7 Dangerous Vaginal Infection Signs Every Woman Must Recognize Immediately
Your body is trying to tell you something, and if you have been ignoring that unusual itch, strange smell, or discomfort “down there,” this article could change everything.
Vaginal infections are among the most common health conditions affecting women worldwide, yet they remain one of the most under-discussed, misunderstood, and dangerously delayed in diagnosis. Millions of women mistake the warning signs for something minor, dismiss them as temporary, or feel too embarrassed to bring them up with a doctor until the problem has already escalated into something far more serious.
Here is the truth: caught early, most vaginal infections are straightforward to treat, often resolved in a matter of days. Left unaddressed, they can spiral into pelvic inflammatory disease, fertility complications, chronic pain, and in some cases, become a gateway for more serious conditions including sexually transmitted infections and even cervical health problems.
This guide breaks down the seven most critical vaginal infection signs that every woman needs to recognize, understand, and act on immediately. No medical jargon. No shame. Just clear, honest information that could protect your health today.
1. Unusual Vaginal Discharge Is One of the First Vaginal Infection Signs to Watch
Vaginal discharge is completely normal. Every woman has it, and its consistency and volume naturally shift throughout the menstrual cycle. What is not normal is when that discharge changes color, texture, or smell in ways that feel unfamiliar to you.
Healthy discharge is typically clear to milky white, has a mild or neutral odor, and does not cause any irritation. The moment it starts looking yellow, green, gray, or chunky, your body is waving a red flag that something has changed in the vaginal environment.
What to watch for:
- Thick, white, cottage-cheese-like discharge, which is a hallmark sign of a yeast infection (candidiasis)
- Thin, grayish or white discharge with a strong fishy odor, which strongly suggests bacterial vaginosis (BV)
- Yellow or green discharge, especially if it is frothy or accompanied by itching, which can indicate trichomoniasis, a sexually transmitted infection
- Any discharge that is noticeably different from your personal baseline, even if it does not match a textbook description
Every woman’s body is different, and only you know what your “normal” looks like. Trust that internal knowledge. If something feels off, it probably is.
2. Persistent Vaginal Itching and Burning Are Classic Vaginal Infection Symptoms You Should Never Ignore
An occasional, brief itch is rarely cause for concern. But when the itching is persistent, intense, or accompanied by a burning sensation, especially during urination or sex, it is one of the clearest vaginal infection symptoms your body can produce.
Itching and burning in the vaginal area are caused by inflammation of the delicate vaginal tissues, usually triggered by an overgrowth of harmful bacteria or fungi, or by the introduction of a pathogen through sexual contact.
Common causes behind this symptom include:
- Yeast infections, caused by an overgrowth of Candida fungus, are the number one cause of vaginal itching and produce intense, uncomfortable burning sensations
- Bacterial vaginosis disrupts the natural lactobacilli balance, causing mild to moderate irritation that can worsen over time
- Contact dermatitis from scented soaps, douches, or synthetic underwear can mimic infection symptoms and sometimes make a true infection harder to identify
- Trichomoniasis, a parasitic STI, frequently causes severe itching, redness, and swelling in addition to discharge changes
According to the Centers for Disease Control and Prevention’s overview of vaginal health and top STI prevention resources, trichomoniasis alone affects an estimated 2.6 million Americans annually, and the majority of cases go undiagnosed because people assume the symptoms are something else entirely.
Do not power through persistent itching or burning with over-the-counter creams unless you have already been diagnosed. Self-treating the wrong infection can delay proper care and allow the real problem to worsen.
3. A Strong or Fishy Vaginal Odor Is a Tell-Tale Vaginal Infection Sign That Demands Attention
The vagina has a natural, mild scent that varies slightly throughout the menstrual cycle. That is completely normal. But a strong, unpleasant, or distinctly fishy odor, particularly one that intensifies after sex or during your period, is one of the most recognizable vaginal infection signs associated with bacterial vaginosis.
