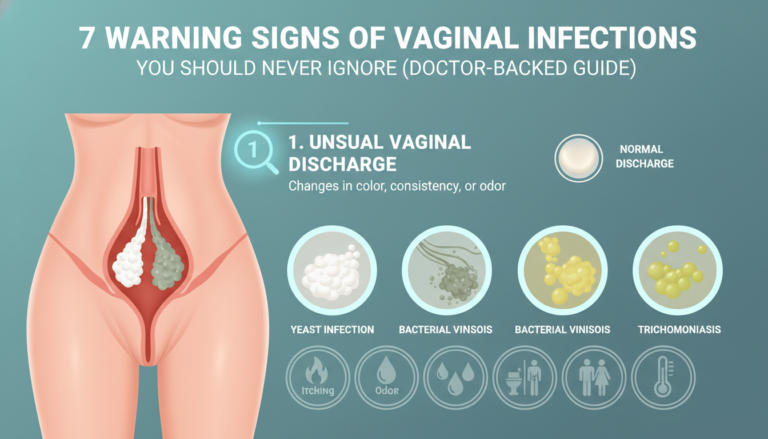
7 Warning Signs of Vaginal Infections You Should Never Ignore (Doctor-Backed Guide)
The 3am Realisation
You’ve been ignoring it for three weeks now. That slight itch that comes and goes. The discharge that’s not quite the same colour or consistency as usual. You’ve convinced yourself it’s nothing, that it’ll sort itself out, that you’re probably just being paranoid.
Then last night, during intimacy with your partner, you felt a sharp burning sensation that made you wince. You excused yourself, citing tiredness. But now, at 3am, you’re awake, scrolling through Google, terrified you’ve left something serious untreated. You’re wondering if that persistent odour you’ve been masking with extra showers means something’s genuinely wrong. The search results range from “perfectly normal” to genuinely frightening, and you’re more confused than when you started.
You’re not overreacting. You’re also not alone in this uncertainty.
The challenge with vaginal infections is that they rarely announce themselves with obvious, textbook symptoms. They creep in gradually, mimicking normal fluctuations in discharge and sensation that happen throughout your cycle. By the time you’re certain something’s wrong, the infection may have been present for weeks or even months, potentially affecting your fertility, sexual comfort, and overall wellbeing.
Understanding Vaginal Infections: The Clinical Foundation
A vaginal infection occurs when the delicate ecosystem of bacteria, yeast, and other microorganisms in your vagina becomes imbalanced. Think of your vaginal microbiome as a carefully tended garden. When it’s healthy, beneficial bacteria (primarily Lactobacillus species) keep everything in check, maintaining an acidic pH that prevents harmful organisms from taking over.
When this balance shifts, one of three common scenarios typically unfolds: bacterial vaginosis (BV), where harmful bacteria outnumber the beneficial ones; vulvovaginal candidiasis (a yeast infection), where Candida fungus overgrows; or trichomoniasis, a sexually transmitted infection caused by a parasite.
Featured Snippet Answer:
Vaginal infection warning signs include unusual discharge changes in colour, consistency, or smell; persistent itching or burning that doesn’t resolve within a few days; pain during intercourse or urination; unexpected bleeding between periods; and vulval redness or swelling. Any combination of these symptoms lasting more than 48 hours warrants medical assessment.
The reason vaginal infections remain so misunderstood in mainstream medicine comes down to one persistent myth: that all vaginal discharge or odour is inherently “dirty” or shameful. This cultural baggage means women often delay seeking care until symptoms become unbearable, and even then, they may receive dismissive advice about “better hygiene” rather than proper diagnosis and treatment.
Your vagina is self-cleaning. It’s supposed to produce discharge. The question isn’t whether discharge exists, but whether what you’re experiencing represents a significant change from your personal baseline.
Understanding what’s normal for you specifically is the foundation of recognising when something’s genuinely wrong. Your discharge will naturally vary throughout your menstrual cycle. Around ovulation, it becomes clear and stretchy, resembling raw egg white. After ovulation, it typically becomes thicker and white or cream-coloured. Light vaginal odour is also normal, often described as slightly musky or tangy, not unpleasant.
The warning signs we’re about to explore represent departures from this healthy baseline. They’re your body’s way of flagging that the vaginal ecosystem has shifted into territory that requires attention.
The 7 Warning Signs of Vaginal Infections
1. Discharge That Resembles Cottage Cheese or Has a Grey Tinge
Texture and colour changes in discharge are often the first visible sign of infection, yet they’re frequently dismissed as “just normal variation.”

Thick, white, clumpy discharge that looks like cottage cheese almost always indicates a yeast infection. This happens because Candida overgrowth produces a characteristic curd-like secretion as the fungus multiplies. You’ll typically notice this alongside intense itching, particularly at night when you’re trying to sleep.
Thin, grey, or greyish-white discharge with a consistency like watered-down milk suggests bacterial vaginosis. BV occurs when the Lactobacillus population drops and opportunistic bacteria like Gardnerella vaginalis take over. Unlike yeast infections, BV discharge is typically not accompanied by significant itching, but it almost always comes with a distinct odour.
