5 Alarming Signs Your Estrogen Levels Are Critically High
Your body has been trying to tell you something. The bloating that never fully goes away, the periods that leave you bedridden, the mood swings that feel nothing like you — these are not random complaints, and they are definitely not all in your head.
They could be signs that your estrogen levels have gone dangerously off the rails.
What High Estrogen Actually Means (And Why Your Doctor Might Have Missed It)
Before diving into the warning signs, it helps to understand what “high estrogen” actually means in practice.
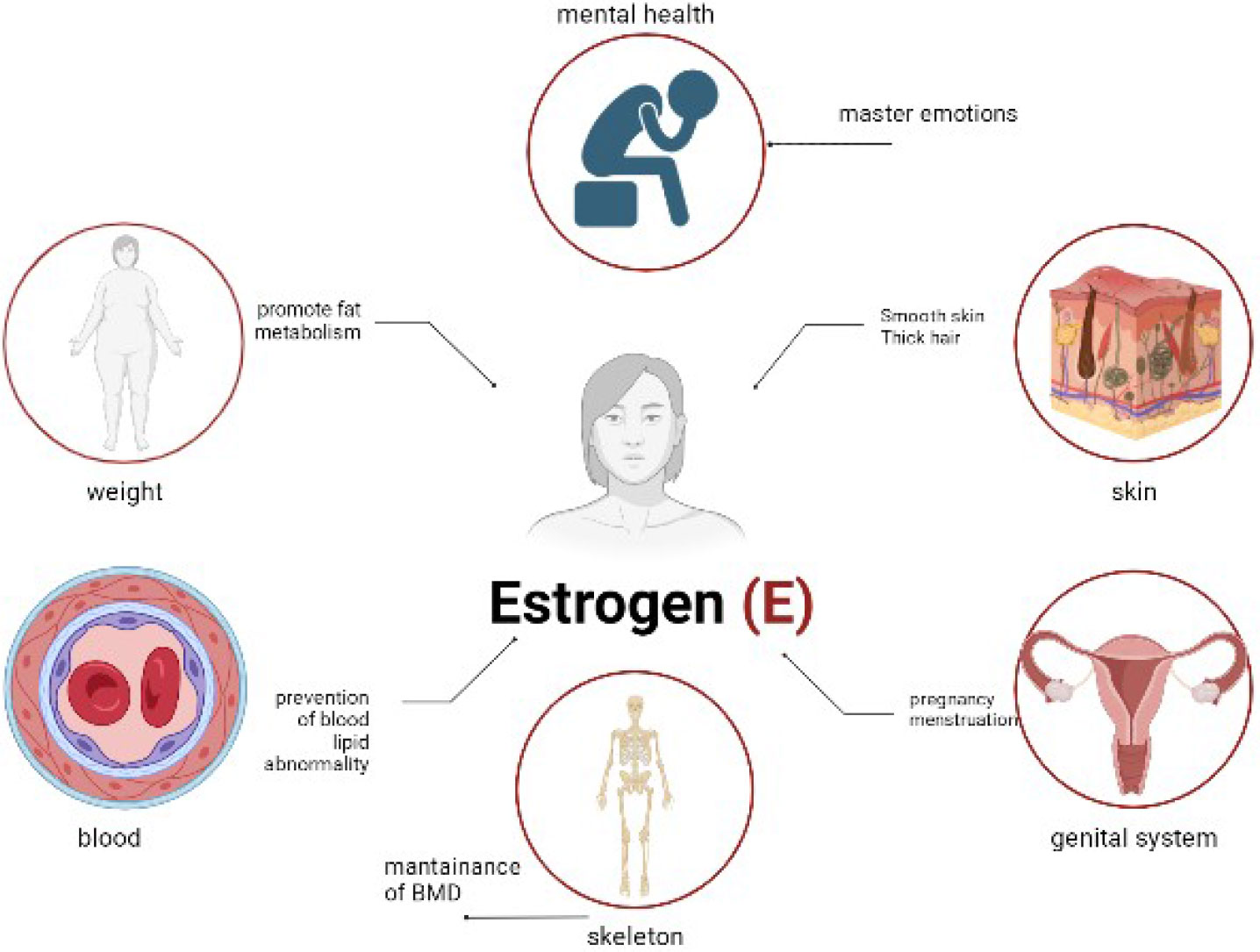
Estrogen is one of the body’s most powerful hormones. It drives puberty, regulates the menstrual cycle, supports bone density, protects cardiovascular health, and even influences how you sleep and how you feel emotionally. In a healthy, balanced body, estrogen rises and falls in a predictable rhythm across your monthly cycle, working in tandem with progesterone, its hormonal counterpart.
