don’t Need Screening Because No One in My Family Has Had Breast Cancer”
Approximately 75% to 85% of women diagnosed with breast cancer have no family history of the disease. Family history is an important risk factor, but its absence does not make you safe. Every woman with breast tissue has some risk, and screening is essential regardless of your family tree.
Myth 2: “Mammograms Cause Cancer Because of the Radiation”
The radiation dose from a standard mammogram is extremely low, approximately 0.4 millisieverts (mSv), which is roughly equivalent to seven weeks of natural background radiation. The lifetime risk of developing cancer from annual mammograms starting at age 40 is estimated at 1 to 2 additional cancers per 100,000 women. Compare this to the approximately 12,500 breast cancers per 100,000 women that would be detected (and made treatable) by that same screening. The math is overwhelmingly in favor of screening.
Myth 3: “I Found a Lump, But It Doesn’t Hurt, So It’s Probably Fine”
The vast majority of breast cancers are painless. Pain is not a reliable indicator of malignancy. If you find any new lump, thickening, or change in your breast, get it evaluated promptly, regardless of whether it hurts.
Myth 4: “I’m Too Young to Worry About Breast Cancer”
While breast cancer is more common after age 50, approximately 9% of new cases occur in women under 45. For women with genetic mutations like BRCA1, the risk begins rising significantly in the late 20s and 30s. Young women should practice breast self-awareness and report any changes to their healthcare provider.
Myth 5: “Thermography or Liquid Biopsy Can Replace My Mammogram”
Neither thermography nor liquid biopsy has the sensitivity or clinical validation to serve as a replacement for mammography. Using them as substitutes puts you at genuine risk of a missed or delayed diagnosis. They may have a role as supplemental tools, but the mammogram remains the foundation.
Creating Your Personal Breast Cancer Screening Plan
Here’s a practical framework for building your own screening strategy using the breast cancer screening methods we’ve discussed. Print this section, bring it to your next appointment, and have a conversation with your doctor.
Step 1: Know Your Risk
Calculate your lifetime breast cancer risk using a validated tool. The most commonly used models include:
- Tyrer-Cuzick (IBIS) model: Incorporates family history, hormonal factors, and breast density. Considered the most comprehensive.
- Gail model: Uses personal risk factors and limited family history. Available at many screening centers and online.
Ask your doctor to run one of these assessments. The number you get determines your risk category and guides your screening intensity.
Step 2: Know Your Breast Density
After your next mammogram, ask for your density category (A, B, C, or D). If you’re category C or D, you should be discussing supplemental screening with your doctor. Under the new FDA rule, your mammography facility is required to tell you.
Step 3: Know Your Genetic Risk
If your family history meets any of the criteria listed in the genetic testing section above, pursue genetic counseling and testing. This single step could transform your screening timeline and potentially save your life.
Step 4: Build Your Annual Screening Calendar
Based on your risk level, construct a screening schedule:
Average risk:
- Mammogram (ideally 3D) annually or biennially starting at 40
- Clinical breast exam annually
Intermediate risk:
- 3D mammogram annually starting at 40
- Supplemental ultrasound or CEM annually (if dense breasts)
- Clinical breast exam annually
High risk:
- 3D mammogram annually starting at 25 to 30
- Breast MRI annually (alternating with mammography every 6 months)
- Clinical breast exam every 6 months
- Genetic counseling
- Discussion of risk-reducing interventions
Step 5: Stay Informed
Screening guidelines evolve. New technologies emerge. Your risk factors can change over time. Make breast cancer screening a standing agenda item at every annual visit with your healthcare provider.
What to Do If a Screening Test Finds Something Abnormal
Getting called back after a screening test is terrifying. But here’s the reassuring reality: approximately 90% to 95% of abnormal screening findings turn out not to be cancer. An abnormal result usually just means something needs a closer look.
Here’s the typical sequence if something is found:
- Diagnostic imaging: Additional mammographic views, ultrasound, or MRI of the specific area of concern
- Biopsy recommendation: If diagnostic imaging remains concerning, a tissue sample is obtained. Most biopsies are performed using minimally invasive techniques (core needle biopsy) under image guidance with local anesthesia. The procedure takes 15 to 30 minutes and most women return to normal activities the next day.
- Pathology results: A pathologist examines the tissue sample under a microscope. Results usually take 3 to 7 business days.
- Next steps: Based on pathology, you’ll either be reassured (benign finding), monitored more closely (certain high-risk benign conditions), or referred to an oncology team (cancer diagnosis).
If you are diagnosed with cancer after screening, the prognosis for screen-detected cancers is substantially better than for cancers found by symptoms alone. Screen-detected breast cancers are smaller, more often node-negative (haven’t spread to lymph nodes), and more likely to be treated successfully with less aggressive therapy. According to the American Cancer Society’s breast cancer survival statistics, the overall five-year relative survival rate for localized breast cancer (confined to the breast) is 99%.