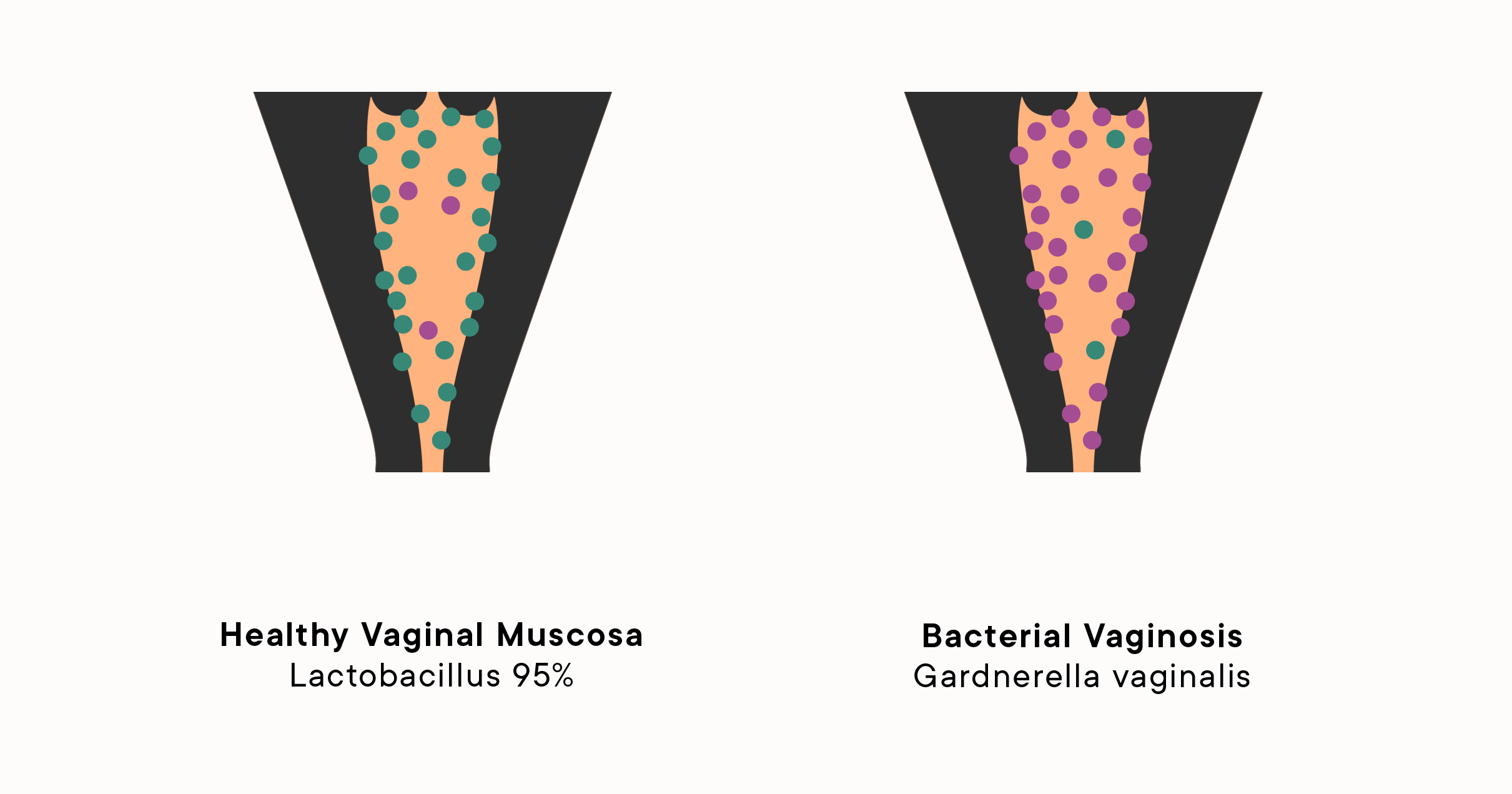
Bacterial vaginosis is the most common vaginal infection in women between the ages of 15 and 44. It occurs when the balance of bacteria in the vagina is disrupted, allowing harmful bacteria like Gardnerella vaginalis to overpopulate and crowd out the protective lactobacilli.
