9 Shocking Reasons You Keep Having Miscarriages — And The 3 Life-Saving Tests Every Woman Needs Immediately
You did everything right. And you still lost the pregnancy. Again.
If that sentence landed somewhere deep in your chest, this article was written for you.
Introduction: You Are Not Alone, and You Are Not Broken
Recurrent miscarriage, medically defined as two or more pregnancy losses, is one of the most emotionally devastating experiences a person can go through. The grief is real. The confusion is real. And perhaps the most painful part of all is the silence. The not knowing why.
Here is something your doctor may not have said out loud: most cases of recurrent pregnancy loss are diagnosable. Many are treatable. And with the right testing and specialist care, the majority of women who have suffered repeated losses go on to have successful pregnancies.
The problem is that millions of women never get those tests. They are sent home after each loss with a sympathetic nod and the vague reassurance that “it happens.” They are told to “try again.” They are never given the roadmap that actually exists, the one that explains what is happening inside their bodies and what can be done about it.
That roadmap is what this article is. We are going to walk through nine medically documented reasons why miscarriages keep happening, and then we are going to get specific about the three categories of testing that every woman experiencing recurrent pregnancy loss deserves to have immediately.
This is not a substitute for professional medical advice. It is the informed starting point you deserve before you walk into your next appointment.
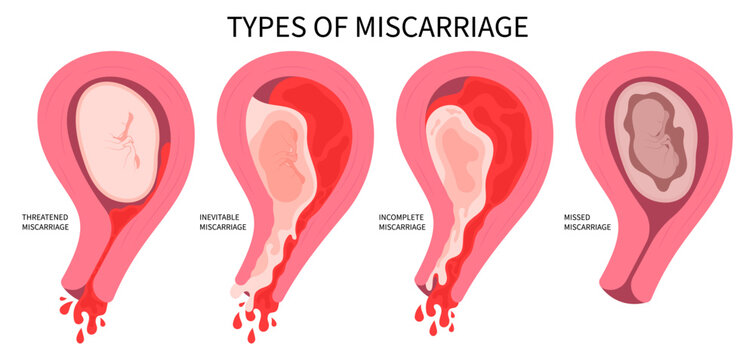
Reason #1: Chromosomal Abnormalities Are the Silent Culprit Behind Most Recurrent Miscarriages
When an embryo forms, it receives chromosomes from both partners. Sometimes, through no one’s fault and for no controllable reason, that process goes wrong. The embryo ends up with too many chromosomes, too few, or a rearrangement that cannot sustain life.
This is called aneuploidy, and it is staggeringly common. According to research published on NCBI’s Recurrent Pregnancy Loss resource, chromosomal abnormalities are involved in up to 80% of all spontaneous miscarriages that occur before ten weeks of gestation. That is not a small number. That is the majority.
What makes this particularly heartbreaking is that random chromosomal errors are exactly that: random. They are not caused by stress, diet, exercise, or anything you did. They happen during the earliest cell divisions, before most women even know they are pregnant.
However, a small subset of couples who experience recurrent losses carry what is called a chromosomal translocation. This is a structural abnormality present in one of the partners where a segment of one chromosome attaches to another. The person carrying the translocation is typically healthy and symptom-free, but their eggs or sperm carry a high rate of chromosomal imbalance. This is not random. This is a pattern, and it is something that can be identified through genetic testing.
Key points about chromosomal causes:
- Random aneuploidy becomes more common as maternal age increases, particularly after 35
- A balanced translocation in either partner can cause recurrent losses even when both individuals appear perfectly healthy
- Testing products of conception after a miscarriage can confirm whether chromosomes were involved
- This finding does not close the door to pregnancy; it opens the door to targeted solutions like IVF with preimplantation genetic testing
Reason #2: Uterine Structural Problems Silently Interfere With Recurrent Pregnancy Success
Think of the uterus as a home you are preparing for a new occupant. If the walls have a structural flaw, a shelf in the wrong place, a room that cannot be properly ventilated, the environment cannot support healthy development no matter how perfect the occupant is.
Structural abnormalities in the uterus are a well-established cause of recurrent miscarriage. These can include uterine fibroids, polyps, adhesions (bands of scar tissue, often called Asherman’s syndrome), and a uterine septum, which is a wall of tissue dividing the uterine cavity in two.
A uterine septum is particularly sneaky. It is present from birth, meaning many women never know they have it until they start trying to have children. The septum has a poor blood supply, so an embryo that implants on or near it often cannot develop properly. Studies suggest that a septum may be responsible for up to 35% of second-trimester losses, and the good news is that it is surgically correctable with a minimally invasive procedure.