The problem starts when estrogen is consistently elevated above normal levels, or when progesterone drops too low to balance it out. This state, sometimes called estrogen dominance, can cause a cascade of symptoms that affect everything from your waistline to your mental health to your reproductive organs.
What makes this condition particularly tricky is that many of its symptoms are dismissed as normal parts of being a woman. “Of course periods are painful.” “Of course you’re emotional before your cycle.” “Of course you’re tired.” The normalization of these experiences means that many women walk around for years with critically unbalanced hormones and never connect the dots.
High estrogen is rarely caused by your body simply making too much on its own. More often, levels run high because of hormonal birth control, hormone replacement therapy, excess body fat (which produces its own estrogen), chronic stress (which suppresses the progesterone that should balance estrogen), poor liver function, or conditions like polycystic ovary syndrome (PCOS). Environmental exposure to xenoestrogens, synthetic compounds found in plastics, pesticides, and certain cosmetics, can also push levels higher over time.
The good news is that once you recognize the signs, you can act. And the earlier you act, the better your outcomes. So here are the five most dangerous signals your body sends when estrogen has climbed critically too high — each one important, and none that should be ignored.
Sign 1: Your Periods Have Become Heavier, Longer, or Completely Unpredictable — A Classic Red Flag of High Estrogen Levels
If your period has transformed from something manageable into a monthly ordeal that has you canceling plans and sleeping on a towel, high estrogen levels could be the culprit behind it all.
Here is the biology. Estrogen is responsible for building up the uterine lining during the first half of your cycle. It essentially lays down a thick, nourishing layer of tissue in preparation for a potential pregnancy. When estrogen levels are elevated beyond normal ranges, that lining becomes thicker than it should be. And when pregnancy does not occur, all of that excess lining sheds at once, resulting in heavier, longer, and often more painful periods.
Beyond the sheer volume of bleeding, women with high estrogen often notice:
- Clots larger than a quarter during their period
- Periods lasting longer than 7 days
- Spotting or breakthrough bleeding between cycles
- Cycles that arrive irregularly, sometimes closer together and sometimes further apart
- Severe cramping that does not respond well to standard over-the-counter pain relief
This is not just inconvenient. Heavy menstrual bleeding is a recognized medical concern that can lead to iron deficiency anemia, chronic fatigue, and a significantly reduced quality of life. It can also signal more serious underlying conditions that are directly linked to estrogen excess, including uterine fibroids and endometrial hyperplasia.
What You Should Do
Track your cycle carefully, including how many pads or tampons you use per day. If you are soaking through a pad or tampon every one to two hours, that is considered medically heavy and warrants a conversation with your doctor. A simple blood test measuring estradiol levels, along with a progesterone test, can help confirm whether estrogen imbalance is driving your symptoms.
Do not wait this one out. Persistent heavy bleeding that goes untreated is one of the most common pathways to diagnoses that could have been caught and managed much earlier.
Sign 2: You Are Gaining Weight in Specific Places — And High Estrogen Levels Are Likely Driving It
You have not changed your diet. You have not stopped exercising. But somehow, your hips, thighs, and lower belly are expanding in ways that feel almost impossible to explain. If this sounds like your reality, the problem may not be your lifestyle at all. It may be your hormones.