Why the odor gets worse after sex:
When semen, which is alkaline, comes into contact with the vaginal environment during BV, it temporarily raises the pH level. This creates a brief but noticeable spike in the fishy odor that many women describe as embarrassing and alarming. This is not a hygiene issue. It is a chemical reaction pointing to a medical condition.
Bacterial vaginosis left untreated increases the risk of contracting sexually transmitted infections, including HIV, and has been linked to preterm birth in pregnant women. It is also associated with pelvic inflammatory disease if bacteria travel upward into the uterus and fallopian tubes.
If you are noticing a smell that feels unfamiliar or stronger than usual, do not try to mask it with feminine deodorant sprays. Those products can actually worsen the imbalance. See a healthcare provider and get tested.
4. Pain or Discomfort During Sex Can Signal Serious Vaginal Infection Symptoms Worth Investigating
Sex should not hurt. While occasional discomfort can be linked to insufficient lubrication or stress-related tension, pain during penetration or after sex is one of the vaginal infection symptoms that often gets dismissed, minimized, or blamed on the wrong cause.
When a vaginal infection is present, the tissues inside and around the vagina become inflamed. They swell, become hypersensitive, and lose their natural resilience. Any friction against those tissues, even gentle friction, can produce sharp, burning, or aching pain that lingers well after the encounter ends.
What the pain can indicate:
- Yeast infections cause significant tissue inflammation, making even mild contact intensely uncomfortable
- Bacterial vaginosis and trichomoniasis both affect vaginal tissue health and can make sex painful or deeply unpleasant
- Chlamydia and gonorrhea, two common bacterial STIs that often present with minimal symptoms, can cause pelvic pain and discomfort during sex as the infection spreads internally
- Herpes outbreaks, which can be localized inside or near the vaginal opening, cause intense pain and burning that is often mistaken for another type of infection
If you are experiencing recurrent pain during sex, do not simply accept it as your normal. That conversation with your doctor, as awkward as it might feel, could catch something that is entirely treatable at this stage but becomes far more complicated if it spreads.
5. Vaginal Redness, Swelling, and Soreness Are Physical Vaginal Infection Signs You Can See and Feel
Vaginal infections do not stay internal. The physical signs often extend to the vulva, the external tissue surrounding the vaginal opening, and they are some of the most visible vaginal infection signs you can observe with a hand mirror or simply notice through touch and sensation.
Redness, puffiness, and tenderness in the vulvar area indicate that your immune system is actively responding to something it perceives as a threat. The increased blood flow to the area, part of the inflammatory response, causes that characteristic pink-to-red flushed appearance and the uncomfortable soreness that makes even sitting or walking feel irritating.
What you might notice:
- The labia minora or majora appear redder or more swollen than usual
- The skin around the vaginal opening feels tender to the touch, like a mild bruise
- Wearing tight underwear or pants becomes noticeably uncomfortable
- There is a general feeling of heat or warmth in the pelvic area that does not resolve
These physical signs become particularly important in cases of herpes, where small blisters or sores may appear on the vulva or vaginal tissue. Those sores can be easy to miss or confuse with ingrown hairs or razor irritation, especially during a first outbreak when you have no prior reference point.
Redness and swelling that appear alongside any other symptom on this list should be treated as a combination signal, meaning multiple signs appearing together almost always indicate that something requires medical evaluation.
6. Painful, Frequent, or Burning Urination Is a Vaginal Infection Symptom That Overlaps With Other Conditions
Here is where things get tricky. Painful or burning urination is most commonly associated with urinary tract infections (UTIs), and many women self-diagnose a UTI when they experience this symptom. But this is one of the vaginal infection symptoms that overlaps across several conditions, and misidentifying which one you have can lead to the wrong treatment and continued suffering.