Fibroids and polyps are also worth investigating carefully. Submucosal fibroids, those that protrude into the uterine cavity, are the most likely to interfere with implantation and fetal development. These too can often be removed surgically, with studies showing improved pregnancy outcomes afterward.
Structural issues to ask your doctor about:
- Uterine septum (congenital division of the uterine cavity)
- Submucosal fibroids (fibroids growing inside the uterine lining)
- Endometrial polyps (small growths on the uterine lining)
- Intrauterine adhesions or Asherman’s syndrome (scar tissue from prior procedures)
- Cervical insufficiency (a weak cervix that opens too early, usually causing second-trimester losses)
Reason #3: Antiphospholipid Syndrome Is a Treatable Cause of Recurrent Miscarriage That Is Frequently Missed
This is one of the most important causes of recurrent pregnancy loss that many women have never heard of. Antiphospholipid syndrome, sometimes abbreviated as APS or APLS, is an autoimmune condition in which the body produces antibodies that attack certain proteins in the blood, leading to an increased tendency to form blood clots.
During pregnancy, these clots can form in the tiny blood vessels of the placenta. The placenta is the lifeline between mother and baby, delivering oxygen and nutrients. When that flow is disrupted by clotting, the pregnancy cannot survive.
Research cited by the National Center for Biotechnology Information suggests that antiphospholipid syndrome accounts for somewhere between 8% and 42% of cases of recurrent pregnancy loss. That wide range reflects the variation in how strictly the syndrome is defined, but even at the lower estimate, it is a significant contributor.
Here is why this matters so much: APS is one of the most treatable causes of recurrent miscarriage. A combination of low-dose aspirin and a blood-thinning medication called heparin, taken during pregnancy, has been shown to dramatically improve live birth rates in women with APS. According to ACOG, this treatment can meaningfully raise the chances of a successful pregnancy for women who would otherwise face repeated losses.
You will not know you have it unless you are tested for it. The test is a simple blood draw.
Signs that APS might be involved:
- Miscarriages occurring after the first trimester (past ten weeks) are particularly suggestive
- A history of blood clots elsewhere in the body
- A known autoimmune condition such as lupus
- Miscarriages accompanied by low platelet counts or unusual blood test results
Reason #4: Thyroid Disorders Are a Surprisingly Common Driver of Recurrent Pregnancy Loss
The thyroid is a small, butterfly-shaped gland in your neck, and it quietly controls an enormous amount of your body’s function. During pregnancy, its role becomes even more critical. The developing fetus depends entirely on maternal thyroid hormone in the first trimester before its own thyroid becomes functional.
Both an underactive thyroid (hypothyroidism) and an overactive thyroid (hyperthyroidism) are associated with recurrent miscarriage. Hypothyroidism is more commonly linked to pregnancy loss, and it is more common than most people realize. Millions of women live with subclinical hypothyroidism, meaning their levels are abnormal but not dramatically so, and many of them have no symptoms at all.
Even more significantly, thyroid antibodies can cause problems even when thyroid hormone levels look normal on a standard test. Women who carry thyroid peroxidase antibodies have an elevated risk of miscarriage, and some studies suggest that treating with thyroid medication even when levels appear borderline may improve pregnancy outcomes.
The takeaway is this: a complete thyroid panel, not just a basic TSH test, is essential for any woman experiencing recurrent pregnancy loss. This means TSH, Free T4, Free T3, and thyroid antibody levels.
Why thyroid function matters so much in early pregnancy:
- The fetus relies on maternal thyroid hormone for brain and nervous system development in the first trimester
- Thyroid abnormalities are easily treated with medication that is safe during pregnancy
- Standard thyroid screening often misses subclinical cases, so requesting a full panel is important
- Optimal TSH levels for pregnant women are different from the standard reference range, so a specialist in reproductive endocrinology can provide more targeted guidance
Reason #5: Uncontrolled Diabetes Significantly Elevates the Risk of Recurrent Miscarriage
Diabetes is well known for its effects on overall health, but its connection to pregnancy loss is less widely discussed. Both Type 1 and Type 2 diabetes, when poorly controlled, are associated with significantly increased rates of miscarriage.
The mechanism here involves elevated blood sugar levels creating a hostile environment for early embryonic development. High glucose can affect implantation, impair placental development, and contribute to fetal chromosomal abnormalities. The good news is that well-controlled diabetes, achieved through careful blood sugar management before and during pregnancy, can bring miscarriage risk down to near-normal levels.