High estrogen levels promote fat storage, and they do so with a particular fondness for certain areas of the body. Estrogen stimulates the growth and proliferation of fat cells, especially in the regions where women naturally carry more adipose tissue, including the hips, thighs, buttocks, and lower abdomen. This is part of why estrogen-influenced body fat has sometimes been called “estrogenic fat.”
What makes this especially frustrating is the cyclical nature of the problem. Fat tissue, particularly around the belly and hips, is not metabolically passive. It actively produces its own estrogen through a process involving an enzyme called aromatase. So the more estrogen-driven fat you accumulate, the more estrogen your body generates, which then encourages more fat storage. It is a loop that can be maddeningly difficult to break through diet and exercise alone.
Beyond fat accumulation, high estrogen frequently causes water retention, which adds to the puffiness and bloating that many women experience. The body holds onto fluid when estrogen levels are elevated, which can make you feel heavy, swollen, and “puffy,” especially in the days leading up to your period.
Common estrogen-related weight and body composition changes include:
- Noticeable weight gain around the hips, thighs, and lower belly without dietary changes
- A persistent bloated or swollen sensation, especially before your cycle
- Clothing fitting differently even when your overall weight has not changed dramatically
- Difficulty losing weight despite consistent effort and caloric restriction
- A sense of feeling “puffy” in the face and hands
What You Should Do
If you are experiencing unexplained weight gain concentrated in estrogen-sensitive areas alongside other symptoms on this list, hormonal testing is a logical next step. A healthcare provider can order a comprehensive hormone panel that includes estradiol, progesterone, FSH, and LH to get a fuller picture of what is happening.
Reducing alcohol intake, increasing dietary fiber, and exercising regularly are all steps that support the liver in clearing excess estrogen from the body. But for many women, lifestyle changes alone are not sufficient without also addressing the underlying hormonal imbalance directly.
Sign 3: Your Mood Is a Rollercoaster — Because High Estrogen Levels Directly Hijack Your Brain Chemistry
One of the most underappreciated effects of high estrogen is what it does to your mental and emotional health. Many women with estrogen dominance describe feeling like a stranger in their own body — anxious without reason, irritable over small things, tearful in ways that feel disproportionate to the situation, or depressed in a heavy, foggy way that does not quite respond to the strategies that usually help.
This is not weakness. This is neurochemistry.
Estrogen interacts directly with the brain’s neurotransmitter systems, particularly serotonin and dopamine, the chemicals most closely associated with mood, motivation, and emotional regulation. In balanced amounts, estrogen actually supports healthy mood by boosting serotonin sensitivity. But when levels are consistently too high, or more precisely when estrogen is running unopposed because progesterone levels are too low in comparison, the system tips into dysregulation.
High estrogen has been linked to:
- Increased anxiety and a sense of being on edge without an obvious trigger
- Mood swings that intensify in the week before your period
- Depressive episodes that seem to track your menstrual cycle
- Brain fog, difficulty concentrating, and problems with memory
- Emotional sensitivity that feels heightened and hard to manage
- Irritability that escalates quickly and seems out of proportion
The relationship between estrogen and mood is particularly noticeable in the luteal phase of the cycle, the two weeks between ovulation and menstruation. During this time, progesterone should rise to counterbalance estrogen. When it does not, because progesterone is insufficient or estrogen is simply too elevated, the emotional symptoms of imbalance become most pronounced. For some women, this manifests as severe PMS. For others, it can look like premenstrual dysphoric disorder (PMDD), a clinically recognized and debilitating condition that goes well beyond ordinary premenstrual moodiness.
What You Should Do
If your emotional symptoms follow a clear cyclical pattern — getting worse in the two weeks before your period and improving once bleeding begins — that pattern itself is diagnostic information. Bring it to your doctor and ask specifically about hormone testing timed to different phases of your cycle, as a single blood draw may not capture the full picture of hormonal fluctuation.
Tracking your mood daily alongside your cycle using a journal or an app can help you see the pattern clearly and make a compelling case to your healthcare provider that hormones, not simply stress or personality, are at the root of what you are experiencing.