Yellow or green discharge, especially if it’s frothy or bubbly, points toward trichomoniasis. This sexually transmitted infection produces a characteristic yellow-green discharge because the Trichomonas parasite triggers an inflammatory response that includes increased white blood cells in vaginal secretions.
2. A Fishy Odour That Intensifies After Intercourse
Vaginal odour is one of the most anxiety-inducing symptoms women experience, largely because we’ve been socialised to believe any odour is problematic. That’s simply not true. But certain odours do signal infection.
A strong fishy smell, particularly one that becomes noticeably worse after sexual intercourse or during your period, is the hallmark sign of bacterial vaginosis. This happens because semen and menstrual blood are both alkaline, and when they mix with the already-disrupted vaginal pH in BV, they trigger the release of volatile amines, the compounds responsible for that distinctive fishy odour.
The smell can be so pronounced that you notice it through your clothing, or your partner mentions it. This isn’t about poor hygiene. It’s a chemical reaction caused by bacterial imbalance, and no amount of washing will resolve it. In fact, excessive washing and douching can worsen bacterial vaginosis by further disrupting the vaginal pH.
If you’re experiencing this symptom, you need antibiotics (typically metronidazole or clindamycin) to restore bacterial balance, not more aggressive cleaning routines.
3. Persistent Itching That Worsens at Night
Vaginal or vulval itching is incredibly common, but when it persists for more than 48 hours or intensifies at night, it’s a red flag for infection.
Yeast infections cause intense itching because Candida produces enzymes and toxins that irritate the vaginal tissue. The itching often feels worse at night because when you’re lying still, you’re more aware of the sensation, and the warmth of bed covers can intensify it.
The itching from a yeast infection is typically concentrated around the vaginal opening and the vulva (the external genital area). You might notice the skin looks red, inflamed, or even develops small cracks or fissures if you’ve been scratching.
Bacterial vaginosis rarely causes significant itching, which is one way to distinguish it from a yeast infection. Trichomoniasis can cause itching, but it’s usually accompanied by other symptoms like the yellow-green discharge mentioned earlier and discomfort during urination.
If you’re reaching for antihistamines or applying nappy rash cream to stop the itch, you’re likely dealing with a yeast infection that needs antifungal treatment, not symptom management.
4. Pain or Burning During Urination
A burning sensation when you urinate can signal either a urinary tract infection (UTI) or a vaginal infection. The distinction matters because the treatments are entirely different.
With a vaginal infection, particularly trichomoniasis or a severe yeast infection, the burning happens because inflamed vaginal tissue comes into contact with acidic urine as it passes. You might also notice the burning is more external, affecting the vulval area, rather than feeling deep inside the urethra (the tube that carries urine from your bladder).
UTIs, by contrast, cause burning that feels internal, often accompanied by an urgent need to urinate frequently and a sensation that your bladder isn’t fully empty.
If you’re experiencing burning during urination along with unusual discharge or vaginal odour, you’re likely dealing with a vaginal infection rather than a UTI. That said, it’s entirely possible to have both simultaneously, particularly if you’ve had a vaginal infection for some time, as the altered pH can make you more susceptible to UTIs.
This symptom should never be ignored beyond 24 to 48 hours. Untreated infections can ascend into the upper reproductive tract, potentially causing pelvic inflammatory disease (PID), which can affect fertility.
5. Discomfort or Pain During Intercourse
Pain during sex, medically termed dyspareunia, has many possible causes, but when it appears suddenly or alongside other symptoms, vaginal infection is a likely culprit.
Yeast infections cause pain during intercourse because the inflamed, irritated vaginal tissue is sensitive to friction and pressure. The pain is often described as burning or stinging, particularly at the vaginal entrance.
Bacterial vaginosis can cause discomfort during sex, though it’s typically less intense than with yeast infections. The pain often feels more like general sensitivity or rawness rather than acute burning.
Trichomoniasis frequently causes painful intercourse because the infection triggers significant inflammation of the vaginal walls. Some women also experience spotting after intercourse with trichomoniasis, as the inflamed tissue is more prone to minor trauma.
If you’ve started avoiding intimacy because of pain, or you’re experiencing a burning sensation that lasts for hours after intercourse, this isn’t something to push through or attribute to inadequate lubrication. Infection-related pain during sex is your body telling you something needs medical attention.
6. Vulval Swelling or Redness
Visible changes to the vulva, the external part of your genitals, are often overlooked because many women don’t regularly examine this area.
Yeast infections commonly cause the vulva to appear red, swollen, and inflamed. You might notice the labia (the “lips” around the vaginal opening) look puffy or feel tender to touch. In severe cases, the skin can crack or develop small cuts, particularly in the creases where the labia meet the thighs.
Trichomoniasis can also cause vulval inflammation, often with a more pronounced red, angry appearance. You might notice tiny red spots on the vaginal walls or cervix, though you wouldn’t be able to see the cervical changes without examination.
Bacterial vaginosis rarely causes significant external changes, which is one way to distinguish it from other infections.