Insulin resistance, even without a full diagnosis of Type 2 diabetes, is also relevant. Polycystic ovary syndrome (PCOS) is a common condition that causes insulin resistance, hormonal imbalances, and elevated androgen levels. Women with PCOS have a higher rate of miscarriage, and managing the insulin resistance component through lifestyle changes or medication can make a meaningful difference.
If you have been diagnosed with PCOS, or if you have a family history of diabetes, flagging this with your reproductive specialist is essential.
Reason #6: Progesterone Deficiency Prevents the Uterine Lining From Supporting a Healthy Pregnancy
Progesterone is often called the “pregnancy hormone” because its role in early gestation is foundational. After ovulation, progesterone transforms the uterine lining into a thick, nutrient-rich environment ready to receive and support an embryo. In early pregnancy, it continues to maintain that environment until the placenta takes over production, typically around the end of the first trimester.
When progesterone levels are insufficient, a condition sometimes called luteal phase defect, the uterine lining may not be adequately prepared for implantation. Even if implantation occurs, it may not be sustained. The embryo essentially loses its support system.
Progesterone supplementation, taken in the form of capsules, suppositories, or injections, has been used to support early pregnancies for decades. Research on its effectiveness in unexplained recurrent miscarriage has been mixed, but for women with documented low progesterone or luteal phase defect, supplementation is a standard and reasonable intervention.
How to approach progesterone concerns:
- Ask your doctor to check progesterone levels seven days after ovulation to assess luteal phase function
- Mention any history of short cycles, light periods, or spotting in early pregnancy, all of which can suggest low progesterone
- Discuss whether progesterone supplementation from ovulation or from a positive pregnancy test might be appropriate in your case
Reason #7: Blood Clotting Disorders Beyond APS Can Quietly Cause Recurrent Pregnancy Loss
Antiphospholipid syndrome gets most of the attention in discussions of clotting-related miscarriage, but it is not the only clotting disorder that matters. Inherited thrombophilias, genetic variations that affect how the blood clots, are also linked to pregnancy loss in some women.
Conditions like Factor V Leiden mutation, prothrombin gene mutation, and protein S or protein C deficiencies are examples of inherited thrombophilias. These conditions increase the risk of blood clots forming in the placenta, which can restrict blood flow to the fetus and result in pregnancy loss, particularly in the second trimester.
It is worth noting that the scientific community has ongoing debate about how strongly inherited thrombophilias are linked to first-trimester losses versus later losses. The evidence for second-trimester pregnancy loss is more consistent. Nonetheless, for women with a personal or family history of blood clots, or those who have experienced losses after the first trimester, thrombophilia testing is a reasonable and informative step.
Reason #8: Immunological Factors and Natural Killer Cell Activity May Disrupt Implantation
This area of reproductive medicine is evolving rapidly, and it sits at the more cutting-edge end of recurrent miscarriage research. The immune system’s role in pregnancy is paradoxical: the body must tolerate a fetus, which is genetically half foreign, while still defending against genuine threats. When that tolerance breaks down, pregnancy loss can result.
Natural killer (NK) cells are a component of the immune system found in elevated concentrations in the uterine lining of some women with recurrent miscarriage. The theory is that excessively active NK cells may attack the developing embryo or interfere with the formation of new blood vessels needed to sustain the placenta.
Testing for uterine NK cells involves an endometrial biopsy, and treatment options including immunosuppressive medications and intravenous immunoglobulin (IVIG) are being explored. However, it is important to be realistic: this field is still developing, and not all proposed treatments have strong evidence behind them yet.
If you have had multiple losses that remain unexplained after standard testing, asking a reproductive immunologist about immune-related testing is a reasonable next step, but one that should come after the more established investigations.
Reason #9: Lifestyle Factors and Environmental Influences Have a Real and Often Underestimated Impact
This section requires some care, because the last thing anyone grieving a pregnancy loss needs is to feel blamed for something they could not control. That is not what this is about.
The reality is that certain modifiable factors do meaningfully affect miscarriage risk, and addressing them is an act of self-care and empowerment, not self-blame.