Sign 4: Your Breasts Are Tender, Swollen, or Developing Lumpy Tissue — A Tissue-Level Warning of Estrogen Overload
Breast tenderness before a period is common enough that most women dismiss it as an ordinary inconvenience. But when that tenderness becomes severe, constant, or accompanied by noticeable swelling and lumpy changes in breast tissue, it is your body communicating something more significant.
Estrogen is a primary driver of breast tissue development and proliferation. Breast cells have estrogen receptors throughout them, and when estrogen levels are elevated, those cells respond. The result is often swelling, soreness, and increased density of breast tissue. In cases of chronic high estrogen, some women develop fibrocystic breast changes, a condition involving the formation of noncancerous, fluid-filled lumps or dense, rope-like tissue within the breast.
According to Healthline’s overview of high estrogen symptoms, breast tenderness and swelling are among the most consistently reported physical signs of estrogen excess in women. Fibrocystic lumps, while not cancerous in themselves, can make it significantly harder to detect any potentially problematic changes during self-exams or routine mammograms.
What this sign looks like in practice:
- Breast tenderness that arrives earlier in the cycle than usual or persists throughout the month
- Noticeable swelling or fullness in the breasts, particularly in the outer and upper regions
- Dense, lumpy, or rope-like changes in breast tissue that were not previously present
- Pain that is disproportionate to what you would normally experience before your period
- Sensitivity so acute that a hug or sleeping on your stomach becomes genuinely uncomfortable
The Long-Term Stakes
This is where the conversation becomes more serious. Long-term exposure to elevated estrogen levels has been identified as a meaningful risk factor for hormone-receptor-positive breast cancer. The majority of breast cancers are estrogen-receptor positive, meaning they are fueled in part by estrogen’s stimulating effect on breast cells. Chronic overexposure to estrogen does not guarantee cancer, but it does create an environment in which the risk is elevated.
What You Should Do
Do not skip your breast self-exams, and do not assume tenderness or lumpiness is necessarily normal just because it happens regularly. Any new lumps, significant changes in breast tissue, or pain that disrupts daily functioning should be assessed by a healthcare provider. If you suspect high estrogen is a contributing factor, request a comprehensive hormone evaluation alongside any breast imaging your doctor recommends.
Sign 5: You Have Been Diagnosed with Fibroids, Endometriosis, or Ovarian Cysts — These Conditions Are Estrogen-Dependent
This fifth sign is arguably the most medically serious on this list, because it moves beyond symptoms and into diagnosed conditions that carry significant consequences for fertility, quality of life, and long-term health.
Uterine fibroids, endometriosis, and ovarian cysts are all conditions in which estrogen plays a central and causal role. They are often referred to by researchers as estrogen-dependent conditions, meaning estrogen is not just incidentally present but actively fueling their development and growth.
Uterine Fibroids
Uterine fibroids are benign tumors that grow within or around the uterus. They are remarkably common, with estimates from Johns Hopkins Medicine suggesting that up to 77% of women will develop fibroids at some point during their reproductive years. Research has shown that estrogen promotes fibroid growth by stimulating cell proliferation within uterine tissue. Fibroids tend to shrink after menopause, when estrogen levels naturally fall, which itself underscores the hormonal connection.
Symptoms of fibroids include:
- Heavy, prolonged, or painful periods (often overlapping with Sign 1)
- Pressure or fullness in the lower abdomen or pelvis
- Frequent urination if fibroids press against the bladder
- Lower back pain
- Pain during intercourse
- Complications with fertility and pregnancy
Endometriosis
Endometriosis is a painful condition in which tissue similar to the uterine lining grows outside the uterus, typically on the ovaries, fallopian tubes, and pelvic tissue. It affects roughly 10% of women of reproductive age worldwide, and it is deeply estrogen-dependent.
High estrogen levels fuel the growth and inflammation of endometrial lesions. Meanwhile, the lesions themselves can produce their own estrogen, creating another self-reinforcing cycle that makes endometriosis both harder to treat and harder to escape once it has taken hold.