If you’re noticing swelling, redness, or skin changes in the vulval area, particularly alongside other symptoms like unusual discharge or odour, you’re looking at an active infection that needs treatment. Don’t assume this will resolve on its own.
7. Abnormal Bleeding or Spotting Between Periods
Unexpected bleeding or spotting between periods, particularly after intercourse, can indicate several conditions, but when it occurs alongside other vaginal infection symptoms, it shouldn’t be dismissed.
Trichomoniasis is particularly associated with irregular bleeding because the infection causes significant inflammation of the vaginal walls and cervix. This inflamed tissue is more fragile and prone to bleeding, especially during intercourse or after a cervical examination.
Severe bacterial vaginosis can occasionally cause light spotting, though this is less common than with trichomoniasis.
Cervicitis, an inflammation of the cervix often caused by sexually transmitted infections like chlamydia or gonorrhoea, also produces abnormal bleeding alongside unusual discharge.
The presence of abnormal bleeding requires prompt medical assessment because while it may be related to infection, it can also signal other conditions including cervical cell changes, polyps, or in rare cases, more serious pathology. Any woman experiencing persistent irregular bleeding should book an appointment with a gynaecologist within two weeks for proper examination and testing.
What I’ve Seen in Clinical Practice
In my 19 years of clinical practice, what I’ve seen most often is women who’ve been living with low-grade vaginal infections for months, sometimes years, because they’ve been told their symptoms are “normal” or “just how bodies are.”
I’ve lost count of how many patients have sat in my consultation room and apologised for “making a fuss” about symptoms that have been affecting their quality of life, their intimate relationships, and their mental wellbeing for extended periods. They’ve been conditioned to believe that vaginal discomfort is something to tolerate rather than investigate.
The truth is that persistent or recurrent vaginal infections are rarely just bad luck. They’re almost always pointing to an underlying pattern: antibiotic use that’s repeatedly wiping out beneficial bacteria, uncontrolled diabetes affecting immune function, hormonal changes from contraception or perimenopause, or practices like douching that disrupt the vaginal ecosystem.
I’ve also seen the relief on women’s faces when we finally identify what’s been causing their symptoms and implement a treatment plan that actually works. Vaginal health directly affects your confidence, your comfort in your own body, and your ability to enjoy intimacy without anxiety or pain. These aren’t trivial concerns. They’re fundamental to your wellbeing.
When to See a Specialist
You should book an appointment with a gynaecologist or sexual health clinic if you experience any unusual vaginal discharge, odour, or itching that persists for more than 48 hours, even if symptoms are mild. Early intervention prevents complications and speeds recovery.
If you notice a fishy odour alongside grey discharge, book an appointment within one week with a GP or sexual health clinic for bacterial vaginosis testing. Left untreated, BV increases your risk of acquiring sexually transmitted infections and can affect pregnancy outcomes if you’re trying to conceive.
Any woman experiencing pain during intercourse that has appeared recently or worsened over the past few weeks should see a gynaecologist within two weeks. Painful sex has multiple possible causes, and proper examination is essential to identify whether infection, pelvic inflammatory disease, endometriosis, or another condition is responsible.
If you develop abnormal bleeding or spotting between periods, particularly alongside unusual discharge or pain during sex, book an urgent gynaecology appointment within one week. While often infection-related, irregular bleeding requires thorough investigation to rule out other causes.
Women who experience recurrent vaginal infections, defined as three or more episodes within 12 months, should request a referral to a gynaecologist with expertise in vulvovaginal disorders. Recurrent infections suggest an underlying issue, whether hormonal, immunological, or related to resistant organisms, that requires specialist assessment beyond standard treatment protocols.
If you’re pregnant and experiencing any symptoms of vaginal infection, contact your midwife or obstetrician within 24 hours. Untreated vaginal infections during pregnancy are associated with preterm birth, low birth weight, and other complications, and require prompt treatment with pregnancy-safe medications.
Your Next Steps
If you’ve recognised yourself in any of these warning signs, the most important thing you can do right now is this: book a medical appointment and resist the temptation to self-diagnose or self-treat.
Over-the-counter treatments for yeast infections have their place, but only if you’re certain you’re dealing with a yeast infection and not bacterial vaginosis or trichomoniasis. Using antifungal treatment for BV, for instance, won’t help and may delay proper care.
Your vaginal health deserves the same attention and respect you’d give to any other aspect of your wellbeing. These symptoms aren’t trivial, they’re not shameful, and they’re absolutely not something you should just learn to live with.
The right treatment, properly administered after accurate diagnosis, can resolve most vaginal infections within days to a week. You don’t have to continue managing symptoms, avoiding intimacy, or feeling uncomfortable in your own body.
Start by making that appointment. Be specific about your symptoms when you speak to the receptionist or triage nurse. Mention the duration, the specific changes you’ve noticed, and any factors that make symptoms better or worse. This information helps ensure you’re seen by the right clinician with adequate appointment time for proper examination.
Share this article with a friend who’s been struggling with these symptoms and doesn’t know where to start. Sometimes the hardest part is simply knowing you’re not alone and that help is available.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before making any changes to your health or treatment plan.