Research has linked the following to an increased risk of recurrent pregnancy loss:
- Cigarette smoking: Affects how the placenta develops and implants
- Alcohol consumption: Even moderate intake of three to five drinks per week has been associated with elevated risk in some studies
- High caffeine intake: More than three cups of coffee per day appears to increase risk
- Obesity: Independently associated with recurrent pregnancy loss in women who conceive naturally; this link is partly explained by the insulin resistance and hormonal disruption that excess weight can cause
- Significant underweight or nutritional deficiency: Can disrupt hormonal balance and uterine function
Additionally, environmental exposures to certain chemicals, heavy metals, and toxins have been studied in relation to miscarriage risk. While this research is still developing, minimizing known environmental exposures during preconception and early pregnancy is a sensible precaution.
The point is not perfection. It is information. Knowing these factors means you can discuss them honestly with your doctor and make adjustments where possible while pursuing the medical investigation you deserve in parallel.
The 3 Essential Test Categories Every Woman With Recurrent Miscarriage Needs
Now we get to the practical part. If you have experienced two or more miscarriages, the American College of Obstetricians and Gynecologists recommends a thorough evaluation. Here are the three major categories of testing that should be part of that workup.
Test Category 1: Genetic and Chromosomal Evaluation
This encompasses testing of both partners as well as, ideally, any pregnancy tissue from a previous loss.
Parental karyotyping is a blood test that maps the chromosomes of both the woman and her partner. It can identify balanced translocations or other structural chromosomal abnormalities that, while causing no symptoms in the carrier, can result in chromosomally abnormal pregnancies.
Genetic analysis of pregnancy tissue (also called products of conception testing) identifies whether a specific loss was caused by a chromosomal problem. This is valuable both for understanding what happened and for determining whether losses appear to be random or patterned.
If chromosomal issues are identified, genetic counseling can map out a path forward that may include IVF with preimplantation genetic testing, which allows embryos to be screened before transfer.
Test Category 2: Uterine and Structural Imaging
The uterus must be evaluated thoroughly. A basic pelvic ultrasound is not sufficient. The gold-standard tests for this category include:
Hysterosalpingogram (HSG): An X-ray procedure where dye is injected into the uterine cavity to outline its shape and check for abnormalities in the fallopian tubes.
Sonohysterogram (SHG): A saline infusion ultrasound that provides an excellent view of the inside of the uterine cavity. It is particularly good at identifying polyps, fibroids, and septa.
3D Ultrasound or MRI: When standard imaging is inconclusive, three-dimensional ultrasound or pelvic MRI can provide a more detailed view of uterine anatomy, including congenital abnormalities.
Hysteroscopy, a procedure where a camera is inserted into the uterine cavity, is both diagnostic and potentially therapeutic, allowing the doctor to identify and sometimes immediately treat structural problems in the same procedure.
Test Category 3: Comprehensive Blood Work Panel
This is the largest and most varied category. A thorough blood panel for recurrent pregnancy loss should include:
Antiphospholipid antibody panel: Tests for lupus anticoagulant, anticardiolipin antibodies, and anti-beta2 glycoprotein antibodies. Note that to diagnose APS, the positive result must be confirmed on two occasions at least twelve weeks apart.
Complete thyroid panel: TSH, Free T4, Free T3, and thyroid peroxidase antibodies (anti-TPO). Requesting antibody testing specifically is important, as many standard thyroid screenings only measure TSH.
Hormonal assessment: Progesterone (checked in the luteal phase), FSH, LH, estradiol, AMH (anti-Mullerian hormone, which assesses ovarian reserve), and prolactin.
Blood glucose and insulin: Particularly relevant if PCOS, obesity, or a family history of diabetes is present.
Thrombophilia panel: Including Factor V Leiden, prothrombin gene mutation, protein C, protein S, and antithrombin III. This is most relevant for losses occurring after the first trimester or in women with personal or family history of clotting disorders.
Comparative Overview: Recurrent Miscarriage Causes, Tests, and Treatability
| Cause | Estimated Contribution | Primary Test | Treatable? |
|---|---|---|---|
| Chromosomal abnormality (random aneuploidy) | Up to 50% of all losses | Products of conception testing | Not preventable, but IVF with PGT is an option |
| Parental chromosomal translocation | 2-5% of couples with RPL | Parental karyotyping | Yes — PGT or donor gametes |
| Uterine structural abnormality | 10-15% of RPL cases | Sonohysterogram / Hysteroscopy | Often yes, with surgery |
| Antiphospholipid syndrome | 8-42% of RPL cases | APS antibody panel | Yes — aspirin + heparin |
| Thyroid disorder | Significant contributor | Full thyroid panel + antibodies | Yes — thyroid medication |
| Uncontrolled diabetes / PCOS | Meaningful contributor | Blood glucose, insulin, hormones | Yes — blood sugar management |
| Progesterone deficiency | Contested but relevant | Day 21 progesterone test | Yes — progesterone supplementation |
| Inherited thrombophilias | Primarily second-trimester losses | Thrombophilia panel | Yes — anticoagulants during pregnancy |
| Immunological (NK cells, etc.) | Emerging research area | Endometrial biopsy (specialist) | Emerging — treatments still being studied |
| Lifestyle factors | Compounding risk factor | Medical history and discussion | Yes — lifestyle modification |
What Happens If No Cause Is Found?