When vaginal tissues are inflamed from an infection, urine passing over those irritated external tissues creates a sharp, burning sensation. This is sometimes called “external dysuria” and it is distinct from the internal burning of a classic UTI, though the two can coexist or be easily confused.
Conditions that cause this symptom:
- Yeast infections frequently cause external burning during urination, particularly when urine contacts the inflamed skin around the vaginal opening
- Trichomoniasis can cause urinary frequency and discomfort that mirrors a UTI almost perfectly
- Chlamydia and gonorrhea, when they affect the urethra, produce burning urination that most people assume is a UTI until testing reveals otherwise
- Herpes can cause extreme pain during urination if sores are present near the urethral opening
The danger here is assuming you know what you have based on one symptom. A positive yeast infection test from a pharmacy kit only rules in Candida. It does not rule out anything else. If you are experiencing urinary symptoms alongside any other sign from this list, see a healthcare provider for a full evaluation rather than treating one condition while another goes unaddressed.
7. Pelvic Pain or Pressure Is Among the Most Serious Vaginal Infection Signs and Should Never Be Delayed
All of the previous symptoms can be uncomfortable, disruptive, and even painful. But pelvic pain or pressure, especially if it is constant, worsening, or accompanied by fever, represents a significant escalation. This is the vaginal infection sign that most clearly suggests an infection has moved beyond the vaginal canal into deeper structures.
Pelvic inflammatory disease (PID) develops when bacteria, usually from an untreated bacterial vaginosis or STI like chlamydia or gonorrhea, migrate upward through the cervix into the uterus, fallopian tubes, and sometimes the ovaries. PID is one of the leading preventable causes of infertility in women worldwide.
Warning signs that suggest PID or serious infection spread:
- A dull, aching pain in the lower abdomen or pelvis that does not go away
- Pain that worsens during sex, particularly with deep penetration
- Fever above 38°C (100.4°F) combined with any vaginal symptoms
- Unusual bleeding between periods or after sex
- Nausea or vomiting alongside pelvic discomfort
- A general feeling of being unwell or run-down that coincides with vaginal symptoms
According to the World Health Organization’s essential facts on sexually transmitted infections and reproductive health complications, untreated STIs and related vaginal infections contribute to an estimated 17,000 cases of infertility in women each year in the United States alone. PID is the mechanism behind most of those cases.
If you are experiencing pelvic pain combined with fever, do not wait for a scheduled appointment. Go to an urgent care clinic or emergency room. This level of infection can escalate quickly, and early antibiotic treatment is the difference between full recovery and long-term complications.
Vaginal Infection Comparison: Symptoms, Causes, and Treatment Overview
Understanding which infection you may be dealing with helps you have a more informed conversation with your healthcare provider. Use this table as a reference guide, not a diagnostic tool.
| Infection Type | Common Discharge | Primary Symptoms | Typical Treatment | Risk If Untreated |
|---|---|---|---|---|
| Yeast Infection (Candidiasis) | Thick, white, cottage-cheese texture | Intense itching, burning, redness, swelling | Antifungal cream or oral fluconazole | Chronic recurrence, tissue damage |
| Bacterial Vaginosis (BV) | Thin, gray/white, fishy odor | Odor (worse after sex), mild itching, discharge | Oral or topical metronidazole or clindamycin | PID, increased STI susceptibility, preterm birth |
| Trichomoniasis | Frothy, yellow-green, strong odor | Itching, burning, painful urination, redness | Oral metronidazole or tinidazole | Increased HIV risk, pregnancy complications |
| Chlamydia | Usually none or mild increase | Often no symptoms, pelvic pain, burning urination | Oral azithromycin or doxycycline | PID, infertility, ectopic pregnancy |
| Gonorrhea | Yellow or green, increased volume | Burning urination, pelvic pain, spotting | Dual antibiotic therapy (ceftriaxone + azithromycin) | PID, infertility, systemic infection |
| Genital Herpes (HSV-2) | No discharge change | Blisters/sores, burning, painful urination | Antiviral therapy (acyclovir, valacyclovir) | Chronic outbreaks, neonatal transmission |
| Vulvovaginal Candidiasis (Recurrent) | Persistent thick white discharge | Chronic itching, burning, repeated episodes | Long-term antifungal suppression therapy | Significant quality-of-life impact, secondary skin damage |
Important note: Many of these infections, particularly chlamydia and gonorrhea, can be completely asymptomatic in early stages. Regular testing, not just symptom monitoring, is the only way to catch silent infections before they cause damage.