That number exists because of screening. Because of women who showed up, who got tested, who caught it early.
The Emotional Side of Breast Cancer Screening That Nobody Talks About
We’ve covered the science, the costs, the technologies, and the decision frameworks. But there’s another dimension to breast cancer screening that deserves honest acknowledgment: it’s emotionally taxing.
The anxiety of waiting for results. The fear triggered by a callback letter. The discomfort of compression. The vulnerability of lying in a cold room with your chest exposed. The weight of knowing your risk score. The grief that comes with a genetic result you didn’t want. The survivor’s guilt when your test is clear but your sister’s wasn’t.
All of this is real, and all of it is valid.
Here’s what I want you to know: feeling anxious about screening does not make you weak. It makes you human. And choosing to screen despite that anxiety makes you brave. Not in the “inspirational quote on a coffee mug” kind of way, but in the real, difficult, show-up-even-when-you’re-scared kind of way.
If screening anxiety is preventing you from getting tested, talk to your provider about it. Many imaging centers now offer comfort measures, including warm gowns, guided relaxation, shorter appointment times, and compassionate technologists who understand what you’re going through. Some women bring a friend. Some use headphones with a favorite playlist. Some schedule their appointment at a time when they can take the rest of the day to decompress afterward.
Whatever you need to make it possible, it’s worth it. Because the discomfort of a screening test is temporary. The consequences of a missed cancer are not.
A Note for Women of Color: Disparities in Breast Cancer Screening and Outcomes
No honest discussion of breast cancer screening methods would be complete without addressing the stark disparities that exist along racial and ethnic lines.
Black women in the United States are 40% more likely to die from breast cancer than white women, despite having similar or slightly lower incidence rates. This disparity is driven by multiple intersecting factors:
- Later stage at diagnosis: Black women are more likely to be diagnosed at a later stage, partly due to lower rates of regular screening and longer intervals between screening and diagnostic follow-up.
- More aggressive tumor biology: Black women have higher rates of triple-negative breast cancer, an aggressive subtype with fewer treatment options.
- Systemic barriers: Unequal access to quality healthcare, insurance coverage gaps, bias in medical settings, and geographic barriers to screening facilities all contribute.
- Dense breast tissue prevalence: Studies suggest that Black women may have higher rates of dense breast tissue, which can reduce mammographic sensitivity if supplemental screening is not offered.
If you are a Black woman, a Latina woman, an Indigenous woman, or a woman from any community that has historically been underserved by the healthcare system, your screening is not less important. It is more important. Advocate for yourself. Ask about your breast density. Ask about supplemental screening. Ask about genetic testing if your family history warrants it. And if your provider dismisses your concerns, find a new provider.
Health equity in breast cancer screening isn’t just a policy issue. It’s a survival issue.
Wrapping It Up: Your Breasts, Your Life, Your Choice
Here’s the thing about breast cancer screening methods: there is no single perfect test. Every technology we’ve discussed has strengths and limitations, costs and trade-offs. Mammography misses some cancers. MRI finds things that aren’t cancer. Ultrasound depends on the operator. Genetic testing tells you about risk, not reality. Liquid biopsy isn’t sensitive enough yet. Thermography doesn’t have the evidence to stand on its own.
But together? Together, these tools create a net that catches what any single test alone would miss.
The right combination for you depends on who you are. Your age, your density, your genes, your history, your risk tolerance, your budget, and your values all play a role. There is no one-size-fits-all answer, and anyone who tells you otherwise is oversimplifying a complex decision.
What is universal, though, is this: doing nothing is the worst option. Every day that a cancer goes undetected, it grows. It evolves. It develops the ability to spread. And once it spreads, the mathematics of survival change dramatically.
Screening saves lives. Not in the abstract, hand-wavy, public-health-campaign sense. In the literal, you-are-alive-today-because-you-got-that-test sense. In the your-kids-still-have-their-mom sense. In the you-got-to-see-60-and-70-and-80 sense.
So schedule the mammogram. Ask about your breast density. Look into your family history. Have the genetic testing conversation. Explore supplemental screening if it’s right for you. Don’t let the perfect be the enemy of the good. Get screened. Get screened again. Keep getting screened.
Your life is worth every minute of discomfort, every dollar of cost, every moment of anxiety.
Because early detection doesn’t just save lives. It saves your life.
Share this article with a woman you love. Your sister, your mother, your best friend, your daughter. Forward it, text it, post it. The information in this article could be the reason someone catches cancer early enough to beat it. That’s not an exaggeration. That’s the reality of what early detection can do.
Drop a comment below: Which of these breast cancer screening methods were you not aware of before reading this? We’d love to hear from you.