It is worth addressing this directly, because it happens in a significant portion of cases.
Even after a thorough investigation, the cause of recurrent pregnancy loss cannot be identified in roughly half of all cases. This is called unexplained recurrent pregnancy loss, and living with that uncertainty is genuinely difficult.
Here is the most important thing to know about unexplained RPL: the outlook is still hopeful. According to the American College of Obstetricians and Gynecologists, about 65 out of 100 women with unexplained recurrent pregnancy loss go on to have a successful pregnancy without any specific treatment. That number is real, and it matters.
Additionally, the category of “unexplained” is shrinking as research advances. Immunological testing, more sensitive genetic analysis, and better evaluation of endometrial function are all expanding the range of what can be detected and addressed.
The absence of a diagnosis is not the same as the absence of hope.
Finding the Right Care After Recurrent Pregnancy Loss
General practitioners and even general OB-GYNs, while compassionate and skilled, are not always equipped to conduct the full workup that recurrent miscarriage requires. Asking for a referral to a reproductive endocrinologist or a specialist recurrent pregnancy loss clinic is entirely appropriate and, frankly, essential.
In the United Kingdom, the NHS guidelines recommend referral to a specialist miscarriage clinic after three losses. In the United States, many reproductive specialists will begin a workup after two losses, and the ACOG supports this approach.
You do not need to wait. You do not need to prove yourself by losing another pregnancy. You are entitled to answers.
If your current doctor is not taking your concerns seriously, seek a second opinion. A good specialist will welcome your questions, order a comprehensive panel, and work with you to understand your individual picture rather than offering vague reassurance.
The Emotional Reality Nobody Prepares You For
A medical article can give you information, but it cannot fully honor what you have been through. Recurrent miscarriage is grief layered on top of grief, often in silence, often without the acknowledgment that a later pregnancy loss would receive.
The mental health toll is real and well-documented. Women experiencing recurrent pregnancy loss report rates of anxiety and depression comparable to those facing serious chronic illness. This is not weakness. This is the weight of love meeting loss, over and over again.
Please do not carry it alone. Seeking psychological support alongside medical investigation is not a luxury. It is part of comprehensive care. Many recurrent pregnancy loss clinics now incorporate counseling as a standard part of their program. Peer support groups, both in person and online, connect you with others who understand in ways that even the most caring friends may not.
You are not broken. You are navigating something genuinely hard, and you deserve both answers and support.
Conclusion: Knowledge Is the First Step Toward a Different Outcome
Recurrent miscarriage is not a sentence. It is a signal. A signal that something in the complex, intricate process of creating a pregnancy is not working as it should, and that with the right investigation, there is a real chance of finding out what that something is.
The nine causes we explored here, chromosomal abnormalities, uterine structure, antiphospholipid syndrome, thyroid dysfunction, diabetes and insulin resistance, progesterone deficiency, clotting disorders, immune factors, and lifestyle influences, each represent a doorway. Behind some of those doors is a treatable problem and a path forward.
The three testing categories, genetic evaluation, uterine imaging, and comprehensive blood work, are not exotic or experimental. They are established, accessible, and often covered by insurance when a physician documents recurrent pregnancy loss.
The most important thing you can do right now is walk into your next appointment armed with specific questions. Ask for a referral to a specialist. Ask for a comprehensive workup. Ask what tests have not yet been done.
You have earned the right to a real answer.
Take the Next Step
Share this article with someone navigating recurrent miscarriage who deserves the information, grief is heavier when it is carried without context.
Read Next:
- What to Say (and Not Say) to Someone Who Has Had a Miscarriage
- IVF With Preimplantation Genetic Testing: A Plain-Language Guide
- How to Talk to Your Doctor About Recurrent Pregnancy Loss (Script Included)
Drop a comment below: Have you been through a recurrent loss workup? What did you wish you had known sooner? Your experience might be exactly what someone else needs to hear.
This article is intended for informational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider regarding your individual circumstances.