When to See a Doctor: Your Action Timeline for Vaginal Infection Signs
Timing matters enormously when it comes to vaginal infections. Here is a practical guide for when to seek care based on what you are experiencing.
See a Doctor Within 24 to 48 Hours If You Notice:
- Fever accompanying any vaginal symptoms
- Pelvic pain or pressure that is new or worsening
- Sores, blisters, or ulcers in or around the vaginal area
- Symptoms that are rapidly worsening rather than stable
Schedule an Appointment This Week If You Have:
- Discharge changes that have lasted more than a few days
- Persistent itching or burning that is not resolving on its own
- Pain during sex that has occurred more than once
- A strong or unfamiliar odor that has not changed after your period
Get Tested Regularly Even Without Symptoms If:
- You are sexually active with new or multiple partners
- You have a history of STIs or vaginal infections
- You are pregnant or trying to conceive
- You have a compromised immune system or are on antibiotics, steroids, or immunosuppressants
A full vaginal infection panel at your gynecologist or sexual health clinic typically takes minutes to complete and can identify bacterial, fungal, and viral causes with a high degree of accuracy. It is genuinely one of the most important health investments you can make in yourself.
Why Women Delay Treatment and Why That Needs to Change
The statistics around delayed treatment for vaginal infections are sobering. Studies consistently show that women wait an average of one to three months before seeking care for vaginal symptoms, often because of embarrassment, the assumption that it will resolve on its own, or a lack of access to healthcare.
Here is what that delay actually costs in practical terms.
A yeast infection caught early is a three-day antifungal course. Left for months, it can develop into chronic vulvovaginal candidiasis that requires months of suppressive therapy and significantly impacts quality of life.
Bacterial vaginosis treated promptly with a one-week antibiotic course resolves cleanly. Left untreated during pregnancy, it increases the risk of preterm labor and low birth weight.
Chlamydia treated in the acute stage with a single dose of antibiotics clears without a trace. Untreated chlamydia spreading into the fallopian tubes causes scarring that can result in ectopic pregnancy or permanent infertility.
The shame cycle around vaginal health is real and it is dangerous. Vaginal infections are not moral failures, they are medical events. They happen to women of every age, background, relationship status, and level of hygiene. A vaginal infection does not mean you did anything wrong. But not getting it treated might mean your body pays a price it did not need to.
Practical Prevention: Reducing Your Risk of Vaginal Infection
While no prevention strategy is foolproof, these evidence-based practices meaningfully reduce the frequency and severity of vaginal infections.
For day-to-day habits:
- Wear breathable, cotton underwear and avoid very tight clothing, which traps moisture and creates a hospitable environment for bacterial and fungal overgrowth
- Wipe front to back after using the bathroom to prevent fecal bacteria from entering the vaginal area
- Avoid douching entirely, the vagina is self-cleaning and douching disrupts its natural pH and bacterial balance
- Use fragrance-free soaps and intimate wash products, scented products are a leading cause of contact dermatitis and bacterial imbalance
- Change out of wet swimsuits and gym clothes promptly, yeast thrives in warm, moist environments
For sexual health:
- Use condoms consistently, they significantly reduce transmission risk for STIs including chlamydia, gonorrhea, trichomoniasis, and herpes
- Get tested for STIs regularly, and ask partners to do the same, particularly with new sexual relationships
- Urinate after sex to help flush bacteria from the urethra, reducing cross-contamination risk
For general immune and gut health:
- A diet rich in probiotics, including yogurt, kefir, and fermented foods, supports the growth of beneficial Lactobacillus bacteria that protect vaginal health
- Manage blood sugar levels carefully if you have diabetes or pre-diabetes, high glucose levels feed Candida overgrowth
- Avoid unnecessary antibiotic use, antibiotics kill beneficial vaginal bacteria alongside the pathogens they target, setting the stage for yeast infections
These habits are not complicated, but they are cumulative. Consistent practice over time dramatically lowers your baseline risk.