Ovarian Cysts
Ovarian cysts, particularly functional cysts and those associated with PCOS, are also closely linked to estrogen excess and hormonal imbalance. When ovulation is disrupted, as it frequently is in the context of elevated estrogen or low progesterone, follicles that should have released eggs can instead persist as fluid-filled cysts on the ovary.
According to the Cleveland Clinic’s comprehensive guide to estrogen and hormone health, excess estrogen in the body is directly associated with conditions including polyps, fibroids, PCOS, and endometriosis pain, all of which can compound over time without appropriate treatment.
What You Should Do
If you have already been diagnosed with any of these conditions, they are not isolated gynecological bad luck. They are signals that your hormonal environment needs assessment and support. Work with your doctor to measure your estrogen and progesterone levels, evaluate your overall hormonal health, and explore both medical and lifestyle-based treatment options. Ignoring the hormonal root cause while only treating the structural symptom (removing fibroids, for example, without addressing estrogen excess) often results in recurrence.
How High Estrogen Levels Compare to Normal: A Reference Guide
Understanding where your numbers land requires context. The following table provides a general comparison of estrogen levels across different life stages, alongside the most common symptoms and associated conditions when levels exceed healthy ranges.
| Life Stage | Normal Estrogen Range (Estradiol) | Signs Estrogen Is Too High | Commonly Associated Conditions |
|---|---|---|---|
| Reproductive age (non-pregnant) | 15 to 350 pg/mL (varies by cycle phase) | Heavy periods, breast tenderness, mood swings, weight gain | Fibroids, endometriosis, PCOS |
| Perimenopausal | 10 to 200 pg/mL (fluctuating) | Irregular periods, bloating, insomnia, anxiety spikes | Estrogen dominance, fibrocystic breasts |
| Postmenopausal | Less than 10 to 30 pg/mL | Any significant estrogen symptoms (unusual in this stage) | Elevated cancer risk if persistent |
| On hormonal birth control | Varies widely by method | Mood changes, breast swelling, low libido, nausea | Medication-induced estrogen elevation |
| On hormone replacement therapy (HRT) | Provider-monitored | Breast tenderness, spotting, bloating | Risk increases with unopposed estrogen use |
Note: Reference ranges vary between laboratories and are always interpreted alongside clinical symptoms. A single blood test is rarely the whole picture. Hormone levels fluctuate throughout the menstrual cycle, and testing should ideally be timed appropriately for accurate results.
What Causes Estrogen to Climb Critically High in the First Place?
Understanding the “why” behind elevated estrogen levels is essential for treating the problem at its root rather than simply managing symptoms indefinitely.
The most common contributors to high estrogen include:
Hormonal medications. Estrogen-containing birth control pills, patches, rings, and certain forms of hormone replacement therapy are among the most common pharmaceutical causes of elevated estrogen levels. This does not mean you should stop your medication without medical guidance, but it does mean that if you are experiencing symptoms, your prescription deserves a second look.
Excess body fat. Adipose tissue, especially visceral fat around the abdomen, contains the enzyme aromatase, which converts androgens (male hormones) into estrogen. The more body fat present, particularly in the abdominal region, the more estrogen the body generates independent of the ovaries. This is one key reason estrogen dominance becomes more common with weight gain.
Chronic stress and cortisol. The stress hormone cortisol and progesterone share biochemical pathways. When the body is under sustained stress, it prioritizes cortisol production over progesterone. This effectively lowers progesterone levels, leaving estrogen relatively unopposed even if estrogen itself has not technically increased. The result is functionally similar to having high estrogen, because the counterbalancing force has been diminished.
Liver dysfunction. The liver is the primary organ responsible for metabolizing and clearing estrogen from the body. When liver function is compromised, whether due to alcohol consumption, poor diet, or conditions like fatty liver disease, the clearance of estrogen slows, allowing levels to accumulate.
Environmental xenoestrogens. Synthetic compounds found in plastics (particularly BPA), certain pesticides, and many conventional personal care products can mimic estrogen in the body, binding to estrogen receptors and producing estrogen-like effects. Reducing exposure to these compounds is an increasingly recommended element of hormonal health management.