A Note on Recurrent Vaginal Infections: When to Dig Deeper
Some women experience vaginal infections repeatedly, sometimes four or more times per year. If that sounds familiar, the recurring infections are not bad luck and they are not just the way things are for you. Recurrent infections are a signal that something in the underlying environment needs to be investigated and addressed.
Potential underlying factors in recurrent vaginal infections include:
- Uncontrolled or undiagnosed diabetes, which fuels yeast overgrowth through elevated blood glucose
- Immune system conditions or medications that suppress immune function, including corticosteroids
- A partner who carries and reintroduces the infective organism, sometimes called a “ping-pong infection”
- Hormonal imbalances, including low estrogen during perimenopause or menopause, which thin vaginal tissues and alter pH
- Genetic predisposition to Candida overgrowth in some women
- Chronic antibiotic use for unrelated conditions that perpetually disrupts vaginal flora
If you are dealing with infections more than three times per year, ask your doctor about long-term suppressive therapy, a more comprehensive blood workup, and partner treatment if applicable. There is almost always an identifiable and addressable reason.
The Emotional Side of Vaginal Infection Signs: You Are Not Alone
It would be incomplete to address vaginal infections purely from a clinical standpoint without acknowledging the emotional toll they take. The discomfort is one layer. But beneath it, many women report feelings of embarrassment, shame, anxiety about relationships, and a deep discomfort with discussing the topic even with their own doctor.
Those feelings are valid. They are also shared by an enormous number of women. Bacterial vaginosis alone affects approximately 21 million American women each year. Yeast infections affect roughly 75 percent of women at least once in their lifetime. You are not the exception. You are in very large, very common company.
The best thing you can do for yourself is to normalize this conversation, at least in your own head and with your healthcare provider. Describe your symptoms accurately. Do not minimize them to avoid seeming dramatic. Do not embellish them out of anxiety. Just tell your doctor what you are experiencing and let them help you find the cause and the solution.
Your vaginal health is part of your overall health. It deserves exactly the same attention, care, and medical priority as every other system in your body.
Conclusion: Your Body Is Giving You Signals, Learn to Listen
The seven vaginal infection signs covered in this guide, unusual discharge, persistent itching and burning, strong odor, pain during sex, redness and swelling, painful urination, and pelvic pain, are not random. They are your body’s internal communication system working exactly as it should, sending increasingly clear messages that something in your vaginal environment has changed and needs attention.
The difference between a minor inconvenience and a serious complication often comes down to one thing: how quickly you respond to those signals.
You do not need to be a medical expert to protect your health. You need to know what normal feels like for your body, recognize when something deviates from that normal, and give yourself permission to seek care without guilt, delay, or second-guessing.
Early treatment is almost always faster, simpler, cheaper, and less physically demanding than treating an infection that has been given weeks or months to escalate. Your future self will be genuinely grateful that you acted today.
Ready to Take the Next Step?
Share this article with a woman in your life who deserves to have this information, your sister, your friend, your daughter. This is exactly the kind of knowledge that changes outcomes.
Talk to your doctor at your next appointment about scheduling a routine vaginal health panel, especially if you have noticed any of the signs discussed here.
Drop a comment below if you found this helpful or if there is a specific topic related to women’s vaginal health you would like us to cover next.
This article is intended for informational purposes only and does not constitute medical advice. Always consult a licensed healthcare provider for diagnosis and treatment.