PCOS and insulin resistance. Women with polycystic ovary syndrome often experience significant hormonal disruption, including elevated estrogen relative to progesterone. Insulin resistance, which frequently accompanies PCOS, also promotes aromatase activity and can contribute to higher estrogen levels.
How Doctors Test for and Treat High Estrogen Levels
If you recognize yourself in any of the signs described above, the path forward begins with getting tested. Here is a general overview of what the diagnostic and treatment process typically looks like.
Testing
A comprehensive hormone panel typically includes:
- Estradiol (E2): The most active and most commonly measured form of estrogen
- Progesterone: Measured to assess the ratio of progesterone to estrogen, which often matters more than estrogen in isolation
- FSH and LH: Hormones from the pituitary gland that regulate the ovarian cycle
- Testosterone: Often assessed alongside estrogen in women with PCOS or related conditions
- SHBG (sex hormone-binding globulin): A protein that binds hormones and affects how much is “free” and biologically active
Timing matters enormously. Testing estrogen on day 3 of your cycle versus day 21 will give you very different results, and both data points can be informative. An integrative or functional medicine physician may order more comprehensive testing, including a DUTCH test (dried urine test for comprehensive hormones), which measures hormone metabolites and gives a fuller picture of how your body is processing and clearing estrogen.
Treatment Options
Treatment depends entirely on the underlying cause of elevated estrogen. Common approaches include:
Lifestyle interventions. For many women, targeted lifestyle changes produce meaningful hormonal improvements. These include increasing dietary fiber (which supports estrogen excretion through the gut), reducing alcohol intake, maintaining a healthy weight, managing stress through evidence-based practices, and limiting exposure to plastics and xenoestrogens.
Nutritional support. Cruciferous vegetables like broccoli, cauliflower, and Brussels sprouts contain a compound called DIM (diindolylmethane) that supports healthy estrogen metabolism in the liver. Flaxseeds, high in lignans, may also help modulate estrogen activity.
Medication adjustments. If hormonal birth control or HRT is contributing to elevated estrogen, your doctor may recommend switching to a lower-estrogen formulation, a different method, or a progestin-dominant approach that better counterbalances estrogen’s effects.
Progesterone therapy. In cases of confirmed estrogen dominance where progesterone is low, supplementing with bioidentical or synthetic progesterone under medical supervision can help restore the hormonal balance and alleviate symptoms.
Addressing underlying conditions. If PCOS, obesity, insulin resistance, or liver dysfunction is fueling high estrogen, treating those root causes directly is an essential part of the solution.
Medications for specific conditions. For women with diagnosed estrogen-dependent conditions like endometriosis or uterine fibroids, a range of hormonal treatments, and in some cases surgery, may be recommended depending on severity and treatment goals.
The Long-Term Risks You Cannot Afford to Ignore
It is worth being direct about what happens when critically high estrogen levels go unaddressed over the long term. This is not about causing unnecessary fear. It is about giving you the honest picture so you can advocate for yourself.
Prolonged exposure to elevated estrogen, particularly when unopposed by adequate progesterone, is associated with:
Endometrial hyperplasia and uterine cancer. Estrogen continuously stimulates the growth of the uterine lining. Without progesterone to counteract this, the lining can become excessively thick, a condition called endometrial hyperplasia. Left untreated, certain types of hyperplasia can progress to endometrial cancer. Research from the National Cancer Institute has found that using unopposed estrogen for five or more years is associated with at least a twofold increase in endometrial cancer risk.
Breast cancer risk. The majority of breast cancers are estrogen-receptor positive, meaning they are responsive to and potentially fueled by estrogen. Long-term exposure to elevated estrogen levels does not cause breast cancer on its own, but it does create a hormonal environment that may contribute to cancer cell development and growth over time.
Blood clots and cardiovascular complications. High estrogen levels, particularly in the context of synthetic estrogen from certain hormonal medications, are associated with an increased risk of venous thromboembolism (blood clots in the veins). Elevated estrogen can affect clotting factors in the blood, making clots more likely to form.
Gallbladder disease. Higher estrogen levels are associated with increased cholesterol saturation in bile, which raises the risk of gallstone formation. Women already have a higher baseline risk of gallstones than men, and estrogen excess compounds that risk further.
None of these outcomes are inevitable. But they are all preventable or mitigable with early awareness and appropriate care. That is exactly why recognizing these signs early matters so much.
A Note About Estrogen Dominance Versus Simply “High Estrogen”
You may have noticed that this discussion has moved between two concepts: high estrogen and estrogen dominance. It is worth briefly clarifying the distinction.
Clinically, high estrogen refers to estrogen levels that are objectively elevated above the normal reference range for a woman’s age and cycle phase.
Estrogen dominance, while widely used in wellness and functional medicine circles, is a more nuanced concept. It refers to a state where estrogen is elevated relative to progesterone, even if estrogen itself falls within a “normal” range. The ratio matters because progesterone is what keeps estrogen’s effects in check. When progesterone is chronically low, and it frequently is in today’s stress-saturated, sleep-deprived world, even moderate estrogen levels can produce symptoms of excess.
This is part of why some women are told their estrogen is “normal” on a blood test and still experience every symptom on this list. The absolute number is only part of the story. The ratio of estrogen to progesterone, the way the body metabolizes estrogen, and the individual sensitivity of tissues to estrogen all play a role in how these symptoms manifest.
If you have been tested and told your levels are normal but your symptoms persist, it may be worth requesting a more comprehensive panel, asking specifically about the estrogen-to-progesterone ratio, or consulting with a provider who specializes in hormonal health.
Bringing It All Together: What Your Body Is Really Saying
Your body is not being dramatic. Your period is not supposed to be that heavy. Your mood is not supposed to swing that wildly. The weight around your hips that refuses to move is not just a lack of willpower. And the fatigue that drags you down even after a full night’s sleep is not just the pace of modern life.
These are messages. Specific, physiological, hormone-driven messages from a body that is working hard to tell you something is out of balance.
The five signs we have covered in this article, including heavy or irregular periods, unexplained weight gain, significant mood disruption, breast tenderness and fibrocystic changes, and the presence of estrogen-dependent conditions like fibroids or endometriosis, are not random or unrelated. They are different expressions of the same underlying problem, and they all point toward estrogen levels that have climbed too high without adequate hormonal counterbalance.
The most important thing you can take away from this article is not a sense of alarm. It is a sense of direction. If these signs resonate with your experience, you now have a clearer picture of what questions to ask, what tests to request, and what conversations to have with your healthcare provider.
Hormonal health is foundational health. When estrogen is balanced, the downstream benefits touch nearly every area of your life, including your energy, your emotional resilience, your reproductive health, your sleep, and your long-term disease risk. Getting there starts with recognizing that what you are experiencing has a name, and that it deserves real attention.
Your Next Steps
If you recognize three or more of the signs in this article, here is a simple action plan:
- Book a hormone panel. Ask your doctor to test estradiol, progesterone, FSH, LH, and SHBG. Request that timing be noted, as cycle-day context is important for interpretation.
- Track your symptoms for one full cycle. Note mood changes, bleeding volume, breast changes, energy levels, and bloating day by day. This data is invaluable at a medical appointment.
- Audit your lifestyle for estrogen amplifiers. Consider reducing plastic use, limiting alcohol, increasing cruciferous vegetables, and addressing chronic stress.
- Find the right provider. If your concerns are dismissed without testing, seek a second opinion. A gynecologist, endocrinologist, or integrative medicine physician with experience in hormonal health is your best ally here.
Did this article help you make sense of symptoms you have been experiencing? Share it with a friend who needs to hear this. And if you have navigated estrogen imbalance yourself, drop a comment below. Your experience might be exactly what someone else needs to read today.
This article is intended for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider for diagnosis, testing, and treatment of any hormonal or reproductive health concerns.

